Contents
ToggleGrainflammation
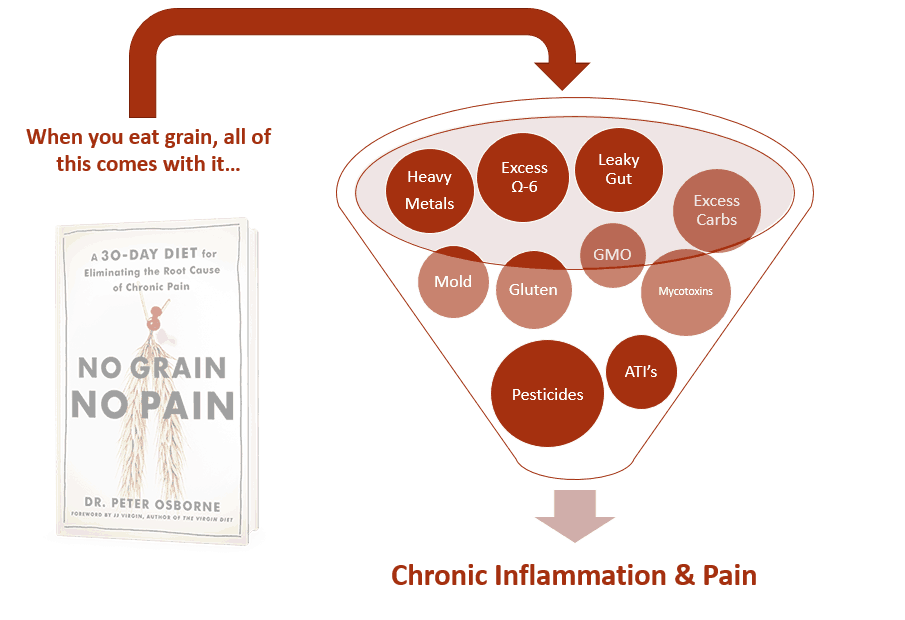
For many, gluten can cause a host of health issues including, leaky gut, chronic inflammation, changes in the healthy bacteria of the GI tract, and autoimmune disease. However; gluten is really only one of many problems with consuming a grain based diet. There are many other chemicals in grain that can contribute to poor health and disease.
Gluten IS a Problem
You see the articles and hear the news stories – Gluten Sensitivity Doesn’t Exist. Yet millions of people are gravitating toward the diet and feeling better. As a matter of fact, the gluten free diet is the biggest diet trend ever. It dwarfs Atkins, South Beach, Paleo, SCD, FODMAP, Sugar Free, Fat Free… But it doesn’t exist right?
I find it hard to believe that people would voluntarily restrict their diets for a trend if their was not a dramatic improvement in their health. I find it hard to believe that people would avoid classic favorites like pizza and hamburgers if doing so didn’t lead to improvements in diseases like migraine headache, IBS, depression, chronic fatigue, neuropathy…
Gluten is NOT the Only Problem & Celiac is Not the Only Gluten Related Disease
 Even though research overwhelming proves that gluten sensitivity exists, there are other non gluten components found in grains that can cause autoimmune problems. Additionally, there are other foods, chemicals, and medications that have been shown to cause similar types of inflammatory damage. These things are rarely discussed and are a proverbial “no man’s land” when it comes to getting a proper diagnosis. Because of this, the people who test negative for celiac disease as well as those who don’t have symptoms of classic celiac disease are left without a diagnosis. They are left without validity to why they are sick when they are exposed to grains or any of the other items on the list below. This, in my humble opinion is where the science needs to focus. To date we have had studies showing the following food based chemicals and drugs can trigger symptoms identical to gluten sensitivity and celiac disease
Even though research overwhelming proves that gluten sensitivity exists, there are other non gluten components found in grains that can cause autoimmune problems. Additionally, there are other foods, chemicals, and medications that have been shown to cause similar types of inflammatory damage. These things are rarely discussed and are a proverbial “no man’s land” when it comes to getting a proper diagnosis. Because of this, the people who test negative for celiac disease as well as those who don’t have symptoms of classic celiac disease are left without a diagnosis. They are left without validity to why they are sick when they are exposed to grains or any of the other items on the list below. This, in my humble opinion is where the science needs to focus. To date we have had studies showing the following food based chemicals and drugs can trigger symptoms identical to gluten sensitivity and celiac disease
- Corn
- Soy
- Dairy
- Quinoa
- GMO foods
- Intestinal infections (yeast, bacteria, parasites, etc)
- Mold and mycotoxins
- Non gluten proteins found in grain (see below)
- Medications – including antibiotics, blood pressure lowering drugs, and acid blockers
New Grain Research Confirms Gluten is Only Part of the Problem
 New research published in the Journal of Proteome Research (click the image on the right to see study) identifies 5 new groups of non-gluten proteins that are responsible for inflammation in patients with celiac disease. These 5 protein families are distinctly different from the gluten proteins traditionally known to cause celiac disease, and this research helps shed light on why so many people who test negative for gluten antibodies respond favorably to a gluten free diet.
