Contents
ToggleYour Thyroid Gland
Before discussing the link between gluten and autoimmune thyroid disease, let’s first cover some fundamentals about the thyroid gland.
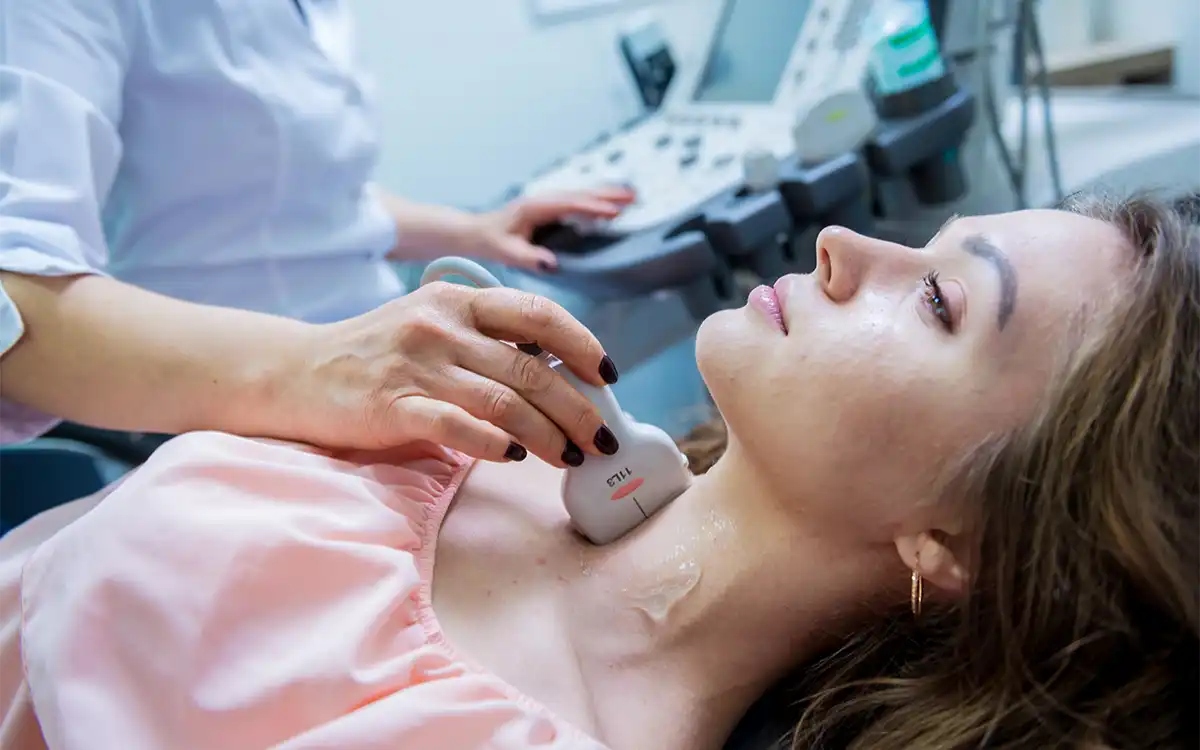
The thyroid gland is a butterfly-shaped organ located in the front of the neck, just below the Adam’s apple. It consists of two lobes, one on each side of the windpipe, connected by a bridge called the isthmus. The hormones produced by the thyroid gland play a crucial role in regulating various metabolic processes in the body.
Functions of the Thyroid Gland
The primary function of the thyroid gland is to synthesize and release thyroid hormones—triiodothyronine (T3) and thyroxine (T4). These hormones contain iodine and are essential for regulating several body functions.
Metabolic Regulation: Thyroid hormones influence the rate at which cells convert nutrients into energy. They help regulate metabolism, affecting processes such as energy expenditure, cell maintenance, and tissue repair.
Metabolism of Nutrients: Thyroid hormones affect the metabolism of carbohydrates, fats, and proteins. They help regulate the breakdown, utilization, and storage of these nutrients, contributing to overall energy balance.
