 Non Celiac Gluten Sensitivity
Non Celiac Gluten Sensitivity
Over the last year, there has been major debate about whether or not non celiac gluten sensitivity (NCGS) exists. Now I know what many of you are already thinking…OF COURSE IT DOES! Just ask anyone without celiac disease who has had a dramatic change in health as a result of going gluten free.
I have personally seen more than 5,000 patients over the last 15 years. Many of them had previously tested negative for celiac disease and were told by their doctors to continue eating grain. The mass confusion on this issue has two origins.
- Flawed Diagnostic Lab Testing. Blood tests are aimed at identifying celiac disease. These blood tests are non comprehensive, non specific, and have a tendency to come back falsely negative. The truth is, even though there are over 400 different forms of gluten that have been identified, the blood tests only measure for the autoimmune reaction found in celiac disease, or a select few antibodies against a handful of gluten proteins found in wheat, barley, and rye. Even the most progressive labs like Cyrex only measure for a handful of different forms of gluten. The test that most GI doctors use as a gold standard (The Biopsy) is more often negative than positive. The reasons? Most people do not develop the classic villous atrophy of the small intestine associated with celiac disease. They have tissue damage in other areas of the body including the brain, liver, skin, muslces, and thyroid gland. Remember that a biopsy is an investigation of the small intestine that includes microscopic samples only. The actual surface area of the small intestine is roughly the size of a tennis court. Taking microscopic cross sections is hardly a comprehensive or definitive evaluation. In my personal experience, I have see as many as 9 negative biopsies in a row( over the course of many years) in the same patient before a 10th biopsy revealed a positive result. Were the first nine biopsy evaluations wrong or did the damage take years to manifest before a biopsy could reveal it?
- Under Educated Physicians: It is no mystery that gluten sensitivity is a nutritional problem. When you combine that fact with the sad reality that the average GI doctor receives less than 7 hours of nutritional study throughout medical school, it is not hard to understand why so many doctors casually dismiss gluten as a potential health threat. Add to this the fact that research in this area has exploded over the last decade. It is a challenge even for the most dedicated doctor to stay abreast of all of the new findings in this area. Unfortunately, the overwhelming majority of doctors are in gluten denial.
Research Confirms Gluten IS A PROBLEM (Again)
Even though the existence of non celiac gluten sensitivity has already been proven in other research, I feel like it is important to highlight the fact that other research groups continue to confirm non celiac gluten sensitivity. Another new study set out to identify whether or not gluten was a problem for those without diagnosed celiac disease. The study involved 61 adults who self reported that eating gluten caused them harm. This study was a randomized, double blind, placebo controlled trial. In case you weren’t aware, that means that this study meets the criteria for the highest scientific standard. What were the results?
When given hidden gluten, these patients reported multiple problems. The study summary is quoted below:
According to the per-protocol analysis of data from the patients who completed the trial, intake of gluten significantly increased overall symptoms compared with placebo (P=.034). Abdominal bloating (P=.040) and pain (P=.047), among the intestinal symptoms, and foggy mind (P=.019), depression (P=.020), and aphthous stomatitis (P=.025), among the extra-intestinal symptoms, were significantly more severe when subjects received gluten than placebo.
So to clarify, patients being exposed to gluten without knowing they were being exposed to gluten experienced increased:
- Abdominal bloating and pain
- Brain Fog
- Depression
- Mouth Ulcers
One could argue that bloating, brain fog, and depression are very subjective symptoms. Mouth ulcers on the other hand are physiochemical symptoms that cannot be blamed on a psychosomatic response.
Source: Clin Gastroenterol Hepatol. 2015 Feb 19
Why All the Confusion Around Non Celiac Gluten Sensitivity?
The biggest reason for all of the confusion has to do with a lack of knowledge. To date, there is no scientific consensus on the issue. If we break down what we do know, it might make more sense.