New research published in the Journal of Proteome Research (click the image on the right to see study) identifies 5 new groups of non-gluten proteins that are responsible for inflammation in patients with celiac disease. These 5 protein families are distinctly different from the gluten proteins traditionally known to cause celiac disease, and this research helps shed light on why so many people who test negative for gluten antibodies respond favorably to a gluten free diet.
These 5 protein groups were all found in wheat and include:
- Serpins
- Purinins
- α-amylase/protease inhibitors
- Globulins
- Farinins
I wrote about #3 in 2012 after research identified these proteins as inflammatory. This new study reconfirms prior research, but also opens up a proverbial can of worms.
How Doctors Diagnose Celiac Disease is All Wrong
Lab tests currently used as the gold standard for diagnosing celiac disease and non celiac gluten sensitivity are vitally flawed. Unfortunately, these known flaws are rarely addressed. Doctors continue to use these tests, ignoring their faults, and patients continue to slip through the cracks. To date, there are no laboratories that commercially test for immune responses to these 5 types of proteins. You can read an excerpt from the study below:
“Compared with healthy controls, patients exhibited significantly higher levels of antibody reactivity to nongluten proteins. The main immunoreactive nongluten antibody target proteins were identified as serpins, purinins, α-amylase/protease inhibitors, globulins, and farinins. Assessment of reactivity toward purified recombinant proteins further confirmed the presence of antibody response to specific antigens. The results demonstrate that, in addition to the well-recognized immune reaction to gluten, celiac disease is associated with a robust humoral response directed at a specific subset of the nongluten proteins of wheat.
The outcome of this study begs the question – “Are there other non gluten, non wheat, grain proteins that cause similar types of inflammatory damage?” The answer is yes. To date, corn and rice have both been found to be problematic. Another study identified an additional 400 gluten proteins in varying grains that more more inflammatory than gliadin (the original type of gluten protein discovered in 1952).
Co-author of the research paper, Dr. Peter Green,of the Celiac Disease Center at Columbia University Medical Center had this to say:
“These results indicate that immunologic reactivity in celiac disease may not be limited to wheat gluten, but can involve certain non-gluten proteins, too. I think the findings have implications for understanding the mechanism of the disease and developing new therapeutics.”
Understanding that what we call celiac disease, what we call gluten sensitivity, goes far beyond the confines of a singular protein named gluten. The research above confirms this, and YOU should understand it as well. Why? Some studies show that as many as 92% of patients going gluten free fail to respond to the diet change. Many of the reasons why are listed above. You should study these and present them to your doctor if you are in that 92%.
Always looking out for you,
Dr. Osborne – The Gluten Free Warrior





24 Responses
Unfortunately, I believe my 16 year old daughter fallen into this category. For a lay person it is difficult to understand what that means as far as altering her diet and how to test further. Any suggestion would be highly welcomed.
