new to the gluten free journey?
new to the gluten free journey?

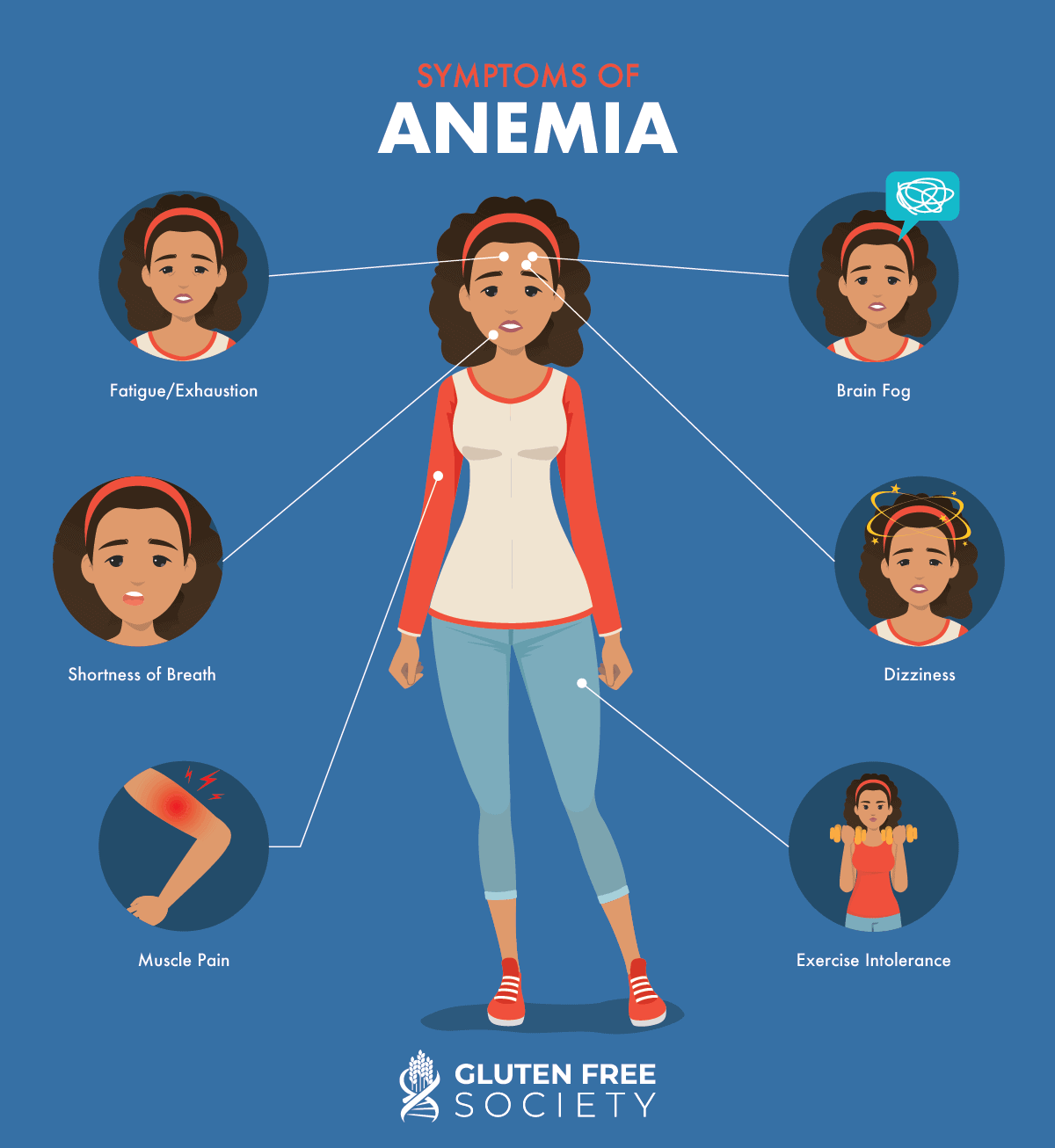 It’s important to note that these symptoms are similar to those of an underactive thyroid (hypothyroidism). Patients are often misdiagnosed or led down the wrong path of testing and treatment if both conditions are not explored. If you’re experiencing these symptoms, advocate for yourself by asking questions about testing for both conditions.