Development and Growth: Thyroid hormones are vital for normal growth and development, particularly in infants and children. They play essential roles in brain development, bone growth, and maturation of various tissues and organs.
Regulation of Body Temperature: Thyroid hormones help regulate body temperature by influencing heat production and heat dissipation. Imbalances in thyroid hormone can contribute to cold intolerance or excessive sweating.
Heart Function: Thyroid hormones have significant effects on the cardiovascular system. They influence heart rate, cardiac output, and blood pressure, helping to maintain proper cardiovascular function. Imbalances in thyroid hormone levels can lead to heart rhythm abnormalities and other cardiac issues.
Now that we have a clearer understanding of the thyroid gland and its function, let’s dive into the autoimmune thyroid diseases.
What Is Autoimmune Thyroid Disease?
There are two main types of autoimmune thyroid disease – Hashimoto’s thyroiditis, and Grave’s disease.
Hashimoto’s Thyroiditis
Hashimoto’s disease is characterized by chronic inflammation of the thyroid gland caused by an autoimmune reaction. This condition results in the thyroid gland failing to produce enough thyroid hormones (hypothyroidism). Some of the most common symptoms of low thyroid function are fatigue, weight gain, joint pain, dry skin, hair loss, sensitivity to cold, and depression. Treatment typically involves hormone replacement therapy to restore thyroid hormone levels and manage symptoms.
Grave’s Disease
Graves’ disease is characterized by the overproduction of thyroid hormones. In this condition, the body produces autoimmune antibodies that stimulate the thyroid to produce excessive amounts of thyroid hormones. This overstimulation leads to hyperthyroidism. Grave’s often results in symptoms such as rapid heartbeat, weight loss, tremors, anxiety, and heat intolerance. Graves’ disease can also cause eye problems, such as bulging eyes and vision changes, known as Graves’ ophthalmopathy. Treatment options may include medications to regulate thyroid function, radioactive iodine therapy, or in some cases, surgery to remove part or all of the thyroid gland.
The Role of Gluten in Autoimmune Thyroid Diseases (AITD)?
Multiple research studies demonstrate that a gluten free diet can improve thyroid function, reduce autoimmune antibody production, and reduce symptoms those with both Hashimoto’s thyroiditis and Grave’s disease. A breakdown of these research finding are listed below.
Celiac, Gluten Sensitivity & Hashimoto’s
One study in the American Journal of Gastroenterology looked specifically at the prevalence of thyroid impairment among adult patients with newly diagnosed celiac disease. It found that there is a greater frequency of thyroid disease among celiac disease patients, enough to justify a thyroid functional assessment for newly diagnosed celiac disease patients.
Another study evaluated the genetic component to celiac disease and thyroid autoimmunity. It found that first-degree relatives of patients with celiac disease have a three-fold higher risk of developing autoimmune thyroid disorders and associated thyroid dysfunction. This means that if you have celiac disease, it may be worthwhile for your parents, children and siblings to be screened for both celiac disease and thyroid autoimmune disease.
Due to the increased awareness around Non Celiac Gluten Sensitivity (NCGS), some studies have attempted to identify whether there is an increased prevalence of thyroid dysfunction among individuals with NCGS as well. A review of literature published in the American Journal of Gastroenterology found promising evidence that a link may exist – particularly in those with Hashimoto’s thyroiditis developing NCGS.
Another study compared individuals with celiac disease and non-celiac wheat sensitivity and found that similar proportions of individuals with non-celiac wheat sensitivity and celiac disease (29% in both cases) developed an autoimmune disease (predominantly Hashimoto’s thyroiditis).
Gluten Free Diets Lead to Improvements in Hashimoto’s
A major meta analysis published in the journal, Frontiers in Endocrinology, found that gluten free diets not only improved antibody levels, but also improved TSH and T4 values in patients with Hashimoto’s.