Gluten is not a single entity. Gluten refers to a family of proteins. To date thousands of gluten proteins have been identified. Most recently a study identified 400 new forms of gluten that are more damaging than the form of gluten doctors most commonly test for. There is NO LAB that tests for all of the different forms of gluten.
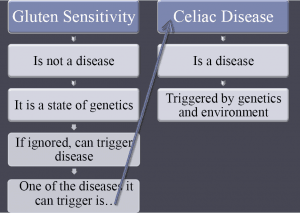
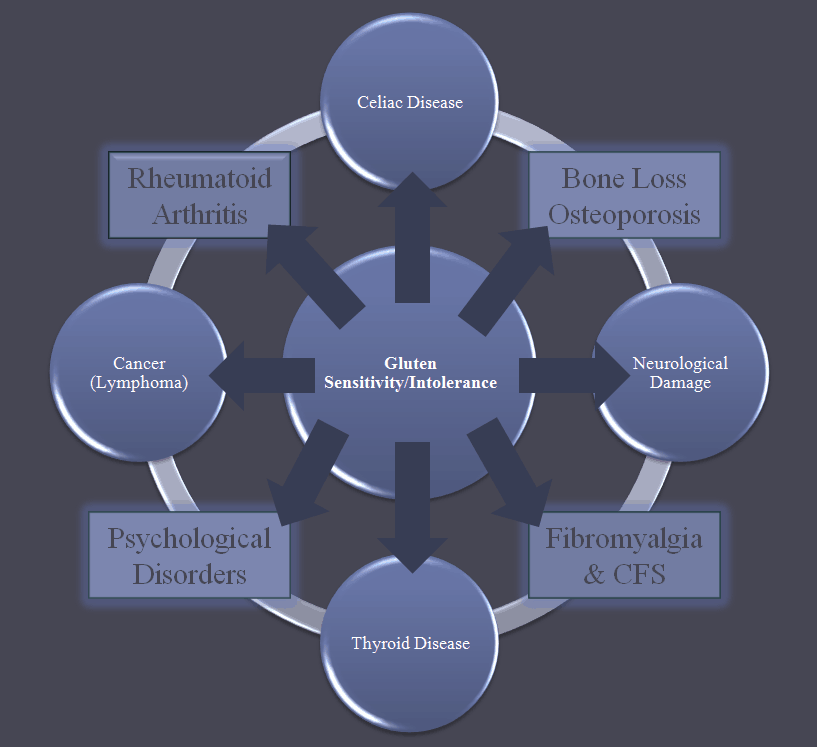
Gluten sensitivity is not a disease. Much like a peanut allergy is not a disease. Exposure to the gluten itself is the trigger necessary to create the negative outcome – i.e. some people who eat gluten experience severe migraine headache. If they don’t eat gluten, they don’t experience the pain of the migraine. In essence, the migraine is the body’s way of letting the person know that they should stop eating the gluten. The diagram below breaks down how you should look at gluten sensitivity from this perspective:
Gluten Can Cause Damage in Multiple Ways
One of the other points of confusion relating to gluten has to do with the fact that the pathway for gluten induced damage is not simple. There are a number of different ways that gluten can induce damage. Some of the pathways can be measured and identified via lab tests, others can not be measured at all.
One of the most common is through an allergic response. Classically, when people think of an allergy, they think of a acute reaction that leads to watery teary itchy eyes, shortness of breath, wheezing, coughing, hives on the skin, vomiting, or diarrhea. This type of allergy, also referred to as an IgE response occurs quickly – within three hours of ingestion or exposure. Think of this type of reaction as an immune system canon going off. Many experience a wheat allergy in this way. Keep in mind that a wheat allergy and a gluten sensitivity are not the same thing.
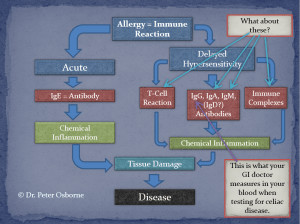
A delayed hypersensitivity reaction (see the right side of the diagram below) is a more subdued type of response. Don’t think cannon, think bullet. People don’t typically manifest severe or obvious problems with this type of reaction. This type of immune response builds with time and exposure. In other words the more a person is exposed to over time, the bigger the inflammatory problem becomes.