It’s important to note that these symptoms are similar to those of an underactive thyroid (hypothyroidism). Patients are often misdiagnosed or led down the wrong path of testing and treatment if both conditions are not explored. If you’re experiencing these symptoms, advocate for yourself by asking questions about testing for both conditions.
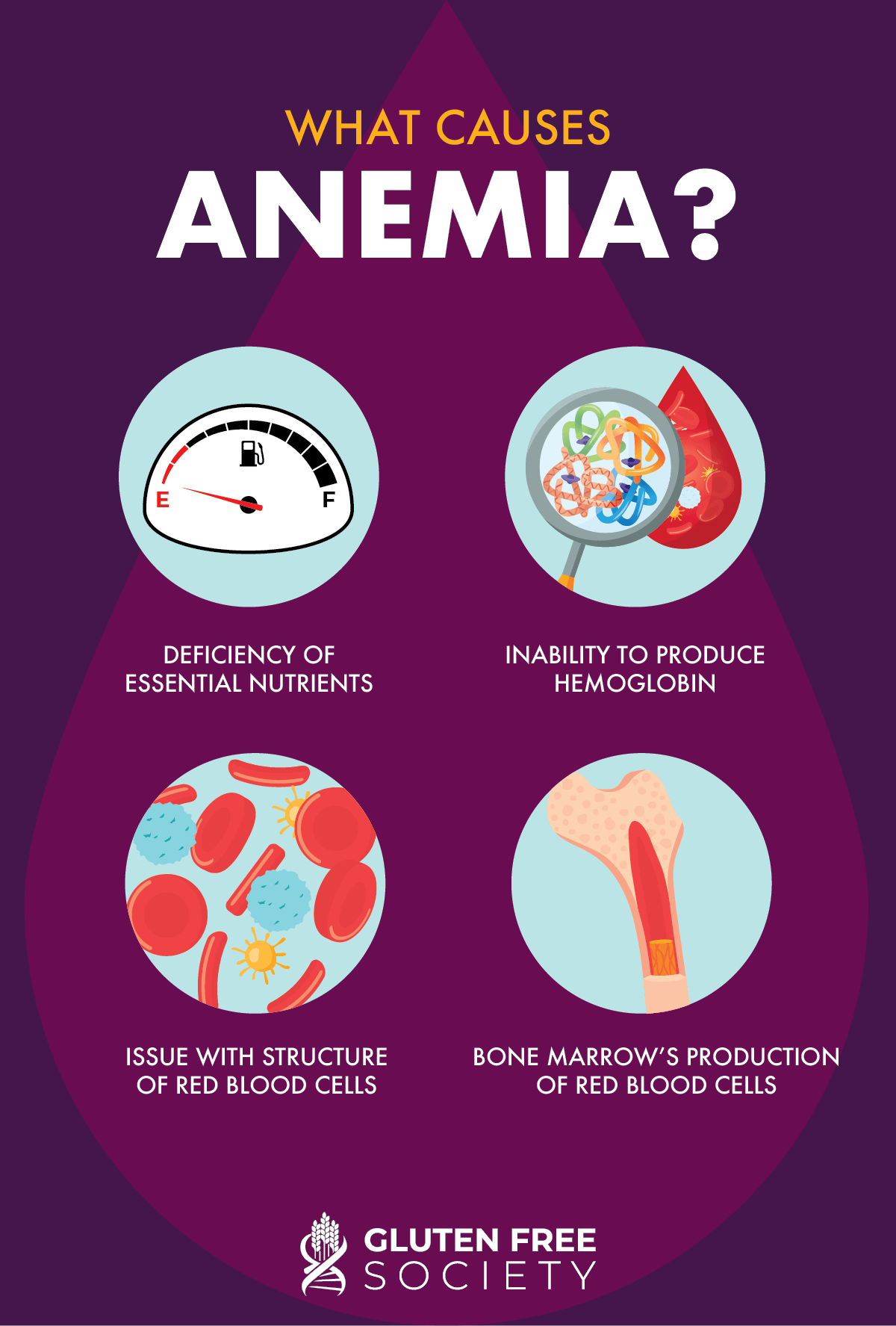
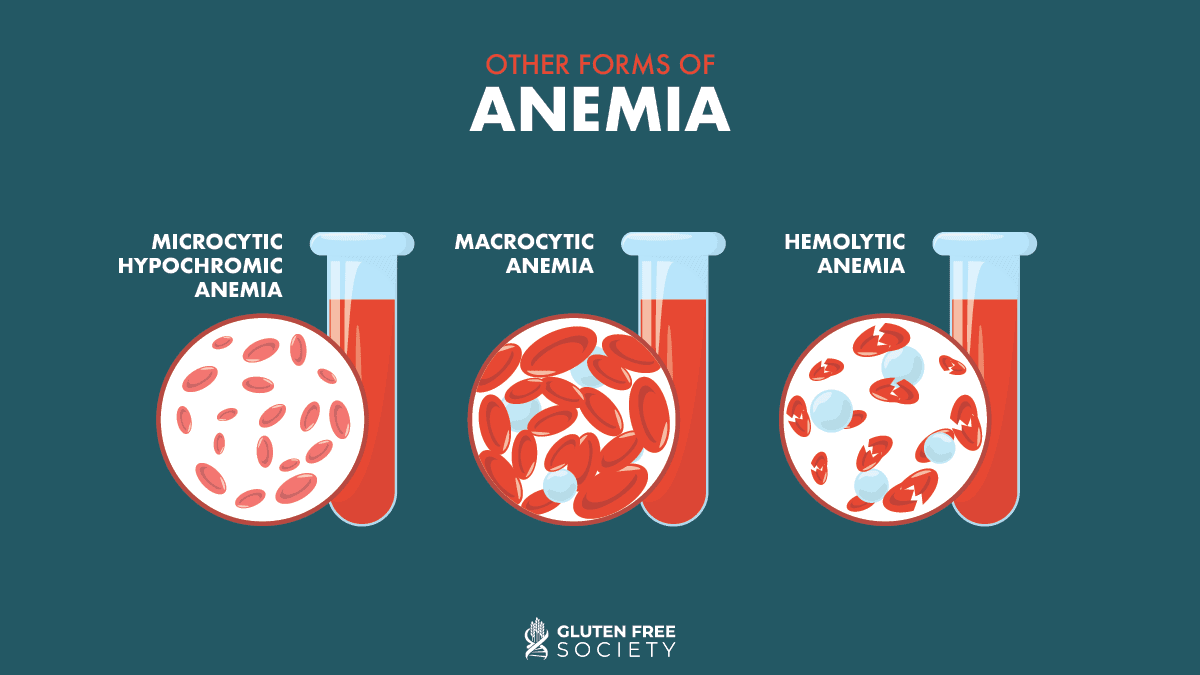
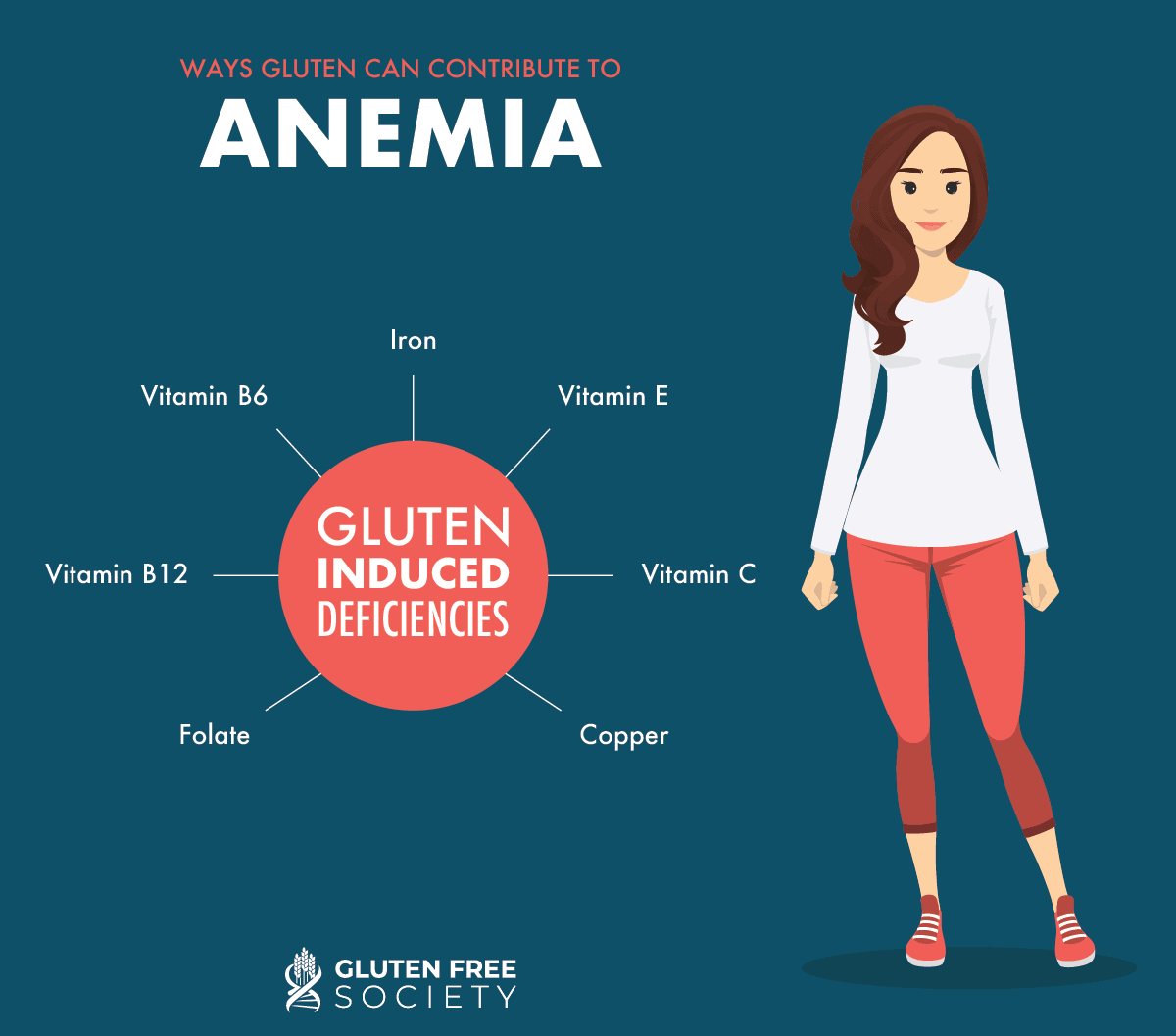 Deficiencies of these nutrients can lead to the following other forms of anemia:
Deficiencies of these nutrients can lead to the following other forms of anemia:
Written and medically reviewed by Dr. Peter Osborne. Updated on April 29, 2021
Stay up-to-date with the latest articles, tips, recipes and more.

*These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure or prevent any disease.
If you are pregnant, nursing, taking medication, or have a medical condition, consult your physician before using this product.
The entire contents of this website are based upon the opinions of Peter Osborne, unless otherwise noted. Individual articles are based upon the opinions of the respective author, who retains copyright as marked. The information on this website is not intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice. It is intended as a sharing of knowledge and information from the research and experience of Peter Osborne and his community. Peter Osborne encourages you to make your own health care decisions based upon your research and in partnership with a qualified health care professional.
2 Responses
Thanks so much for this information. Doctors have been playing with supplemental iron for my daughter (Coeliac) for years..try this type, that type ..but not have not resolved the issue. Currently working with an alternative practitioner. Hoping for some improvement. As a coeliac my iron levels are not too bad but no gall makes for some other interesting absorption/nutrient issues. Cannot gain weight.
Please keep up the interesting articles and keep us searching for the answers for our individual problems.
I have dermatitis herpetiformis, And geographic tongue. I have stop all grains and dairy,can you tell me what does my symptoms tell you that I need to help this issues… thank you