Gluten and Cancer – What is the Connection
 Does gluten cause cancer? Do those with gluten sensitivity and celiac disease have an increased risk for developing this deadly disease? We will get to that shortly. First let’s dive into some statistics and facts around this deadly disease. Cancer is the second leading cause of death in the United States, with more than 1.5 million new cases diagnosed per year. About 40% of American adults are expected to develop cancer at some point in their life. And the World Health Organization predicts cases worldwide to rise by 70% over the next 30 years. All that being said, it is estimated that 1/2 of all cancers are caused by lifestyle choices such as diet and exercise.
Does gluten cause cancer? Do those with gluten sensitivity and celiac disease have an increased risk for developing this deadly disease? We will get to that shortly. First let’s dive into some statistics and facts around this deadly disease. Cancer is the second leading cause of death in the United States, with more than 1.5 million new cases diagnosed per year. About 40% of American adults are expected to develop cancer at some point in their life. And the World Health Organization predicts cases worldwide to rise by 70% over the next 30 years. All that being said, it is estimated that 1/2 of all cancers are caused by lifestyle choices such as diet and exercise.
Prefer to learn by video? Watch the breakdown here.
What is cancer?
Cancer is sometimes mistakenly seen as a foreign invader attacking your body. But that’s not what happens. Instead, cancer is when your own cells begin to grow abnormally. They grow faster than normal cells. They don’t function properly. They spread easily. And your body is unable to stop them.
So what causes your cells to grow abnormally?
Ultimately, genetic mutations and changes in gene expression (turning genes on or off) come into play. However, only 10% of cancer cases involve inherited gene mutations. The remaining 90% of cancers involve genetic mutations and changes in gene expression that occur after birth.
This is an important concept to grasp. Because it means that most cancers are preventable. Even if you’re genetically predisposed.
Risk Factors of Cancer
There isn’t one single cause or risk factor when it comes to cancer. It’s usually a combination of factors. And the contributing factors may be different from one person to the next.
Lifestyle-Related Risk Factors
It’s estimated that 33 – 50% of all cancers can be prevented by making healthier lifestyle choices. This means a vast majority of cancer risk factors are within your control.
Four well-studied lifestyle risk factors include:
- Poor diet
- Tobacco use
- Alcohol abuse
- Physical inactivity
Obesity, which can be triggered by the above risk factors in addition to others, also plays a role in the onset of cancer. The International Agency for Research on Cancer (IARC) estimates that obesity causes 25% of kidney cancers, 11% of colon cancers, 39% of uterine cancers, and 9% of breast cancers in postmenopausal women.

Infectious Disease
Chronic infections account for up to 20% of cancers. In fact, science has found at least seven viruses that can contribute to the development of cancer. And Helicobacter pylori is a species of bacteria that can cause stomach cancer.
Hormonal Risk Factors
Estrogen is a sex hormone involved in the development and progression of several cancers, including breast, ovarian, and uterine. Some cases are believed to be caused by an excess of estrogen coming from the food you eat, environmental toxins, birth control pills, and/or hormone replacement therapy.
In fact, the International Agency for Research on Cancer (IARC) has deemed hormone replacement therapy “carcinogenic to humans” based on scientific evidence that it may increase your risk for breast and uterine cancer.
Toxic Environmental Exposures
Air pollution, pesticides, food-borne contaminants, and chemicals added to processed foods, personal care products, and cosmetics all have links to cancer.
Other Chronic Diseases
Just like cancer, other chronic diseases are caused by a combination of risk factors. But it’s important to note that having a chronic disease also increases your risk of developing cancer as well as succumbing to it.
In addition to obesity, associated diseases include (but not limited to):
- Heart disease
- Kidney disease
- Diabetes
- Lung disease
- Autoimmune diseases (e.g., celiac disease, rheumatoid arthritis, and systemic lupus)
Autoimmunity occurs when your body’s immune system attacks its own tissues and organs. The resulting immune response causes inflammation. And chronic inflammation is believed to be the key link between autoimmunity and cancer (as well as most other chronic diseases).