If you look at the diagram below, you can see all of the known immune pathways from both an acute and a delayed perspective. The IgE side of the diagram is typically what an allergy doctor will measure. When trying to identify celiac disease or gluten allergy, most labs only measure the IgG response to a handful of different types of gluten. This is precisely why so many tests come back negative even though a person may experience dramatic health improvements by cutting out gluten.
- Acute Allergy Antibody Response – IgE antibody formation and inflammation
- Delayed Allergy Antibody Response – IgG, IgA, IgM, and IgD antibody formation and subsequent inflammation
- Delayed Allergy Immune Complex Response – non antibody response that causes chronic inflammation
- Delayed T-Cell response – a direct response by the immune T-cells leading to chronic inflammation
Other Ways Gluten Can Cause Health Problems
There are a number of additional types of responses that rarely get discussed. Understanding some of them may be helpful for you to grasp the whole concept of gluten sensitivity better.
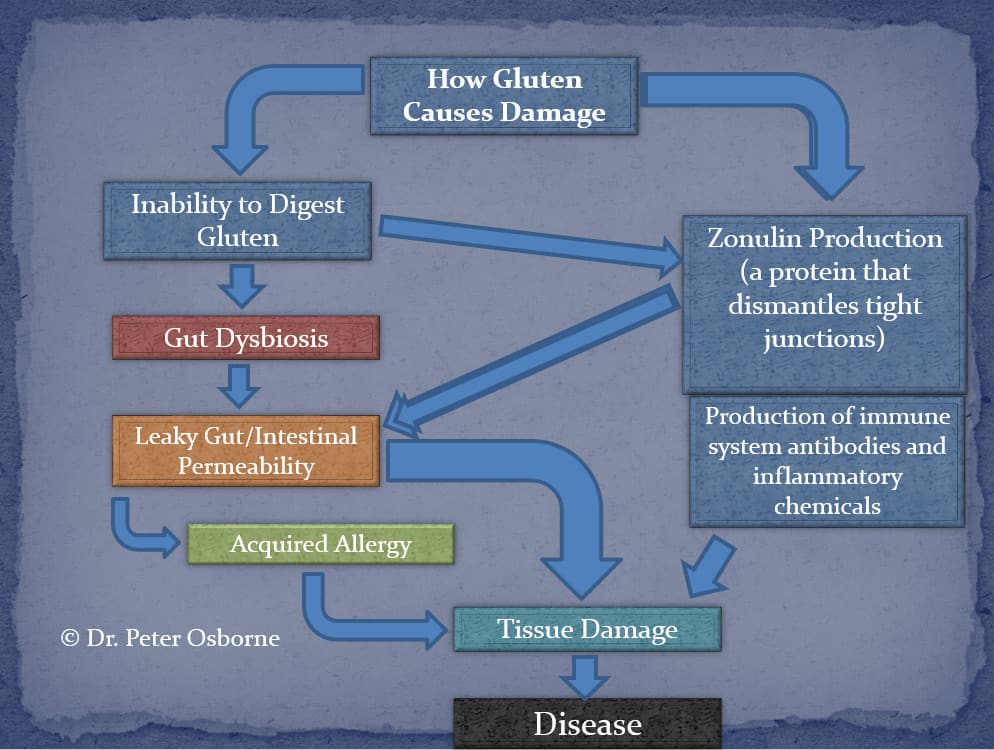
- Gluten Intolerance – not the same thing as a sensitivity, gluten intolerance refers to the inability to digest gluten. This in turn leads to the protein putrefying in the gut. The by product of putrefaction leads GI disruption in a number of ways to include the symptoms of IBS, stress on the enzyme producing cells of the intestine and pancreas, and changes in healthy GI bacteria.


- Gluten Induced Dysbiosis – gluten has been shown to alter the normal bacterial flora in the gut. This can lead to multiple types of digestive problems including leaky gut.
