
You can eat “clean,” take a multivitamin, and still be running on empty.
Why? Because deficiencies are rarely about willpower. They are about physiology. Absorption, medication side effects, stress chemistry, ultra-processed foods, immune reactions to grains, and toxin load can all drain your nutrient reserves faster than you can refill them.
Below are the 6 biggest drivers I see, plus what to do about each one. What causes vitamin & mineral deficiencies? Let’s Dive in.
TL;DR
Vitamin and mineral deficiencies aren’t just caused by poor diet. They often result from poor digestion and absorption, medication use, chronic stress, processed foods, gluten-related gut damage, and toxic overload. You can eat well and still be deficient if your body can’t properly absorb and use nutrients. That’s why testing at the cellular level — not just relying on standard blood labs — matters.
Contents
ToggleThe “Hidden Truth” About Deficiencies
Your body is not a simple input-output machine. Nutrients only count if you can:
- Digest them
- Absorb them
- Transport them
- Activate them
- Use them inside cells
When any part of that pipeline breaks, deficiencies show up even with “normal labs” and “good diets.”
#1: Broken GI Tract Absorption
If your gut is inflamed, leaky, low in stomach acid, or dysbiotic, you can eat well and still develop deficiencies.
Here’s a simple breakdown of your digestive tract and other factors needed for healthy absorption:
Digestion Starts in the Mouth
Physical breakdown begins with chewing. Chemical breakdown happens through digestive enzyme secretions in your saliva. If you have oral health issues, these problems can make it harder to extract nutrients from your food.
Stomach Acid
Stomach acid helps liberate minerals and supports proper digestion and breakdown of proteins. When acid is low, digestion slows and absorption often suffers. This is one reason acid-reducing drugs can backfire long-term (more on that in section #2).
Liver and Bile Flow
Your liver produces bile. Bile helps emulsify fats so you can absorb fat-soluble vitamins A, D, E, and K. When bile flow is impaired (cholestasis and other bile-related issues), fat absorption drops and fat-soluble vitamin deficiency risk rises.
Pancreatic enzymes
Your pancreas provides enzymes that digest fat and protein. When enzyme output is low (exocrine pancreatic insufficiency, chronic pancreatitis, post-surgery changes), nutrient malabsorption becomes predictable. In chronic pancreatitis and pancreatic insufficiency, deficiencies of fat-soluble vitamins are common, and protein digestion issues can impair B12 handling.
Gut Inflammation & Malabsorption Conditions
Many inflammatory GI disorders that impair fat absorption can reduce fat-soluble vitamin uptake. Inflammation to the GI tract can also contribute to water soluble vitamin and mineral deficiencies. Common inflammatory conditions include celiac disease, Crohn’s, ulcerative colitis, and pancreatitis.
Action steps
If you have bloating, greasy stools, floating stools, unexplained weight loss, chronic reflux, or chronic diarrhea, do not assume it is “normal.”
Talk with your clinician about evaluating:
- Pancreatic function (especially if stools are oily or you have upper abdominal symptoms)
- Bile flow and liver markers
- Celiac and gluten-related genetic markers or antibody tests.
Read the following comprehensive breakdown on digestion for more detailed information.
#2: Medications Drain Nutrients
This is one of the most under-discussed causes of nutrient depletion in modern medicine.
Proton pump inhibitors (PPIs) and acid reducers
Long term PPI use has been associated with increased risk of deficiencies involving protein, vitamin B12, iron, calcium, magnesium, zinc and vitamin C metabolism.
That matters because low acid can reduce the breakdown and release of nutrients from food. These nutrient deficits can in turn effect the functionality of the gut, creating a vicious circle.
Metformin
Metformin, a diabetic medication, is most well known for causing vitamin B12 deficiency Additionally, it has also been linked to folate and CoQ10 deficiency.
If you are on metformin and you start to develop tingling, numbness, burning feet, fatigue, or anemia, you should ask you doctor to immediately check your B12, folate, and CoQ10 levels, as a deficiency of these key nutrients are known to cause this symptom cluster.
Statins
Statins have been shown to block CoQ10 production in clinical trials, with multiple analyses reporting significant reductions.
Why this matters: lowered CoQ10 is linked to nerve damage, muscle pain, fatigue, weakness, and cramping. All of these are factors that can lead to exercise avoidance, but also more serious complications. If you are taking statins, strongly consider both monitoring your levels as well as supplementing with CoQ10.
