Contents
ToggleGluten Affects People in Many Ways
To date, scientists have elucidated a number of ways that gluten can cause damage to both celiacs and non celiac gluten sensitive individuals. Unfortunately, when trying to identify gluten as a progenitor to disease, doctors typically only look to diagnose celiac disease. As celiac disease is an autoimmune reaction in the small intestine identified by measuring specific antibodies (gliadin, anti-tissue transglutaminase, and anti-endomysial antibodies) and performing a biopsy of the intestine, those who don’t have positive test results fall through the cracks. Even though these people report feeling better on a gluten free diet, many doctors and nutritionists insist that their patients continue to eat gluten because their labs are celiac negative.
The Lab Tests Are Not Definitive
Here in lies a big part of the problem. When doctors use labs as definitive information, and ignore what a patient is telling them, then the patients fail to get better without knowing why.
A new research study has identified a new mechanism of gluten induced damage. Current lab tests do not address this newly discovered finding, but you should be inclined to share it with your doctor if you respond favorably to a gluten free diet even though your traditional lab tests have come back negative:
Ingestion of wheat, barley, or rye triggers small intestinal inflammation in patients with celiac disease. Specifically, the storage proteins of these cereals (gluten) elicit an adaptive Th1-mediated immune response in individuals carrying HLA-DQ2 or HLA-DQ8 as major genetic predisposition. This well-defined role of adaptive immunity contrasts with an ill-defined component of innate immunity in celiac disease. We identify the α-amylase/trypsin inhibitors (ATIs) CM3 and 0.19, pest resistance molecules in wheat, as strong activators of innate immune responses in monocytes, macrophages, and dendritic cells. ATIs engage the TLR4-MD2-CD14 complex and lead to up-regulation of maturation markers and elicit release of proinflammatory cytokines in cells from celiac and nonceliac patients and in celiac patients’ biopsies. Mice deficient in TLR4 or TLR4 signaling are protected from intestinal and systemic immune responses upon oral challenge with ATIs. These findings define cereal ATIs as novel contributors to celiac disease. Moreover, ATIs may fuel inflammation and immune reactions in other intestinal and nonintestinal immune disorders.
Source: J Exp Med. 2012 Dec 3. Wheat amylase trypsin inhibitors drive intestinal inflammation via activation of toll-like receptor 4.
How Gluten Causes Damage:
Gluten has been shown to damage people in different ways:
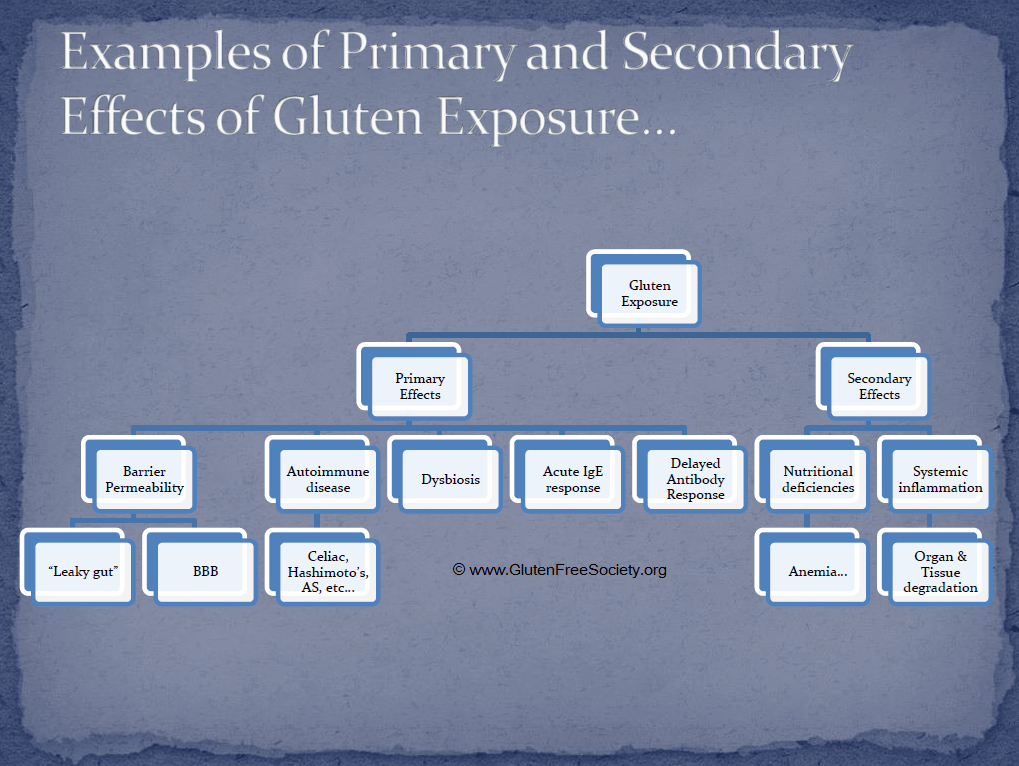
Some of the more commonly known mechanisms are listed below and many more are listed in the diagram…
- Adaptive immune reaction – People make antibodies to gluten that subsequently cause inflammation and tissue damage ultimately leading to autoimmune disease.