One study looked at the effect of a gluten free diet on a group of women diagnosed with Hashimoto’s thyroiditis. The study split the group of women into those who followed a gluten free diet and those who ate gluten. The participants who followed a gluten free diet had reduced thyroid antibody levels.
Another study evaluated children aged 1-12 with celiac disease and concluded that compliance with a gluten free diet can help reduce incidence of autoimmune thyroiditis and also maintain a healthy thyroid in existing celiac disease patients.
Another topic of interest with respect to thyroid dysfunction is the symptom of obesity in those (particularly women) with Hashimoto’s thyroiditis. One study attempted to take the evaluation of a gluten free diet on autoimmune hypothyroid a step further and compared weight loss in a group of women with Hashimoto’s thyroiditis who followed a standard calorie reduction diet with a group of women with Hashimoto’s thyroiditis who followed a standard calorie reduction diet and a gluten free diet. After six months, body fat content was statistically significantly lower in the group of women on the gluten free diet than in the control group of only a calorie reducing diet.
Gluten Free Diet and Grave’s Disease
A major analysis published in The Journal of Clinical Endocrinology & Metabolism found that patients with gluten induced celiac disease were at higher risk for developing Grave’s disease.
A number of studies have acknowledged that a gluten free diet likely benefits those with Grave’s hyperthyroid as well, and that there is enough evidence to warrant further research. One case review is particularly compelling. It followed a 37-year-old woman with Graves’ disease as well as thyrotoxicosis (excess circulating thyroid hormones in the bloodstream) that was not responsive to medical management. She tested positive for celiac disease, and after initiation of a gluten free diet, her thyrotoxicosis responded to medical management and thyroid health stabilized.
What Can You Do If You Have Been Diagnosed with Autoimmune Thyroid Disease?
Bottom line…celiac disease and non celiac gluten sensitivity are linked to both Hashimoto’s and Grave’s disease. Research shows that a gluten free diet can bring many of these patients improvements. If you have been diagnosed with an autoimmune thyroid disease, and have not considered a gluten free diet, it is definitely worth investigating. Ask your doctor to test you for gluten sensitivity to confirm whether a gluten free diet is right for your thyroid.





27 Responses
Many thanks, Dr. O!
No idea why I needed to wait 8 or 9 months for this important article to be posted.
I did cut out all grains within the last 9 months after becoming more and more intolerant of many foods. Now, after following this program with very few relapses, I have seen my eyebrows grow back in, all normal colored, not white, and my snow white hair is now quite silvery, going to salt and pepper, because I have so much hair growing back in, all in a dark color–so much so that it shows up in photos. I am now slowly regaining some tolerance for some of the foods I could not eat one year ago, like eggs, and small amounts of yogurt. I also do not react violently to accidental ingestion of tiny amounts of grain like I once did, but I do not eat grain if I can help it!
My eyebrows are in a terrible state and would like them to grow back
Been both Hyper and Hypothyroid for over 30 years. Health has been in a terrible state.
I can eat many foods without any digestive problems, but interested in how going Gluten free can help with overall health and wellbeing.
Is gluten in oats? Is cous cous gluten free?
Yes there are gluten in oats. And cous cous is allmost made of grain.
I a Hashimoto and dont eat also spinazie SOY and bananas.
For me only glutenfree dieet doesnt worked.
Although gluten does seem to be a problem for many people, i think many people’s real problem lies elsewhere. The modern western (especially US) diet includes almost no foods which reinforce good probiotic bacteria levels within our gut (yogurt does, but many people don’t eat the right kind, or enough of it). All our milk products have been pasteurized, wiping out almost all the nutrients & probiotics that were once contained within it. Combine that with the fact that many people eat far too much sugar / processed foods, & many people end up living with a condition called ‘leaky gut’ (also caused by increased usage of antibiotics). Our intestinal linings literally become leaky, and small particles enter the blood stream, which the immune system has to get rid off. This leads to a general level of inflammation & poor health (feeling tired, difficulty losing weight, etc), and ultimately sets off autoimmune diseases, allergies, and serious health problems down the road. Try taking a probiotic (a good kind with a high active culture and strain count), & cutting out too much sugar & processed food. This alone will probably ‘cure’ many people’s ailments, and you might even still be able to indulge in a gluten filled snack once in a while. Good luck!