I have had gluten sensitivities and hypothyrodism for 23 years that I know off as it was only then I got diagnosed but had been having problems for years before. My doctor 23 years ago was well ahead of his time luckily and really looked at these problems in a way other medical people didnt even know about. He slowly took me off wneat and then gluten, all dairy, red meat. The meat was added back in later. He lightened my immune load which with herbal supplements helped my body to heal itself from the autoimmune lroblems which RA and thyroid problems are among many others. We also didnt have gluten free food around then so I learnt to eat properly without replacing foods with just junk carbohydrates with more grains and starches that can cause more problems.All my thyroid issues normalized, all aches, pains and stiffness disappeared plus I lost 35 kilos which is 5 stone. Over the years I have gone off the wagon for periods of time and all my problems come flooding back. Dr Ozborne is so onto it and absolutely right. Follow his guidelines and you wont believe the changes you will experience. Sure it can be difficult with all the food around today but when you get the great results it will be so worth it. Goodluck.
I find this VERY interesting!!!! I suffered for years (at least 8). With these strange rashes & not 1 doctor suggested I try a gluten free diet. Then one day Dr Oz had a show on gluten and at the end of it the specialist who was on said there is on other reaction that can happen, but it is not at all common so I’ll skip it, but luckily Dr Oz said tell us what it is, you never know who’s out there listening and might be having that reaction. Thank god he did!! I was the one person (maybe not only) who’s life was changed by that detail. My husband looked at me & said that’s your problem!! That night we cleaned out our kitchen. Then the next day I went on line and researched gluten. It was then I learned it wasn’t only in food, but various drug store items too. I started reading labels and saw gluten was in my cosmetics and moisturizer. I began to change all of these products for gluten free ones. I also found out it was in gum. BINGO another item I ingested everyday. I got rid of all the gum I had and started buying only trident. Amazingly all my rashes cleared up!! I couldn’t believe it!! I got further proof that I was affected by gluten when if I did eat or use a product with gluten in it my rashes returned. I was SO thankful to have learned about gluten that afternoon, it changed my life!! I don’t have celiac so, but I definitely am affected by gluten. I have since thanked Dr Oz for helping to save my life. If it hadn’t been for that show about gluten I don’t even know how bad I would be by now!! Gluten DEFINITLY does cause other problems besides celiacs disease. I hope the medical profession will finally agree!!! Helping a lot more of us figure out what’s causing their strange reactions even when they get negative results for celiacs.
Robbin, What type of rashes did you get from gluten…location, severity, how long did rash last? I’m wondering if gluten is sparking my sister’s sudden rashes. Thanks for your help.
Please message me Joleen. I may be able to help. Go to my site and type in gut health in the search bar
I definitely have sensitivities, in varying degrees to items 1-5 and wouldn’t be surprised if the other items on the list are problematic,, but have not had to put them to the test, thankfully.
In recent months I have identified that any form or quantity of corn will lower my mood, quickly to depression and eaten daily for 3 days caused accute suicidal thoughts. I can now understand why synthetic T4 became less effective for me following 18 years of successful medication with T4 up to approx 2000.
It will be wonderful when main stream medicine catches up with all the research and knowledge shared by the wonderful Intagrative Doctors…..Currently I am my own pysician, I only turn to my general practitioner when there is a test i want that they offer.
Thank you for all you share, it is greatly appreciated
Sue, can you explain more about the T4? Does it have corn in it? I’ve had allergy testing many years ago and was allergic to corn. Also, if I accidently eat or drink anything with high fructose corn syrup, it makes me have a sore throat. More info will be appreciated.
Thanks!
JL
J L I have only seen your question! In the UK most Thyroxine (T4) has maize starch as one of the fillers/excipients.
The tiny amount of maize starch effected my mood and for many years I was not motivated, just couldn’t be bothered and this is not like me at all! My house became a mess, clutter, clutter everywhere! I transitioned across to Natural Dessicated Thyroid 2 years ago and that with a ‘clean’ diet (no gluten, dairy, corn, soy, egg white, very few carbs and only natural sugar) has transformed my life.
Sadly our main stream doctors are not open to excipients in pharmaceuticals causing problems to their patients…..
Good luck with your journey…We are our own health detective 🙂
Nancy, I, too have RA and hypothyroidism. I’ve been taking synthroid for the hypothyroidism and never questioning my doctor for 20 plus years and was just dx’d w/RA in 2010. 2 years ago I listened to a free webinar that directed my attention towards Hashimotos Thyroiditis and I asked my doctor to test me for the 2 thyroid antibodies. I tested high on one of the antibodies, the other was in the normal range.