- Intestinal permeability – gluten disrupts the gut barrier causes a leaky gut (see diagram)
- Digestive distress – gluten digestion is resistant. This leads to changes in bacteria, gut dysbiosis, as well as increased risk for infections.
- Maldigestion and Malabsorption – This process can cause numerous problems including – vitamin and mineral deficiencies, anemia, weight loss, failure to heal, hormone imbalance, and many more.
Sometimes Gluten is Not the Issue – Components in Grain Are…
You can read more about Grainflammation in detail right here <<<
All the best,
Dr. O
 Ingestion of wheat, barley, or rye triggers small intestinal inflammation in patients with celiac disease. Specifically, the storage proteins of these cereals (gluten) elicit an adaptive Th1-mediated immune response in individuals carrying HLA-DQ2 or HLA-DQ8 as major genetic predisposition. This well-defined role of adaptive immunity contrasts with an ill-defined component of innate immunity in celiac disease. We identify the α-amylase/trypsin inhibitors
Ingestion of wheat, barley, or rye triggers small intestinal inflammation in patients with celiac disease. Specifically, the storage proteins of these cereals (gluten) elicit an adaptive Th1-mediated immune response in individuals carrying HLA-DQ2 or HLA-DQ8 as major genetic predisposition. This well-defined role of adaptive immunity contrasts with an ill-defined component of innate immunity in celiac disease. We identify the α-amylase/trypsin inhibitors 






15 Responses
is there a test for gluten sensitivity? if yes, can you tell me the name of it.
Larissa,
The most accurate way is through DNA. Check out the video and information here >>> https://stg-gfsociety-testing.kinsta.cloud/genetic-testing-for-gluten-sensitivity/
All the best,
Dr. O
This is no one like Dr. Peter Osborne that I am aware of doing this for us? He truly cares. He’s an Angel!
Could it be possible that gluten sensitively is really Celiac before one tests positive?
I have been gluten free, preservative free and almost completely dairy free for 7 months and it’s the first time in over 25 years that I can say I feel GREAT. My immune system has been so compromised by foods and each and every time I ended up either at the Dr.’s office or the ER they would tell me that there was nothing wrong. It wasn’t until I ended up in the hospital for three days with a B12 deficiency diagnosis that I started putting two and two together. You see I also had a higher than normal white cell count and would get hives in the cold. After many nights of research on the computer and speaking with my primary care doctor did he decide to send me to a hematologist to have extensive blood work done…also sent me back to the gastro dr. for more test…Tests should CLL and dybiosis…..my body has been in FIGHT mode for years due to FOODS…I blame gluten for ALL of it…..It amazes me that I can feel SO amazingly good now by eliminating foods from my diet. Just 2 weeks after going gluten, preservative and dairy free my WBC went down over 6 points…I’ve dropped 31 lbs. in 7 months too….FEELING GREAT!!!!
How come most people loose weight on GF diet and I don’t? My belly is even bigger?
Most gluten free foods are higher in calories than regular foods. Gluten free only lets you loose weight if your weight gain came from being sensitive to gluten.
Because something else is still causing inflamation.
@Dr. Osborne, I owe my life to you. You have provided the scientific information for me to continue my healing process.
I share some of your information on the cookbook-memoir I am about to publish, “Tales of A Gluten-Free Gypsy” I am 77 and have been on the g-f diet for more than 5 years. Continuous improvement for gluten-sensitivity and intolerance. I have more credibilty because of your documented research.
I wrote this book to warn people about the dangers of the gluten-free fad. My family have all converted to gluten-free.Thanks for all your inspiration. I refer all my clients to you.
Judith is the one who is responsible for turning me on this website! I will be forever grateful
Thank you Judith and thank you Dr Osborne.