The Connection Between Gluten and Cancer
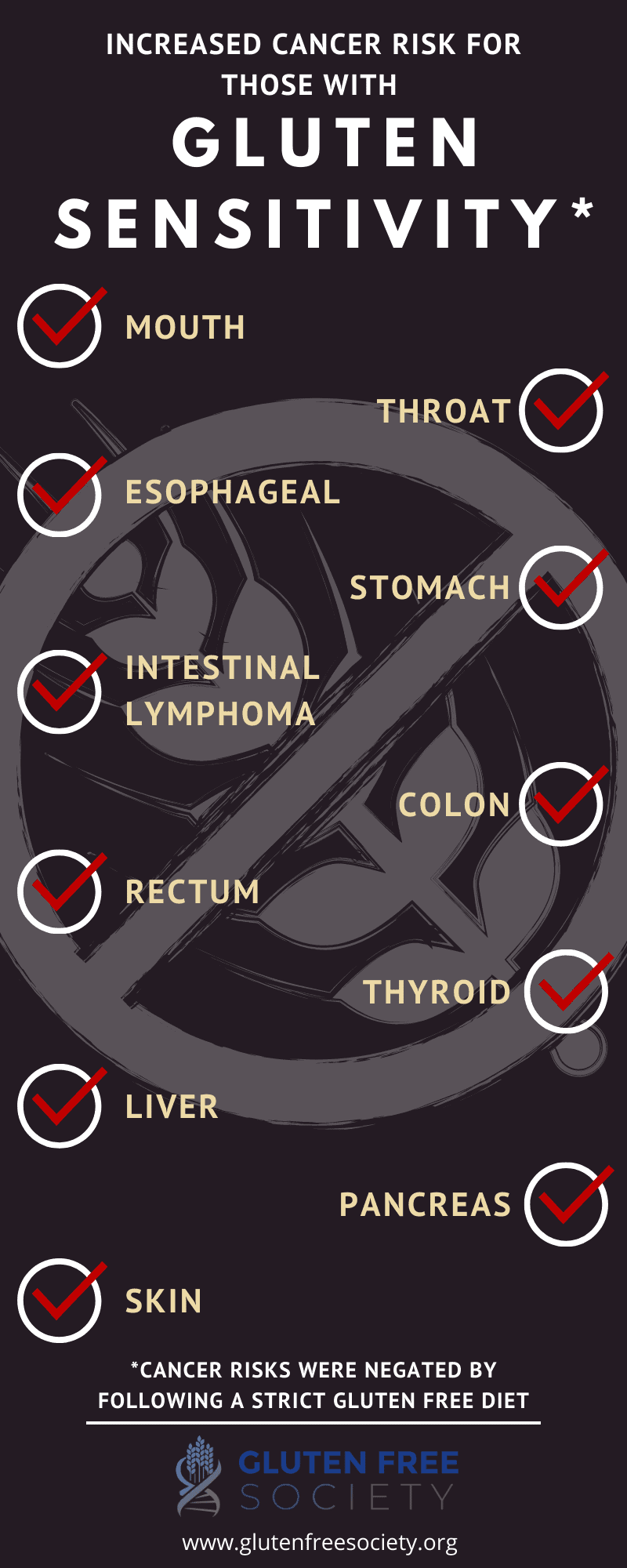
Research has shown an increased risk of developing cancer for those with gluten sensitivity who fail to follow a strict gluten free diet. For cancers of the mouth, esophagus and pharynx, there was a 22.7% increased relative risk. For lymphoma, there was a 77.8% increased relative risk.
Other research studies have shown that those with celiac disease who fail to comply to gluten free dietary restrictions have an increased risk for cancers of the intestine, colon, rectum, esophagus, thyroid, pancreas, skin, liver, and stomach.
Aside from the studies that show a direct increase in cancer development, eating gluten (and grains) can also contribute to almost all of the cancer risk factors I outlined above. So let’s take a closer look at all the possible connections…
Gluten Causes Inflammation
There’s no doubt about it. Gluten causes chronic inflammation in the gut as well as throughout the body for those with celiac disease and gluten sensitivity. Essentially, it irritates the lining of the intestines and causes the immune system to overreact.
Science has known about the link between inflammation and cancer since the 19th century. But researchers are now beginning to better understand the connection.
Inflammation is an immune response used to fight infections. Essentially, immune cells, such as macrophages and leukocytes, are sent to attack and neutralize threats. This is beneficial when you’re dealing with an acute situation.
However, this reaction becomes dangerous when chronic. Because the immune response produces inflammatory compounds and free radicals that damage cells and cause genetic mutations.
When this happens, your cells begin to divide to create new cells. One cell splits into two, two split into four, and so on. This process is known as cell proliferation.
However, due to the damage, a process known as metaplasia occurs where cells change from one type to another. For example, with some types of breast cancer, breast cells are transformed into cells that resemble soft and connective tissue.
Dysplasia is the term used to describe the presence of abnormal cells. And when these abnormal cells begin to multiply, that’s when tumors begin to form. Plus, tumor cells release inflammatory compounds, which contribute to their growth and spread.
