Contents
ToggleHypothyroidism
 Hypothyroidism is one of the most common medical conditions diagnosed in the U.S. Thyroid medications account for the 4th most commonly prescribed drug. It costs patients more than 4 billion annually to treat, while the disease effects an estimated 13 million plus people(Data source here).
Hypothyroidism is one of the most common medical conditions diagnosed in the U.S. Thyroid medications account for the 4th most commonly prescribed drug. It costs patients more than 4 billion annually to treat, while the disease effects an estimated 13 million plus people(Data source here).
The Thyroid Problem
Typical symptoms of low thyroid condition include: fatigue, weight gain, bloating, dry hair and skin, joint pain, elevated cholesterol, sleep disruption, infertility, depression, and cold hands and feet. Traditional diagnosis is made based on a set of lab tests typically ordered by a general doctor, internist, or endocrinologist. This work up includes:
- TSH (thyroid stimulating hormone)
- T4
- T3
One of the many problems with this approach is that it is not comprehensive. If your TSH comes back high or if your T4 and T3 come back low, the doctor tends to diagnose you with hypothyroid disease. Unfortunately, this approach often times leads to treatment with medications without further investigation. Keep in mind one fundamental point – Having a low thyroid diagnosis and taking medicine does not fix the problem. Ultimately, the goal of the doctor and patient is to identify the reason the thyroid levels are abnormal. And this, my friends, requires a fundamental knowledge of nutrition and biochemistry.
Lets take a deeper look at some of the common things that can contribute to low thyroid hormone production:
- Nutritional Deficiencies (vitamins, minerals, etc)
- Gluten induced autoimmune response
- Excessive exposure to the halide elements – chlorine, bromine, and fluoride
- Eating massive quantities of goitrogenic foods (i.e. soy, peanut, cassava)
Adequate Nutrition is Crucial for a Healthy Thyroid
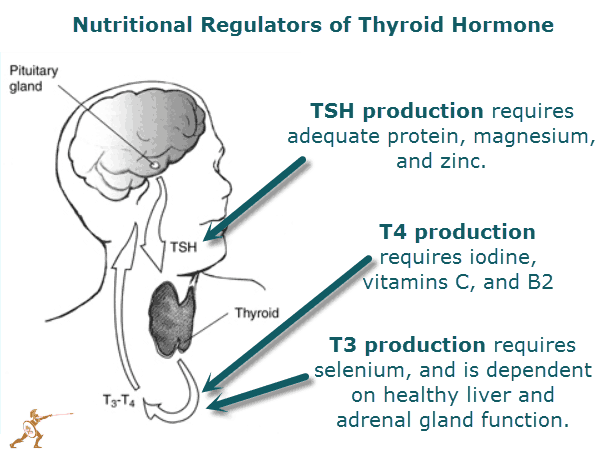
The diagram below illustrates some very important nutrient-thyroid relationships. Vitamins and minerals help drive the chemistry behind the production of the different thyroid hormones. They also help these hormones communicate with the DNA and other organs to improve and regulate metabolism. The following is a list of nutrients that your doctor should measure when evaluating your thyroid:
- Protein – most Americans eat too many carbohydrates and not enough protein. Protein is absolutely necessary to form the backbone of thyroid hormone (particularly the amino acid in protein called tyrosine). Protein is also responsible for carrying thyroid hormone through the blood stream to your tissues.
- Magnesium – this minerals help your body make TSH (the hormone made in your brain that tells your thyroid gland to make T4).
- Zinc – like magnesium, this mineral also helps your body make TSH
- Selenium – this mineral is responsible for converting T4 (inactive thyroid hormone) into T3 (active thyroid hormone).
- Iodine – this mineral helps the body build T4 (the hormone that doctors commonly measure that floats through the bloodstream). The “4” in T4 represents how many molecules of iodine are present.
- Manganese – is crucial for thyroid hormone production and also works as an antioxidant to protect the gland from free radical damage.
- Vitamin C – is extremely important for helping deliver iodine into T4
- Vitamin B2 – is extremely important for helping deliver iodine into T4
- Vitamin B3 – is extremely important for helping deliver iodine into T4
- Vitamin D – allows T3 to communicate to your DNA to regulate metabolism
- Vitamin A – works in conjunction with vitamin D to help T3 to communicate to your DNA to regulate metabolism
- Vitamin B12 – one of the most common B vitamin deficiencies, B12 deficiency can mimic low thyroid.