- Gluten Induced Leaky Gut – Dr. Alesio Fasano of Harvard discovered that gluten causes a direct intestinal permeability (leaky gut). This reaction is not an immune reaction. That is why the lab tests for celiac and gluten will never detect this. Remember that lab tests only measure antibody responses.
- Molecular Mimicry – This is what can happen after the gut becomes “Leaky”. The gut is responsible for handling all types of “undesirable characters” to include the viruses, bacteria, protozoans, prions, parasites, yeast, chemicals from food, chemicals in the water, etc. Some of the molecules that the gut helps to manage can mimic the tissues within our own bodies. When this happens, the molecular mimicry process leads to autoimmune diseases. For example, you may be exposed to a bacteria in your food. Your gut would typically handle this exposure without a problem, but because it is leaking, the bacterial proteins are able to access the blood stream. These bacterial proteins can mimic or look like the cartilage in your joints. If this happens, your immune system not only attacks the bacterial proteins, but it also starts to attack your cartilage. This in turn causes joint pain and inflammation.
- Gluten Induced Nutritional Loss – One of the biggest secondary effects of gluten is the loss of vitamins and minerals. This can occur as a result of GI damage and the subsequent inability to process, digest, and absorb nutrients, but it can also be as a result of excessive inflammation. Increased inflammation puts a greater demand on the body’s vitamin and mineral storage.
Guilt By Association – Damage not Caused by GLUTEN
Then we get to the non gluten aspects of grain that can also contribute to damage. These are the elements that are often confused as gluten sensitivity, and this is why some research shows that gluten proteins are not a problem.
- Lectins and other grain protective proteins – Remember what grains are – the seeds of grass…and like all seeds, they are designed to protect and allow for the perpetuation of their species. The seeds themselves are physically hard, hard to digest, but they also contain grain protective proteins that can cause inflammation and inhibit our ability to digest them. Examples of these non gluten proteins have been discovered over the last several years, but they are rarely discussed within the confines of gluten sensitivity. Some of these protein families include: Serpins, Purinins,and α-amylase/protease inhibitors.
- Chemicals Used in Food Processing – There are a number of chemicals used in food processing that can insight gluten like symptoms. One of the most common additives is MSG. Bromine is chemical commonly added to flour as a dough conditioner. It can enhance the detrimental effects of gluten. Another common enzyme process used for dairy manufacturing is microbial transglutaminase. This process creates a dairy product that can mimic gluten proteins. Carrageenan is another compound used to thicken foods. It has been shown to cause gluten like symptoms as well.
- Chemicals Used in Grain Production – The most notable is glyphosate – AKA Roundup. This chemical pesticide has been shown to cause many of the same symptoms as those seen in gluten sensitivity. Some believe that it is glyphosate, not gluten, that is responsible for many of the diseases we see gluten contribute to. I have personally not seen this with my patients. In my experience, those with gluten sensitivity who attempt to eat organic grain products continue to have reactions to the gluten.
- Grains are High in FODMAPS – these are difficult to digest carbohydrates that can contribute to gas, bloating, and irritable bowel symptoms. Wheat and corn sugars are especially high in them.
- Grains are High in Molds and Mycotoxins – Because of farming practices, grains contain large quantities of mold and the toxins mold produces. Some people have gluten like reactions to these compounds. Recent research has identified mycotoxin in corn to cause persistent problems in those trying to follow the gluten free diet.
- Medications & Other Foods Known to Mimic Gluten Sensitivity – Research from Mayo has identified that certain blood pressure medications can cause damage to the intestine that mimics celiac disease. Additionally, soy, dairy, and corn proteins have all been shown to cause villous atrophy identical to that found in celiac disease.