He didn’t know what to do with that info other than just keep prescribing synthroid like he’s done for past 20 years. They synthroid has kept my thyroid tests in the normal range but it has never reduced any of my symptoms. I have every single textbook symptom attributable to hypothyroidism. So I’ve had to research on my own. I can’t afford to go to a naturopathic doctor or do any of the further testing because my insurance won’t cover it.
For the past 2 years, I’ve really made some major changes that have paid off. Every time I’ve gone for my thyroid lab tests, I have needed a reduction in my synthroid. Started at 200 mcg, reduced to 175, 150, 137, then 125 and now on 112 and just had labs drawn and am waiting to hear the results.
Some of the things I’ve done that have helped: Stopped drinking tap water filtered through my refrigerator because that filter didn’t remove fluoride or chlorine or chloramines. Those things all get into the iodine receptors we have on every cell in our body and block the iodine from getting in, which is necessary for the cell to use the thyroid hormone. Also, bromide found in flour and baked goods can also block iodine. I buy Reverse osmosis, filtered water from a local health food store. It’s a system set up by “Fresh Pure” which filters out fluoride, chlorine, chloramines, pharmaceuticals, radiologicals, and just about every other undesireable thing found in today’s municipal tap water. Of course it also removes all the beneficial minerals from the water too, but I can live with that and make sure I get my minerals from food and a multi-mineral supplement and good quality sea salt or pink himalayan salt.
I would benefit even more if I could afford to filter my home water that I bathe in. But I settle for filterd drinking and cooking water as better than nothing.
I also try to avoid all the xenoestrogens that are found in plastics, and harmful pesticides and chemicals used in meat and produce. I try to eat only organic produce and organic grass fed/finished meat and poultry.
I also avoid all wheat and barley products, using only coconut and almond flour to bake with. I have cut way back on dairy products like cheese and drink only coconut or almond milk. I avoid most processed foods altogether and just eat real whole food for the most part. I never eat soy if I can avoid it and also stopped eating corn. These are all foods that are often found to contribute to food sensitivities. I try to eat an anti-inflammatory diet because inflammation is the driver of almost all autoimmune disorders.
All the NSAIDS that I took for RA probably contributed to “leaky gut syndrome” which then drives the food sensitivities further and causes more autoimmune problems. Fortunately, all the dietary changes I’ve made have lowered my inflammation enough that I no longer take the medications for RA.
I’m a work in progress but feel like all these changes have been changes for the better and have benefitted my health tremendously. My goal is to get the Hashimotos under control so I can someday stop taking the synthroid too. But I’m not sure whether or not my thyroid will ever bounce back after being artificially controlled by the synthroid for 20 plus years. We’ll see, I just keep trying to eat right and get good exercise like walking and rebounding. Next I want to try weight bearing exercises. Did I mention I’ve also lost 50 pounds in the past two years? Prior to all those changes, I had been progressively gaining weight for the past 20 years.
I didn’t do all this overnight. It took time and persistence after falling off the gluten wagon several times. I took baby steps but I kept trying to make progress. Still am…
Hope some of this helps you.
Lori
Thank you so much for all your info, I am going to keep on plugging away. I have had RA for about 13 yrs that I know of. I have never been on any RA meds, I take .88 mgs of synthroid.