Celiac disease, an autoimmune condition triggered by gluten, has been associated with an increased risk of certain cancers since the 1960s. It’s also correlated with a higher cancer mortality rate. There’s even some evidence that a strict gluten-free diet can help prevent abnormal cell growth and tumor formation.
A study has found that the older a person is at the time of their celiac disease diagnosis, the greater their risk for developing cancer. Thus, ignoring your symptoms or letting your condition go untreated is not recommended.
I also want to point out that gluten-rich foods are often heavily processed and made with chemical food additives and omega-6 fatty acids that are pro-inflammatory. Plus, researchers have found a 10% increase in ultra-processed foods in the diet is correlated with a greater than 10% increased risk of developing cancer.
Gluten Increases Risk of Infections
If your immune system is frequently activated when you eat gluten, it may become less responsive to other threats. So chronic gluten exposure may increase your risk of developing an H. pylori infection, a species of bacteria believed to trigger autoimmunity.
Using the pathway discussed above, H. pylori causes chronic inflammation in your stomach. If untreated, this inflammatory state causes cellular damage and the replacement of normal glandular stomach cells with intestinal cells (metaplasia). Dysplasia then occurs followed by tumor growth.
Gluten Causes Nutrient Deficiencies
Due to the intestinal damage gluten can cause in susceptible individuals, digestion and nutrient absorption are hindered. This leads to nutrient deficiencies, including those linked to both cancer and gluten sensitivity.
The mechanisms that link nutrient deficits and the progression of cancer are complex. Science has found that deficiencies in zinc, iron, vitamin B12, vitamin B6, and folate can damage your DNA, which can ultimately lead to cancer.
However, other links exist. Let’s take a look…
Zinc
Zinc is a mineral with hundreds of roles, including DNA synthesis, cell reproduction, growth, and tissue repair. Zinc deficiencies are associated with immune system dysfunction, including autoimmunity. Plus, zinc is anti-inflammatory in nature and works as a potent antioxidant to protect cells and DNA from free radical damage.
In this study, researchers found that 65% of patients with neck and head cancer were deficient in zinc. They also found that insufficient zinc levels reduced the activity of natural killer cells, which are capable of killing cancer cells. Overall, the scientists concluded that zinc supplementation may help slow the growth of cancer cells, reduce the release of inflammatory compounds, and increase cancer cell death.
Another study reported similar results when they found that zinc supplementation stopped the growth of tumor cells of the esophagus in vitro.
Iron
Iron deficiency is associated with cancers in the stomach and the esophagus. In the stomach, there may be a link between low iron and bacterial infections, such as H. pylori.
Scientists have found that iron deficiency can cause inflammation in the stomach that results in the loss of glandular cells responsible for secreting stomach acid. This can be dangerous because stomach acid is used to digest protein as well as kill harmful bacteria that enter the stomach. Thus, low levels of stomach acid can increase your risk of bacterial infections. The researchers also suggested that bacteria in the stomach may increase the production of nitrosamines from nitrates in the diet, which are carcinogenic to humans.
The same researchers also concluded that this might help explain the increased risk of stomach cancer in those with pernicious anemia, a lack of red blood cells caused by a vitamin B12 deficiency. Because a healthy lining of the stomach that secretes an adequate supply of stomach acid, as well as a compound known as intrinsic factor, is necessary to absorb vitamin B12.
Vitamin B6
Vitamin B6 plays a role in the metabolism of proteins, fats, and carbohydrates. It’s also involved in DNA synthesis as well as DNA methylation, a process that changes the activity of a portion DNA without changing its sequence. And these functions may be why vitamin B6 deficiencies are associated with an increased risk of cancer.
In fact, human studies have shown that higher vitamin B6 levels are associated with a 30 – 50% reduction in the risk of developing colon cancer.
In animal models, it’s been shown that vitamin B6 supplementation prevents tumor growth, reduces the number of tumors, and reduces oxidative stress. Plus, low vitamin B6 is associated with chronic inflammation.
Vitamin D
Many studies have shown that those with cancer generally have lower circulating levels of vitamin D than healthy control subjects. And high vitamin D levels have been associated with a lower risk of certain types of cancer, including liver, breast, esophageal, and stomach.
Further, treatment with extremely high doses (50,000 IU) of vitamin D every two weeks in women with cervical cancer helped reduce their tumor sizes as well as inflammation and oxidative stress.
Another small study found that 10,000 IU per day of vitamin D given to women with breast cancer significantly decreased concentrations of a compound (27HC) that supports the development of the disease.