Blood Pressure Medications
Diuretics can increase urinary loss of both vitamins and minerals. Nutrients known to be commonly depleted include, vitamin B1, B6, B9, magnesium, calcium, potassium, zinc, and CoQ10.
The irony is that deficiencies of these nutrients can elevate blood pressure and heart disease risk. If you are taking blood pressure medicines, make sure to ask your doctor to monitor your levels, and supplement accordingly.
Steroids (glucocorticoids)
Steroids commonly prescribed to reduce pain and inflammation can reduce intestinal calcium absorption and increase urinary calcium loss, contributing to bone loss risk over time. Additionally, these medications can deplete vitamin D, magnesium, potassium, zinc, selenium, vitamin C, vitamin A, folate, B6 and B12.
NSAIDs (aspirin, ibuprofen, naproxen, etc.)
Non steroidal anti-inflammatories (NSAID’s) can cause damage to the stomach and intestinal lining. This is often associated with occult bleeding that contributes to iron loss and deficiency. In addition, NSAIDS can deplete folate and vitamin C.
Tylenol (acetaminophen)
Acetaminophen is metabolized into a toxic intermediate (NAPQI) that is detoxified by glutathione. This process can deplete glutathione stores, especially in overdose but also as a core part of the pathway.
Hospitals give N-Acetyl Cysteine, a direct precursor that increases glutathione to patients with acetaminophen overdose.
SSRIs and electrolyte depletion
SSRIs are strongly associated with hyponatremia (low sodium) Low sodium can cause headaches, nausea, muscle aches, cramps, and fatigue. In addition, these medicine have been associated with lower vitamin D and calcium, increasing the risk for bone loss.
Hormones (HRT and birth control)
Oral contraceptive have been linked to many nutritional deficiencies, including CoQ10, B vitamins and minerals like magnesium, selenium, copper, and zinc.
With an increased popularity of women taking estrogen long term, there is a greater concern for the development of deficiencies that can contribute to health issues. If you are taking estrogen or HRT, ask your doctor for an intracellular nutrient analysis (INA).
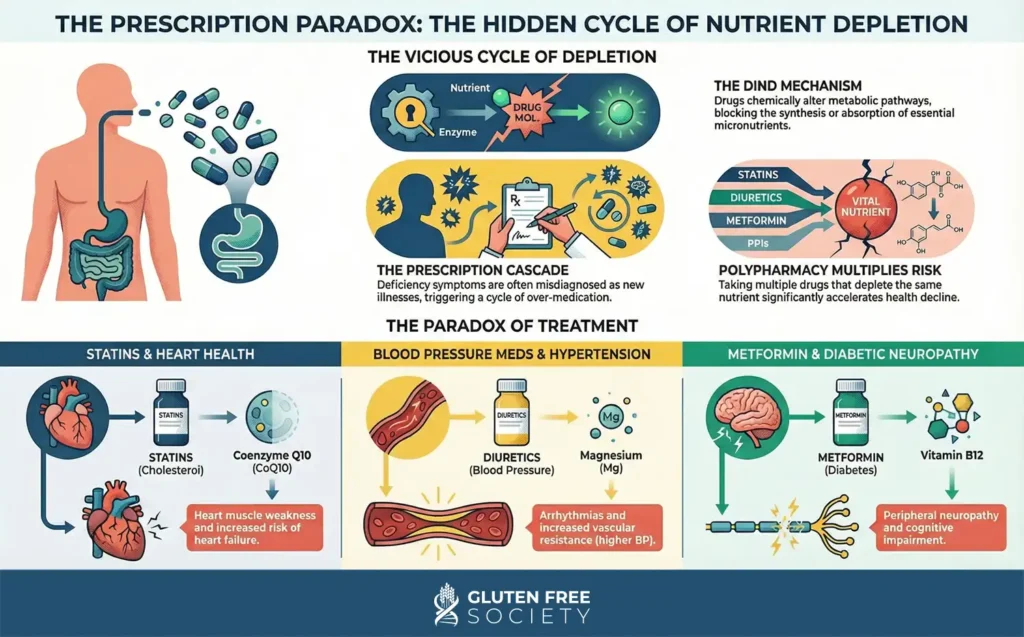
The diagram below illustrates additional drug induced nutritional deficiencies:
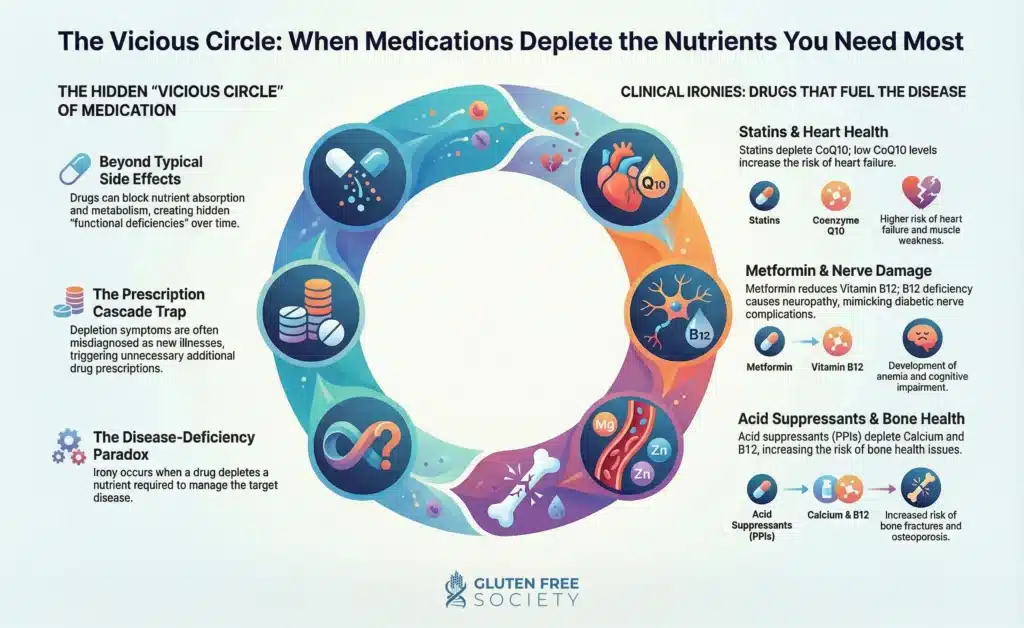
Bottom line:
- If you are taking prescription medications, Test, Don’t Guess when it comes to preventing nutritional problems.