very informitive subject
Exactly what Kate said – this article contradicts itself. Maybe more clarity. If gluten free is working for most – maybe it is but some people are having lingering symptoms and fall into the 92 percent. I *knew* once I figured out I was gluten sensitive (on my own by eliminating it) that rice was going to be the next big problem. I read a Dr. Osborne article that corn can cause issues too so I also eliminated that – I eliminated soy, corn, and gluten and am vegan. I felt great and my skin was awesome – all my pain gone. I’m 34 but have been having unexplained bone pain for a couple of years now and lost 20 pounds without trying. I sometimes drop to 102-103 pounds when I’m really stressed out. For the most part have been at 108 which is a bit low for me not that I’m complaining. It’s when I get to 102 with stress that freaks me out. Anyway – I think if people would go vegan they would solve a lot of their problems. Not only is eating meat and dairy HORRIBLE for the environment (see Cowspiracy.com) but think about what the animals are eating – wheat – corn – soy. You’re getting it second hand. And dairy is just terrible for you – we are the only species that takes babies away from their mother so we can drink her milk. It’s ridiculous. I went back to eating soy and corn but am going to eliminate again because otherwise I have a chronic runny nose (yeah I know) and bloating and itchy eyes. I know I should cut out rice but that one has been difficult. I don’t really do nuts anyway as they don’t agree with me well. I am very very sensitive. After reading this though I am going to eliminate all of it plus rice. So what do I eat? Lots of plants. The hardest thing is my plant protein as a lot of it contains rice… I eat a lot of avocados, fruit, and veggies. Once you eliminate all the crap from your diet you also find you aren’t as hungry and don’t need as much – and you’ll end up at a lower weight without really trying. If you’re wondering how I get my b12 – well b12 comes from the dirt – animals these days are deficient because they are eating corn-wheat-soy and not grass…so I wouldn’t get it from meat anyway. I supplement. There are plant based supplements. Don’t argue that isn’t natural because factory farming isn’t natural either. Other animals in nature do not have other animals raise and slaughter other animals by the billions so they can pick it up at the grocery store. So go vegan – get rid of soy corn and gluten and rice – and go from there. try to do organic as much as you can. Salad dressings do apple cider vinegar and olive oil and lemon. OH and one thing not mentioned – SUGAR – sugar is super inflammatory – eliminate it as you can. It will help lower cholesterol too.
I am so glad going vegan has worked for you. However, please don’t assume it will work for everyone and make a comment followed with don’t argue. I used to be vegan and it actually made me sicker. Before you accuse me of not doing it right I assure I did. I finally had a doctor tell me that I can under no circumstances continue to eat this way…and she herself was a vegan. I struggled with that bit of news for a long time but once I started adding in good source meat (I agree with you about CAFO)and raw dairy (not milk yet) I began to feel so much better. Not every diet works for everyone. Please do not judge others who must eat differently than you do. You don’t know the why of it. Everyone must walk their own path. I hope the vegan lifestyle continues to work for you and you don’t wind up with health issues caused by it 20 years down the road. And btw, cholesterol in and of itself is not bad. You need it for a properly functioning brain. Studies show that elderly people with higher cholesterol have less dimensia and are sharper than those with lower. Might be something to research. Just as the dairy campaign has not been truthful about bone health, the cholesterol s are is much the same.
I understood that when he spoke about the 92% he was specifically referring to those with Celiac Disease, not the general public.
Kate I have used Interolab.com to have my tests done – it was a gamechanger for me. i did gluten gentic test ++ and it has helped to initially show the soy-corn-casein-egg links. Also as i requested tests other allergies and for malabsorbtion for the most common foods.
That was last year it has helped me find my way and go on a TRUE glute free diet – with many more cross allergen triggers that i have now eliminated from my diet. But i am not completely syptom free, I still struggle with unknown contaminations
People stress going on a vegan diet, but I tried it for seven years, and felt horrible, so I went back to eating chicken, turkey and fish. Perhaps it works for some people, but I suspect that there is something to the studies involving blood types and meat eaters. It is difficult enough trying to figure out what to eat on a daily basis when you eliminate gluten and grains from your diet, without taking away all of the meat.
for Angela,
think about the sugar in your frut as well if you still have problems, I gave up sugar some time ago but still got rashes, Fructose was the culprit, I have had to give up almost all fruit, just an occasional treat and though I do eat a lot of veggies I take a vit C supplement.