I am trying to do my part and pass this information on to others not only my clients as a health coach but anyone who shows an intrest.
Hello Dr, Are you ever in DC, I was thinking of a Presentation at some point?
Hope all is well!
Q
Hi Q,
I get to DC on occasion. Do you have a group in need?
Thank you Dr O. I cant thank you enough. Rashes on my back and arms have disappeared after i went gluten free for only two months. My problem however is that where i come from our staple food is complex carbohydrate. As soon as i eat i just sleep off. Trying to cut off but difficult to know what to eat. Still strugling with my body fighting itself. Itchy sensation all over my body.
Valerie, I hope you found the answer to your question to Dr Osborne above. Look up The Thyroid Connection by Dr Amy Myers;)
Dr. O.
I WAS WONDERING WHAT TO DO AS MY SON HAS BEEN EFFECTED HIS ENTIRE LIFE WHEN HE STARTED EATING SOLID FOODS. HE HAS BEEN HOME BOUND FOR ALMOST ALL OF HIS CHILDHOOD, HE IS NOW 15. MANY YEARS IN AND OUT OF HOSPITALS, FAR TOO MANY GASTEROLOGISTS,BIOPIES,TESTS AND MORE TESTS,MANY , MANY SPECIALISTS ONLY TO BE DISAPPOINTED AS NOTHING HAS HELPED HIS DAILY, NIGHTLY INTENSE PAIN. I HAD HIM ON T.P.N FOR 3 1/2 MONTHS, HIS GUT RESTED, AND HE GOT WELL, COMPLETLY ,FOR 5 MONTHS, THREE YEARS AGO.BECAUSE OF HIS SEVERE WEIGHT LOSS AND THE AUTO IMMUNE, THEY DID THE T.P.N. DR’S SAID HE HAD SMALL BOWEL NEUROPATHY ALL OVER HIS SMALL INTESTINES AND MASTOCYTOSIS .
ALTHOUGH NONE OF THESE WERE PRESENT AFTER THE T.P.N, HE GAINED 34 POUNDS, FOR THE FIRST TIME IN HIS LIFE WAS NOT ON PAIN BUT THEN JUST 5 MONTHS LATER IT ALL STARTED AGAIN WHEN FOODS WERE INTRODUCED. I MAKE FERMENTED YOGURTS, CHICKEN BROTH WITH THE CHICKEN BONES, SOME CHICKEN. HE BREAKS OUT WITH COLE SORES WITH FRUIT,POSSIBLE FRUTCOSE ALLERGY,AND HE IS LACTOSE INTOLLERENT.
AT A TIME IN HIS LIFE WHEN HE SHOULD BE WITH OTHER CHILDREN IN SCHOOL, HE REMAINS HOME YEAR AFTER YEAR IN PAIN, ISSOLATED FROM FRIENDS,……..AND CAN’T PLAY OUTSIDE BECAUSE HE IS SO ATTOPIC, THE HEAT BOTHERS HIM TOO. AFTER YEARS OF IN AND OUT OF HOSPITALS, INFECTIONS HE IS NOW LEFT WITH THE LAST YEARS OF WHAT I THINK IS AUTO IMMUNE. EVERYTHING YOU SPEAK OF(AND I HAVE WATCHED SEVERAL OF YOUR LECTURES THAT ARE WONDERFUL)I ALWAYS THINK IS MY SON CONDITIONS.NO MEDICAL DR’S HAVE BEEN ABLE TO HELP AND I WAS WONDERING IF YOU KNOW OF ANY GOOD DR’S IN PHOENIX AREA. WE JUST MOVED FROM FLORIDA.IF NOT, I WOULD LIKE TO COME SEE YOU IF YOU THINK YOU COULD HELP.MY HEART BREAKS EVERY DAY AS MY SON FALLS FARTHER BEHIND IN SCHOOL, NOW TWO YEARS BEHIND AND HE IS O SMART BUT TOO WEAK TO THINK, WRITE OR DO THE WORK ANYMORE.I WOULD APPRECIATE YOUR HELP, I KNOW YOU ARE A CARING DR, YOU HAVE A COMPASSION TO HELP THOSE IN NEED, ESPECIALLY THOSE THAT SLIP THROUGH THE CRACKS,…LIKE MY ONLY SON.
THANK YOU FOR AL YOU DO.
VERY CONCERNED MOM,
SHERRY REDMOND
sredmond4jc@gmail.com