The Best Way to Determine Gluten Sensitivity
To date, no lab exists that is capable of measuring all of the different types of immune responses to all the different types of gluten proteins. Many will argue that an elimination diet is the best way to determine gluten sensitivity. I don’t fully agree with this premise. Yes, it is a smart thing to pay attention to the food you eat and how it makes you feel. If you feel bad eating a food, the common sense thing to do is to avoid it. However; many people suffer from silent, internal inflammation for years before properly diagnosed. It can take several decades of inflammatory damage before a person starts to have open symptoms of disease. An elimination diet does not identify these people.
Understanding that gluten sensitivity is not a disease, but rather a state of genetics, it makes better sense to default to genetic testing as the most accurate screening tool. To date we have discovered two gene patterns that are present in the majority of those who have celiac disease. These genes are referred to as the HLA-DQ genes (there is an alpha1 and a beta 1 gene). These genes are responsible for building a receptor on the surface of your immune cells. The job of this receptor is to help the immune system recognize good from bad. Having a gluten sensitive gene pattern directly increases the likelihood that your body will look at gluten as an enemy. The side effect of this response is inflammation. The more gluten exposure over time, the greater the inflammatory response.
As stated above, there are thousands of different types of gluten proteins that have the potential to interact with the HLA-DQ receptors on your immune cells. Knowing your gluten gene pattern is helpful in determining whether or not gluten consumption poses a risk of creating inflammation. Not knowing is guessing. Using genetics to identify Non Celiac Gluten Sensitivity risk should be the gold standard for all.






29 Responses
My husband has MS and in an attempt to minimize meds he needs to take we did some research and found that a gluten free diet might help him. So, together we decided to eat gluten free. He feels much better, less sluggish, more energy. I do too! While neither of us have Celiac or Gluten Sensitivity according to our doctors, we both feel great and would never go back to our gluten eating ways! Gluten is an inflamatory and it does just that…to us anyway.
Hi
Thanks for all the great information on gluten & celiac.
Since I eliminated gluten, over time
my vision has improved from 20-400 to 20-30. My auto immune Hashimoto’s is gone – no testable levels of antibodies, and my life long chronic bronchitis is gone.
Kathy
You are welcome Kathy!
Thanks for sharing your story with us! So glad you are feeling better!
All the best,
Dr. Osborne
After being diagnosed with Hasimoto’s hypothyroidism, I did a lot of online research. So many sites suggested a gluten free diet. My Thyroglobulin Ab was at 531 and my Thyroid Peroxidase was at 497. After two years of being GF my Thyroglobulin dropped to 170 and my Thyroid Peroxidase dropped to 134. My doctor said going GF had nothing to do with it! I believe it did! I also lost weight in places that I never could before!
me too and on Ipad right now
thanks so much for writing this! Im a pediatric nurse practitioner and nutrition/lifestyle nerd and very interested in topic
Thank you for this amazing information you provided in this extensive article. I’ve been a follower of yours for many months & never cease to be impressed with the information you freely share with us. After self diagnosing my long term gluten problem & having some major improvements, I then had a few minor set backs, I mentioned this to my primary care physician & asked about getting tested for my condition. She looked at me like I was from another planet. This article provides a wealth of detailed useful information. Thank you! Lisa
Lisa,
Thank you for tuning in! I am so glad that you have found the information helpful!
All the best,
Dr. O
P.S.
My comprehensive new book, No Grain No Pain is coming out in January. You can pre-order it on Amazon.
I would like to share your article with friends and family who don’t believe this whole gluten thing but I am not able to see the graphics that you have displayed and would like to know that that’s working before I forward this on .
Thanks so much for all your doing !!!
It exists, for sure. My symptoms of bloating, gas, indigestion (“too slow”) have improved a hundred per cent with a gluten free diet and my irritabilty too. I think we just need to listen to our bodies, to pay attention to our reactions to the food and we will clearly identify what does harm to us.
Thank you for the article, it’s really informative.
“How long will it take for the medical profession and people in general to realize that:
The human body cannot make something out of nothing.
The use of refined and de mineralized foods cause our body to disintegrate . First our teeth and then may follow gastric ulcers, arthritis, and heart disease.