Gluten and Your Thyroid
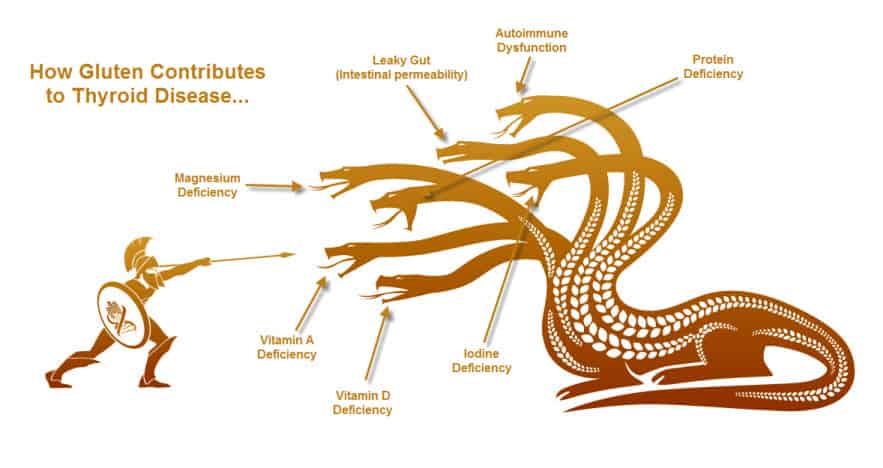
Gluten sensitivity contributes to hypothyroidism in a number of different ways. Gluten induced gastrointestinal damage is one of the main mechanisms of action. It is this mechanism that leads to a domino like effect. The first step in this process is the creating of intestinal hyper permeability (AKA – Leaky Gut). When the intestinal barrier is compromised, a cascade of inflammation, immune over stimulation, and molecular mimicry can ensue. Over time these processes can cause an autoimmune thyroid reaction often times referred to as Hashimoto’s disease.
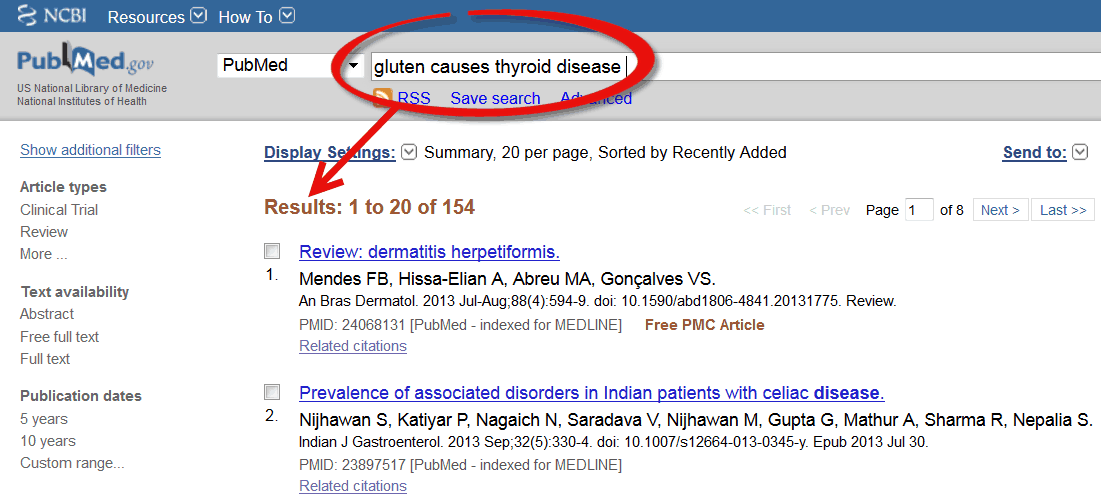
Gluten induced gastrointestinal damage can contribute to poor digestion and absorption of thyroid critical nutrients. Gluten can also alter normal gut bacteria. These bacteria play a crucial role in thyroid hormone conversion. Many doctors will argue that no research exists between gluten and thyroid disease. They are wrong. The image below is taken from a quick search in the National Library of Medicine database.