Cyrex Labs tests more foods and was a life changing revelation for me:
Rye, Barley, Spelt, Polish Wheat IgG + IgA Combined ( CPT CODE : 86256 )
Cow’s Milk IgG + IgA Combined ( CPT CODE : 86256-59 )
Alpha-Casein & Beta-Casein IgG + IgA Combined ( CPT CODE : 86256-59 )
Casomorphin IgG + IgA Combined ( CPT CODE : 86256-59 )
Milk Butyrophilin IgG + IgA Combined ( CPT CODE : 86256-59 )
Whey Protein IgG + IgA Combined ( CPT CODE : 86256-59 )
Chocolate (Milk) IgG + IgA Combined ( CPT CODE : 86256-59 )
Oats IgG + IgA Combined ( CPT CODE : 86256-59 )
Yeast IgG + IgA Combined ( CPT CODE : 86256-59 )
Coffee IgG + IgA Combined ( CPT CODE : 86256-59 )
Sesame IgG + IgA Combined ( CPT CODE : 86256-59 )
Buckwheat IgG + IgA Combined ( CPT CODE : 86256-59 )
Sorghum IgG + IgA Combined ( CPT CODE : 86256-59 )
Millet IgG + IgA Combined ( CPT CODE : 86256-59 )
Hemp IgG + IgA Combined ( CPT CODE : 86256-59 )
Amaranth IgG + IgA Combined ( CPT CODE : 86256-59 )
Quinoa IgG + IgA Combined ( CPT CODE : 86256-59 )
Tapioca IgG + IgA Combined ( CPT CODE : 86256-59 )
Teff IgG + IgA Combined ( CPT CODE : 86256-59 )
Soy IgG + IgA Combined ( CPT CODE : 86256-59 )
Egg IgG + IgA Combined ( CPT CODE : 86256-59 )
Corn IgG + IgA Combined ( CPT CODE : 86256-59 )
Rice IgG + IgA Combined ( CPT CODE : 86256-59 )
Potato IgG + IgA Combined ( CPT CODE : 86256-59 )
They have a newer test, Array 10 for more foods that I have not taken as yet, but may do in future. Unfortunately, insurance does not cover these tests in my case, but the cost is worth it.
I understood that when he spoke about the 92% he was specifically referring to those with Celiac Disease, not the general public.
Understand that the patients did experience subjective improvements when removing traditional gluten from the diet. However; 92% of them had persistent, measurable continuation of gastrointestinal inflammation. Persistent GI inflammation is the problem because if the gut fails to fully heal, long term consequences such as vitamin and mineral deficiency, intestinal permeability, and chronic immune activation are a very real threat.
Robbin, can you elaborate a bit on the rash you had? I have had a terrible rash for 11.5 months and it started,about 36 hours after eating bread – rye bread. I had been gluten free for 8 years and decided to try the bread. I thought nothing would happen but the next day, I developed a rash on my back. Since then, it has spread to my neck, arms, face even though I haven’t had any gluten ( or any other grains) since last February. I’ve narrowed my diet to exclude grains, dairy, eggs, sugar. I will nt eat anything from a package or bottle. Everything is gone cooked and no seasonings with things I don’t know. But, I’ve been to 10 doctors and no one can diagnose my strange rash. How long did your rash last?
So, if my gut was damaged from eating the bread last February, what can I do to heal? Is it possible that my gut is permemently damaged? I haven’t had any gluten or grain since last Febeuary! I ve had the rash now for almost a year and no doctor can give me a diagnosis. The rash is so bad that I haven’t been able to work since September 2016. It is horribly itchy, painful and burns. It looks like I’ve been burned but biopsies show atopic dermatitis. Along with the rash, I feel very ill, esp when it’s flaring.
Patty,
It is possible you are suffering with other food or chemical allergy reactions. Here is an example of someone who had a similar issue and how it was resolved – https://www.youtube.com/watch?v=fcfp6kU5F2Q
Best,
Dr. O
I developed a rash in February 2016 after consuming bread. I had been gluten free for 8 years and this was kind of a test to see if there was anything to my doctors recommendation of cutting gluten. Well it’s been almost a year and I’m here to say, there is definitely something to the positive anti gliadin anti
Body in my saliva. This rash grows by the day, itches, burns and doesn’t show any signs of going away, despite being gluten free since last February. Now, my doctors can’t understand what is causing the rash because it’s been so long since I consumed gluten.
If anyone has experienced a prolonged reaction to gluten, I’d love to hear from you because everyone is mystified and I can’t go back to work until someone is able to identify this nasty thing.