Selenium
Researchers have discovered that selenium, a common gluten-induced deficiency, has the capacity to prevent genetic mutations and the growth of tumors in rodents when exposed to known carcinogens. However, the exact mechanisms involved are not fully understood.
There’s some evidence that selenium increases the secretion of detoxifying enzymes. It’s also known that selenium is incorporated into proteins that play a role in cell growth and death. These selenoproteins also have strong antioxidant properties. Thus, scientists suggest that selenium could play a role in cancers induced by a high intake of omega-6 polyunsaturated fats, such as those found in “vegetable” oils (i.e., canola, corn, soy, sunflower, and safflower). Because these fats oxidize easily. And selenium can protect cells from oxidative damage.
Before I move on, it’s worth noting that those eating a gluten-rich diet don’t usually get enough of the above nutrients to begin with. Because a gluten-rich diet is often filled with heavily processed foods that don’t contain adequate amounts of these nutrients.
Gluten Influences Your Hormones
In this article, I discuss many ways in which gluten can contribute to hormonal imbalances and dysfunction. And this is relevant because hormones help regulate cell differentiation (determining the type of cell), cell proliferation, and cell death. This means hormone abnormalities can help fuel certain types of cancer, such as breast and ovarian cancers.
The Connection Between Grains and Cancer
Grains are the source of gluten, but gluten isn’t the only danger associated with grains when it comes to cancer. This means even those without celiac disease or gluten sensitivity may be affected.
Pesticides
Grains are often grown with pesticides. And some pesticides are classified as carcinogens, which means they have the potential to cause cancer. Others have been shown to promote the growth of tumors in the presence of carcinogens. Plus, there are contaminants found in pesticides that may pose a risk.
Commonly used pesticides have been correlated with soft tissue sarcomas, malignant lymphoma, non-Hodgkin’s lymphoma, leukemia, and ovarian cancer.
Wheat specifically is often sprayed with a chemical known as glyphosate (AKA Roundup) to help increase the yield and speed up its drying time. Corn is also heavily sprayed with glyphosate.
Glyphosate is an endocrine disruptor. This means it can mimic your natural hormones and cause imbalances and dysfunction, which is one way it can contribute to cancer.
In March of 2015, the IARC classified glyphosate as “probably carcinogenic to humans” based on “limited” human evidence and “sufficient” evidence from animal studies. The IARC also reported there’s “strong” evidence indicating that glyphosate is capable of damaging DNA and causing genetic mutations.
Now, it’s important to note that limited and infrequent exposures aren’t likely to cause lasting harm. Problems typically arise over time from frequent exposures, such as eating pesticide-laden foods on a daily basis.
Grains are Contaminated with Mycotoxins
For most people in the world, grains are the largest component of their diet. And we’re constantly being told to eat more whole grains. However, not many people talk about the fact that grains, especially whole grains, are contaminated with mycotoxins.
Mycotoxins are metabolic byproducts produced by fungi (mold) that grow on grains. Fungi can infect grains growing in the field as well as during harvest, transport, processing, and storage. Thus, there are many chances for contamination.
Five common categories of mycotoxins found in grains include:
- Deoxynivalenol (a.k.a. vomitoxin)
- Zearalenone
- Ochratoxin A
- Fumonisin B1
- Aflatoxin
Deoxynivalenol is the least harmful, but it is prevalent. Zearalenone is classified as a possible human carcinogen. And ochratoxin A1 is linked to kidney disease, which is associated with cancer as I mentioned previously.
Fumonisin B1 is mostly found on corn and is a suspected carcinogen. Aflatoxins are the most dangerous and are classified as a “Group 1” carcinogens by IARC, which means the classification is based on a substantial amount of human evidence.
However, some people are more susceptible to the effects of mycotoxins than others, which is likely due to genetic factors.
The health of your gut may also play a role because certain species of gut bacteria can help rid your body of mycotoxins.
While large doses can cause acute toxicity and even death, it’s usually low doses over a long period of time that lead to cancer. Early symptoms may include:
- Headaches (including migraines)
- Wheezing
- Fatigue
- Muscle Pain
- Anxiety
- Mood swings
- Brain fog
There are several mechanisms by which mycotoxins can contribute to the development of cancer, including turning off tumor suppressor genes and causing DNA mutations. Some mycotoxins may act like estrogen while others may impair your body’s immune response.
It’s worth noting that mycotoxins can also damage the lining of your gut, which can cause inflammation, malabsorption, and gut bacteria imbalances.
Grains & Toxic Metal Contamination
Heavy metals are naturally found in soil. And plants, including grains, can absorb them from the soil as they grow. So when contaminated grains are consumed regularly over time, these heavy metals can build up in the body and cause harm that can contribute to the development of cancer.