ANY poison added to food or drink is too much- we are being submitted to illegal mass experimentation when this principle is violated.” Dr. Royal Lee founder of Standard Process Whole Food Concentrates ………..this was his statement in 1955 !!!!!
Thanks Dt.Osborne for all your hard work !!!!
Doing my little part emailing family in different parts of the world to help educate the hows & whys.
You are very welcome Stefi! Glad I could be of help to your and your family!
Best,
Dr O. –
This infirmation is revealing. But, what do we have left? Vegetables and meats? The ancients ate more grain than meats and vegetables. So what happened? Why are grains no longer edible? Where can i get more infornation?
Anyone who isn’t a believer just needs to stop gluten for one week then eat it again . It will make a believer out of them. I have proven that myself gluten not only bloats it contributes to diabetes worse than sugar.
I have been gluten free since January and am convinced through my own health that all that is here written is true for an increasing number of people. What I did want to share, however, is my practice of soaking rice, millet and buckwheat overnight in two teaspoons of whey (the liquid from yoghurt) which decreases the hard to digest phytates. I would be interested to know if other people also find that helpful and if there is a way of testing this method´s safety. Thanks!!!
I find it difficult to communicate with my Dr. in regard to anything that falls outside of what he has been taught, He dismisses anything that doesn’t show up in tests that have been proven to be inadequate; i.e., I don’t have Celiac Disease therefor I don’t have a problem with Gluten. Makes me wonder how much doctors in general are growing in knowledge. It is refreshing to see the movement toward Functional Medicine. I don’t believe in taking drugs, I want to know the root cause and frankly do not trust doctors who are too quick to prescribe drugs!
I had suffered from severe migraine-type headaches from most of my life, beginning in my 20’s. It was only in my mid 60’s that I have become almost free of my headaches, and one of the triggers has shown itself to be gluten in wheat. However, I should add that other of my triggers are foods known to be high in vegetable protein of other types, notably soy and quinoa, and also casein in milk. The bottom line is that some people have extreme sensitivities to certain foods, and just because the “gluten sensitivity debunkers” may not have such issues themselves, they should not generalize their good fortune to the population at large.
Three days after finding out I was gluten intolerant and giving up gluten, I stopped having daily headaches that had plagued me for over 30 years. Nobody can tell me that gluten free is a scam.
I had Hashimoto’s a year ago. My antibodies were 552. I went gluten free and in 6 months they came down to 3.
Dr. Osborne,
I cannot see the charts on my iPhone either. So for the Apple users, here’s what I know regarding HLA-DQB gluten genetics:
DQ1 subcategorized as DQ5 and DQ6
DQ2 is a risk for celiac, NCGS, ataxia, 02 01 is a risk for MS, type I diabetes and the second most common haplotype among Caucasian Americans
DQ3 (subtypes categorized as DQ7, DQ8 and DQ9) is a risk for celiac, NCGS, ataxia as DQ8;
DQ4 no known gluten risk ( only 2% have one, but what is on the other allele?) only 1% of Americans have two DQ4s
DQ5 is a risk for NCGS, ataxia
DQ6 is a risk for NCGS, ataxia, 06 02 is a risk for MS and is the most common haplotype among Caucasian Americans
DQ7 is a possible risk for celiac, risk for NCGS
DQ8 is a risk for celiac, NCGS, ataxia, type I diabetes
DQ9 is a possible risk for celiac, a risk for NCGS
How did I do doc?
I respectfully take issue with the sales pitch to a genetic test that you sell on your site. Why is this test suddenly the gold standard.? Are you saying that testing a person’s genetic coding is the only 100% foolproof way to know if they are gluten sensitve? I would need a lot more info about this test and its reliability and validity before I even considered whether this was worth it.
I believe an elimination diet has been called the gold standard, to avoiding gluten, not some test people know little to nothing about.