Multiple medical research studies show a connection between gluten and thyroid disease…
Thyroid Problems Linked to Halide Exposure
The halides chlorine, bromine, and fluoride all compete with iodine for uptake into your thyroid. Over exposure to these toxic elements is linked to an increased risk for hypothyroidism, but also to thyroid cancers. Avoidance of excessive exposure to halides is recommended to maximize thyroid function. Below are common sources of exposure.
Chlorine is typically found in: plastics, pesticides, paper products, unfiltered drinking water, bath water, swimming pools, processed salt products, and Splenda (sucralose). Water filters on your drinking water and bathing water are recommended.
Bromine/Bromide is typically found in: brominated flour products, citrus flavored soft drinks, chemical additive used in municipal water purification, pesticides, dyes, leaded fuel additive, brominated flame retardants: Carpet, upholstery, electronics, mattresses; bromocriptine (hyperprolactinemia), and OTC antitussives (cough medicines).
Fluorine/Flouride is typically found in: Toothpaste; fluoridated drinking water; infant formula; processed cereals; non-organic grape juices; wine; beer; soda; tea (higher in decaf); glass etching; Freon/refrigerants; cockroach insecticide fluoridated salt; non-stick coatings, Medications: Anesthetics: (Enflurane, Isoflurane & Sevoflurane); fluconazole; fluoroquinolone antibiotics, and linezolid antibiotics, Prozac/fluoxetine, efavirenz, fluorouracil, flurbiprofen, fenfluramine, cerivastatin, paxil, fluvoxamine, astemizole (allergy), cisapride, fluvastatin, fluocinonide & fluocinolone (topical corticosteroids); fluticasone & flunisolide; fluocinolone acetonide (intravitreal implant); fludarabine (antiviral); fludrocortisone; antimalarial drugs.
Foods That Contribute to Goiter (Thyroid Enlargement)
There are a number of foods that can impact thyroid hormone production. These are typically referred to as goitrogenic foods, because when eaten in large quantities, they can cause a goiter to form. The following is a list of foods that have these properties. Keep in mind that just because a food is goitrogenic doesn’t mean you cannot eat it. Cooking them reduces this effect by as much as 70-80%.
- Soy (cooking does not reduce the goitrogenic effects of soy)
- Brussels Sprouts
- Cabbage
- Cassava
- Broccoli
- Kale
- Spinach
- Flax
- Peanuts
The Labs You Should Have Your Doctor Analyze to Thoroughly Evaluate Your Gland
- TSH, T3 and T4, plus free T3 and T4
- Reverse T3
- Iodine loading test (urine test)
- Spectracell (vitamin and mineral deficiency blood test)
- Thyroid antibody testing – includes TPO and anti-thyroglobulin antibody testing
- Genetic testing for gluten sensitivity
- Food allergy testing
- Also consider measuring gut bacteria as well as ruling out chronic exposure to heavy metals (i.e. mercury and lead), and environmental molds.
Remember this – the article above is just a scratch on the surface of what you should know about your thyroid. Knowledge is power.
Always looking out for you,
Dr. Osborne – The Gluten Free Warrior
If you think that this information will help someone you love suffering with a thyroid problem, please forward this along.





5 Responses
A couple of years back, I had constant fatigue. I noticed I did better on the days I had a couple eggs. After a while, I got tired of eggs and decided to go with sunflower oil. I had more good days than bad days. Then one day I had a baby kale salad…the next day I couldn’t get out of bed. When I got checked out by my NP, my TSH was almost zero. I learned my lesson, not to eat kale or cabbage, and a more moderate use of sunflower oil. Yes, I feel better.
Hello. magnificent job. I did not expect this.
This is a great story. Thanks!
Attempting to filter your bathwater to remove chlorine is pointless in most metropolitan areas. All large cities have switched over from chlorine injection to chloramine injection (first chlorine, then ammonia a couple of miles downstream). Chloramines can’t be boiled off or removed by simple filters, it takes a HUGE activated charcoal filter stack and slow pass rate (lots of dwell time in the charcoal). It’s a lot like a dialysis filter, and it’s expensive to do, typically running $400USD per year for the filters or LOTS MORE.
Check out Wikipedia > chloramine and you’ll see the problems.
Thank you so much for sharing. I learned a lot from you!
All I read is what is on this site. I am already eating gluten free, dairy free, sugar free, no grapefruit (allergic to it), bananas (they make me constipated). If I were to follow your extensive list there would be nothing for me to eat.