- Ask your clinician: “Which nutrients does this medication deplete, and what should we monitor?”
- Do not stack supplements blindly. Identify your deficiencies first.
Testing: Why I like Intracellular Nutrient Analysis (INA)
Standard blood tests can be helpful, but they do not always reflect functional nutrient status inside cells.
Intracellular Nutrient Analysis (INA) is designed to assess functional deficiencies at a cellular level where the nutrients work.
In plain terms:
- Serum can look “normal” while tissues are struggling.
- INA identifies whether or not your cells on functioning properly based in their nutrient adequacy.
This is especially worth considering if you have symptoms, chronic inflammation, gut issues, toxin exposure, or long-term medication use.
#3: Chronic Stress
Stress is not just a feeling. It is a biochemical state. Chronic stress burns through your nutritional reserve tank.
When stress stays “on,” your body shifts into a fight or flight state leading to:
- higher demand for energy metabolism
- higher turnover of neurotransmitters
- higher oxidative stress burden
- higher stress hormone synthesis demands
This shift in biochemistry increases the body’s demand for vitamins and minerals. Subsequently, chronic stress has been linked to deficiencies in zinc, calcium, magnesium, iron, vitamin C, and B vitamins.
Many people turn to heavy caffeine use to overcome stress induced fatigue and a vicious cycle ensues. When done in excess, caffeine intake (more than 400 mg/day) has been shown to deplete nutrients. In addition, high stress pushes people toward convenient ultra processed food choices devoid of adequate nutrients.
Action steps
If you are burned out and wired, treat stress like a medical risk factor. Start with the basics daily choices that can have the biggest impact:
- Sleep timing and consistency
- Exercise to tolerance only
- Hydration and electrolytes
- Eat real food (Avoid processed)
- Process your emotions and give yourself forgiveness and grace
- Consider taking a high potency multi-vitamin/mineral.
#4: Sugar, Soda, Alcohol, & Ultra-Processed Foods (overfed, undernourished)
Consumption of empty calories, alcohol, chemical preservatives, and pesticides create a nutritional deficiency time bomb. This behavioral pattern has been the standard norm for the past several decades. The outcome? A nation of malnourished, disease laden people turning to medications as a means to manage the symptoms largely caused by poor dietary decisions.