very interest in gluten thyroid connection
I have been having severe stomach cramps with the pain being simultaneously in my back. This has lead to a weight loss of 40 lbs. I don’t want the weight back, but I haven’t done anything to lose it. I have undergone several tests including an ultrasound of my gall bladder area, a CT scan of this area, also. My gallbladder was removed about 30 years ago; 2 endoscopies, one of them being an ultrasound endoscopy, and a colonoscopy, plus numerous blood tests. All tests came back negative, but malnutrition was found. I am taking Levothyroxine, Sertraline, Omeprazole, Colestipol all 1 x daily. I also take Endocet 10/325 up to 4 x daily or as needed, Soma, 2 x daily,both for back pain & muscle spasms & Requip, 3 x daily for RLS.
I have absolutely no energy, and could. easily sleep all day. Lately, what brings the pain on, is if I move around which causes my back to hurt thus triggering my stomach pain. What does relieve the pain is drinking something warm to hot and laying down with a heating pad, placed either on my stomach or back. It generally takes about 15 minutes to an hour for the pain to subside.
Could this possibly be connected to gluten intolerance with Hypothyroidism Are there any particular tests that you will suggest? I am at my wits end and am willing to do just about anything to rid myself of this problem! One more thing for you to consider in this history……………I had 2 lower back surgeries in 2011, with the 2nd one resulting in a fusion.
Any help or suggestions you can give me, will be greatly appreciated.
Sincerely,
Diane Malone
gizziesmom@wmca.net
Diane – I was getting the same: bad stomach ache & simultaneous backache every time I ate anything, for a number of years. (I do have hypothyroidism, so can’t lose weight.) The described pain happens only once in a while, NOW: I did give up gluten & dairy, & coffee & most sugar. I eat mostly fruits, vegetables, quinoa, & salmon. The best to you.
I am in the same pescatorian diet (plus coffee though). And I’m living it! =D
Amazing results in the body, mind and surprisingly emotional improvement as well! Never going back! 😛
Diane,
Cut out the omeprazole. If you are taking it just for acid reflux, you may find that you are actually low in stomach acid and you will be suffering from malabsorption issues.
Get you vit B12, vit D, vit A, iron, folate and ferritin tested, make sure you get the results from your GP along with the range.
You then need to take supplements to bring you up to the top end of the range on all.
Do a bit of research to provide you with the knowledge you need to supplement optimally
I myself have many of the same symptoms that you described. After suffering for 8 years with it I was just diagnosed with an inflamed pancreas. That might be the pain you feel. I feel it in my center about 6 inches above my bellybutton and in my back near my kidneys especially in the AM. I was told that I had dysbiosis in my gut and had become insulin resistant so I would have to stay on my grain free/sugar free diet forever. I guess it’s better than getting fat and feeling terrible. Expensive way to eat. He said my stool motility was poor and my stool was rotting in my gut leading to a leaky gut. He pointed out fungus and bad bacteria overgrowth as a problem for me. I did a three day stool test that I’m now awaiting the results for. Have your pancreas checked. I find that naturopaths and the like are better than traditional doctors. The 3rd leading cause of death is medical malpractice.
Thank you for posting this article. It’s always interesting to me to see how CD is connected to so many other AD. I would however, love to hear thoughts on the relationship between Graves Disease and CD. I see so many articles stating the correlation between CD and Hypothroid, but not the other end of the spectrum. Can you point me to any research studies pertaining to this? Thank you!
I have learned to take care of myself through a healthy diet. I rarely have to see doctors and i can list the kind of conditions I have treated myself with just keeping an eye of what I put in my body, for example, Sindrome of irritable colon. I make it clear, I have great respect for doctors but the food industry is killing more people than doctors are able to cure.