For example, heavy metals can prevent beneficial minerals (e.g., magnesium, calcium, iron) from being absorbed, which can lead to nutrient deficiencies. Heavy metals can also bind to cellular structures and enzymes, which can change how they function.
The long-term effects of heavy metal poisoning can involve many systems and tissues, including your immune system, hormonal system, cardiovascular system, and metabolic systems as well as your bones, brain, liver, kidneys, and lungs.
Finally, most heavy metals are classified as carcinogens due to their ability to cause oxidative stress as well as damage and change the function of DNA.
Some heavy metals of concern found in grains include cadmium, arsenic, and lead.
Cadmium is found primarily in the endosperm, the inner starch portion, of wheat berries and rice. Thus, white flour, white rice, and all the products made with them are potential sources of cadmium contamination.
Rice absorbs more arsenic than any other grain. And it stays in the outer layer. So brown rice may contain up to 80% more arsenic than white rice.
Lead is found in equal amounts in the inner and outer layers of grains. In addition to absorbing lead from the soil, grains can also be contaminated with lead from old equipment during processing.
The amount of heavy metals present in grains depends on the specific soil they were grown in, the practices used to grow them, and how they are processed. So it’s hard to know what you’re going to get, which is one of the many reasons why I suggest avoiding grains all together.
Grains are High in Calories and Carbs
When you eat a diet filled with grains, it’s usually high in calories and carbohydrates. For many people, this leads to weight gain. It also causes insulin to rise over time, which further promotes fat storage and prevents fat burning.
So if you continue to consume more energy than your body needs, especially from grain-based carbohydrates, obesity and type 2 diabetes are possible outcomes.
Obesity is an inflammatory condition. It causes inflammation in your fat tissue, which can alter your body’s immune response. In addition, when your fat cells are inflamed, they release additional inflammatory compounds that can wreak havoc throughout your body. Thus, experts believe inflammation is a key link between obesity and cancer.
But obesity isn’t only associated with an increased risk of cancer. Data also shows that obesity can increase your cancer fatality rate. In a study of over 1 million American men and women, researchers found the following:
- Individuals with a BMI of 30 – 34.9 had a 9% increase in cancer mortality risk
- Individuals with a BMI of 35 – 39.9 had a 20% increase in cancer mortality risk
- Individuals with a BMI over 40 had a 52% increase in cancer mortality risk
Fat cells are also capable of secreting hormones, including estrogen and testosterone. Thus, the presence of more fat cells can increase the production of these hormones and/or create imbalances, which are associated with an increased risk of reproductive cancers.
Interestingly, scientists suggest the release of sex hormones by fat tissue may be driven by high insulin levels (a.k.a. hyperinsulinemia).
Hyperinsulinemia is also associated with rapid cell growth that can lead to cancer. In fact, many studies have found that hyperinsulinemia is correlated with an increased risk of cancer as well as cancer mortality. Further, in animal studies, calorie restriction diets that lower insulin levels have been shown to reduce tumor growth.

Can Gluten & Grains Cause Cancer?
There’s no denying the fact that gluten can cause significantly more harm than an upset stomach. The truth is a daily diet rich in gluten, grains, and processed foods can lead to cancer. Inflammation, nutrient deficiencies, environmental toxins, hormonal imbalances, and calorie excesses are key driving forces.
The big take away from most of this research, is that if you adhere to a gluten free diet, your risk of developing cancer is not increased.
So if you haven’t already, go change your, diet and make healthier lifestyle choices. It might just save your life.
Also, if you suspect that you have a problem with gluten, please don’t ignore it. Find a doctor that specializes in gluten-related conditions and knows what to look for.





4 Responses
I eat glutty free 🍞 bread & are corn base grown in Roundup glyphosate. I rat sourdough bread if I can get it.
hmm…no you don’t “get it.” Read his book. Watch his seminars and weekly Q&A. This is so serious and no sourdough will help. All grains to be zero grains or will continue to be ill and manifest other illnesses. Addictions to gluten even rice continues the madness. But they see it as a sacrifice and it most certainly sets you “apart” of which God says is a good thing.
Wonderful article! Very thorough and well written. I wish this information was more widely known. As an RN, I agree with this 100%. I will do what I can to spread the truth. Most health practitioners believe cancer just happens. Every disease has a cause. Thank you for this awesome explanation.
Just watched a Netflix special about Gluten, as a food staple in Gansu,China. I then searched “leading cause of death in Gansu” …. Stomach cancer