Maria,
You might consider watching some of the videos provided on this sight about genetic testing. An elimination diet can be tricky. While eliminating grain and feeling better may be considered or construed as gluten sensitivity, there are also many other possibilities – i.e. allergy, intolerance, sensitivity, reaction to mold not gluten, reaction to pesticides, reaction to other types of protein beyond gluten, FODMAP reaction, etc.
All the best,
Dr. O
A genetic test cannot tell you if you have a disease or will get it. It can tell you something about your risk, but not everything. The most important thing is to get the best antibody test available for celiac disease before going gluten-free. The reasons are: 1) according to Dr. Kenneth Fine, 47% of Americans have either a DQB2 or DQB8 gene. 2) very few celiac patients have been diagnosed. 3) most celiacs claim to have no symptoms (they are used to the way they’ve always been) 4) the autoimmune antibody tests for celiac are not valid unless you are consuming gluten. 5) one medical doctor I heard had the courage to call a gastroenterologist who orders a gluten challenge for someone who experienced celiac symptoms and already went gluten-free “bordering on malpractice”. This is because the patient’s immune system may have recovered to the point that all kinds of disabling autoimmune damage can occur during a gluten challenge.
You should be wary and ask a lot of questions about the particular lab’s genetic testing. I used the cheek swab gluten sensitivity genetic screening through enterolab.com, done by the American Red Cross. They identify both of your HLA-DQB genes on chromosome 6 and tell you something about your risks. If you can find a lab that will identify both of your DQA genes as well, that would be ideal. The alpha portion provides some risk, but the beta portion provides the major risk. Some labs only give you a positive or negative, without identifying anything. Some labs just identify the alpha portion first, and if it is not positive, they skip identifying the beta portion. Stay away from both of those situations. A risky alpha portion on one allele and a risky beta portion on the other allele is a risk for celiac disease.
Also, there is a gene on chromosome 16 that determines how much zonulin you secrete in response to a certain gluten peptide, which affects your risk for intestinal permeability. I doubt there is a commercially available test for that yet.
Scandinavian researchers have discovered 47 other genetic loci that affect gluten sensitivity and Indian researchers have discovered about 100.
Furthermore, if you have your DQA and DQB genes identified you can usually know what your risks for other autoimmune diseases are from nearby genes. For example, I know that I have two different genes on my two alleles that are risks for systemic lupus erythematosus. Dr. Pamala Smith MD says that SLE can cause your immune system to attack every organ, tissue and system in your body.
Thank-you for the great info. I know I have a problem with gluten and have tried unsuccessfully to get around it. I now completely understand the gluten issue and am planning to be completely gluten free in the future.
I am gluten free and feel loads better – less overall inflammation, and a lot less depression & migraines. I do travel a lot and try my best to avoid gluten, but it is hard. A friend of mine suggested that I carry activated charcoal tablets with me in the event I feel as though I may have been “glutened” that day. Would that help? I’ve tried various enzymes on the market, without much success.
Arlene,
Charcoal will not do much for gluten exposure. I would highly recommend you carry Gluten Shield with you when you travel. It is a digestive enzyme that contains a special protease designed to help with gluten breakdown. It also contains a type of probiotic that gluten has been shown to disrupt. You can read more about it here <<===
All the best,
Dr. Osborne
Thanks Dr. Osborn for your article answering the doubters and to the book”GLUTEN LIE”. I have been tremendously helped by living gluten free, started knowledge of it in 2006 and did not at first follow it very well, but got back on track in 2012 after much pain. Now much better bc I am stricter and have learned also other food sensitivities have also been a factor.Thanks again Dr. Osborn for all you do!
I’ve never been tested but was urged by a doctor to go gluten free for a few months to see if there were positive changes. This was around 7 years ago. I didn’t really realize the amazing impact until my husband had to be in the hospital and I had to eat the hospital food, none of which was gluten free. It was then that my migraine headaches came back along with intestinal issues, both of which had plagued me for life. . Now, it is quite obvious. A little gluten brings a headache quickly along with digestive problems later. I believe I have less joint aches and pains without gluten also though this is not so obvious. I’m convinced!