Since being diagnosed with CD I have been gluten free for about 8 months & sugar free for about 6 months. My GP has just reduced my thyroxine tablets from 1.25 to 1.00mgs.thrilled about that. However iBS has just flared up horribly and had such excruciating pain two days ago that had me doubled over had to escort to Mebeverine. Just drinking a glass of hot water with ginger is soothing me more. In spite of cutting nightshade veg, bean & lentils from my diet I have not lost weight. ( about 40 lbs overweight). Had life saving mitral valve repair about 10 years ago & take candestartin & aspirin to keep blood flowing & support my heart. Also CFS back with avenge cue after two year remission. Now my GP wants me to take a station as cholesterol too high. Any advice/ support gratefully received.
When IBS symptoms strike I find Fennel Tea helps ease the cramps and bloating. Fennel tea is sometimes hard to find, so I order online from Heather’s tummy care. Great site for IBS issues.
Don’t take statin. Google it there is so much info on how bad statins are for you and have zero effect on cholesterol
Need to get tests.
hi,i have hypothroid I haven’t been treated but have gained so much weight I know I’m gluten sensitive I have stomach problems if I eat gluten foods what should I do
Nellie,
I would encourage you to find a functional medicine doctor to work with. Sometimes having solid guidance can make all the difference.
All the best,
Dr. Osborne
Hi, I am 37 year old female. My Dad was recently diagnosed with Hashimoto’s (as a result of my persistence for him to get tested). I’m very sure I have it but I have never been tested (I asked my pcp to test me but she drew the wrong antibodies). I went strictly gluten and dairy free 2 years ago with the exception of white rice (I don’t eat much and not every day). I was also just diagnosed with osteoporosis, per a dxa scan, which my pcp ordered with resistance. I won’t be back to see her. Not wasting anymore time there. I did find a local integrative physical who is treating a friend of mine for Hashi’s. I have made so many changes and had had great improvements in my symptoms but I need help. I hope this new doctor, who I will see in OCT will be the answer I’ve been looking for. I just want to encourage others to keep looking for a practitioner who will listen and who will really help you, not just throw pills at you. You don’t have to accept mediocre treatment and you don’t have to figure it all out on your own. The functional approach is gaining momentum thanks to the tireless efforts of those like Dr. Osborne. I also just finished my nursing degree and hope to be part of the coming changes in healthcare. It is very exciting. Much love to all those out there who are struggling. You are not crazy! You are not alone! There is a better way!
I’ve been hypothyroid for many years, at least 20. Never thought about any connection to anything in particular. I’ve been in the medical field for 30 years, and just did and took what my doctors told me to. About a year ago, I became allergic to many chemicals and for the first time in my life developed eczema. All the dermatologists and allergists want to do is for you to out cream on it. (Most of which I am allergic to) the past year has been pretty miserable for me, as I gave not been free of outbreaks. I’m really interested in learning more about the thyroid. I feel I should be tested for gluten sensitivity, but not sure who would do this for me. I’m reading everything I can find on healing my body from the inside instead of masking the real problems. Any advice would be appreciated. Thank you.
Sandy,
Two things:
1. Genetic testing for gluten sensitivity can be done here.
2. Read and follow the 30 day protocol in this book <<<
All the best,
Dr. O
Sir, I had very athletic body and good health. But I had some digestive problems from childhood. Since last month, my cheeks get swallowing. Marginal increase in my weight, hair loss. Muscle tightening, losing consciousness etc. My doctor said it as hypothyroidism. I made some changes in my diet as increase use of wheat and rice. Is there’s any sense of sudden imbalance in thyroid hormones. Now my digestion is very weak. Can I get rid of this? Please help me sir
Please can you find some articles on the relationship between Graves Disease and CD. I have an over-active thyroid and have been advised to give up gluten, but you don’t seem to have anything on your website about this.
Could you comment about patient who doesn’t have thyroid anymore as she had thyroid cancer?
I just started a gluten free diet today, 6-18-21. I look forward !