Ultra-processed foods (UPFs) displace micronutrients and are linked to chronic diseases, UPFs often deliver high amounts of:
- Refined starch
- Refined oils
- Added sugar
- Synthetic preservatives and flavors
- Processed food gums and artificial sweeteners
- Microplastics
- Pesticides
- Toxic Metals
- Low micronutrient density
Alcohol: a proven deficiency accelerator
Chronic alcohol intake is has long been linked to severe nutritional problems. Over the past many years, there has been an industry driven social push to normalize alcohol as safe and non problematic. Take for example the fact that wine has been recommended by cardiologists as “heart healthy”, despite the fact that it is a known toxin that causes vitamin and mineral deficiencies.
Action steps
Replace liquid calories first. Remove soda and reduce alcohol. Build your plate around healthy grain free ingredients:
- Nutrient dense, organic whole foods
- Grass fed/finished meats
- Free range, organic chicken and eggs
- Wild caught fish
- Organic fruits, vegetables, and nuts.
If you rely on protein powders or packaged “health foods,” choose brands that provide transparent contaminant testing where possible.
#5: Gluten & Grain Consumption
This is not about trendy dieting. This is about immune biology and gut integrity. The evidence for grains driving nutritional deficiencies is clear. I wrote extensively about this in my book No Grain No Pain.
When the gut lining is damaged, malabsorption becomes the norm. Autoimmune inflammation from grains drives up stress hormones, causes tissue damage, and drives demand on nutrients needed for healing and repair. The cycle is known as Grainflammation.
If you want clarity about whether a gluten free diet is right for you, consider taking our gluten quiz, having genetic testing performed, or visiting with a doctor who is gluten literate. You can learn more about how gluten causes vitamin and mineral deficiencies here.
#6: Food Chemicals & Environmental Toxins
Detox is not a fad word. Your body has dedicated pathways to help you process and eliminate chemicals and environmental toxins.
Those pathways rely on vitamins and minerals for proper function. Processed foods are heavily contaminated with chemical additives, emulsifiers, and preservatives. The presence of these compounds drives up demand for nutrients in order to help the body process and eliminate them.
When environmental toxic exposures from pesticides, herbicides, microplastics, toxic metals, toxic molds, mycotoxins, and medications are added to this burden, detox pathways can become overwhelmed, and nutritional deficiencies are often the consequence.
Detox Requires Nutrients
Detoxification is a complex, two phase process occurring primarily in the liver. The goal is to transform fat soluble toxins into water soluble substances that can be safely eliminated from the body through urine, sweat, and the bowels.
Phase I detoxification relies on a family of enzymes known as cytochrome P450 (CYP450). During this phase, CYP450 enzymes use chemical reactions to break the toxin down into something smaller. This first step leads to the formation of free radicals. If the body lacks adequate nutrient antioxidant defenses, these free radicals can create to other cells.
The main nutrients required for Phase I include:
- B-vitamins (B2, 3, 6, 9, and 12)
- Magnesium & Zinc
- Glutathione
- Antioxidants – vitamin E, C, and selenium
Phase II detoxification acts to safely package and neutralize the reactive compounds generated during Phase I. In this stage, enzymes attach (or conjugate) a water-soluble molecule to the toxin. This conjugation effectively “wraps” the toxin, neutralizing its harmful effects and transforming it into a water-soluble compound that can be safely excreted form the body through the GI tract, urine, or sweat.
The main nutrients required for Phase II include:
- Vitamins – B1, B5, folate, B6, B12, and Vitamin C
- Minerals – Magnesium, molybdenum, selenium, sulfur
- Amino Acids – Methionine, Glycine, Taurine, Glutamine, Cysteine
- Glutathione
- Betaine
- Water
Bottom Line:
The more toxins your are exposed to, the more nutrients your liver needs to process and eliminate them.
#7: Bonus – What Else Causes Vitamin and Mineral Deficiencies?
Lack of nutrient intake
Poor soil quality has become increasingly depleted due to modern farming practices. This means that we could eat the same food today as our grandparents did a few decades ago and we get fewer nutrients.
Phases of Life
Certain phases of life demand a higher nutrient intake. If you don’t meet that need, you can easily become depleted. Some examples include the following:
- Growth spurts: Baby, children, and adolescents are growing quickly and they require more nutrients to accommodate their growth spurts. For example, adolescents are more likely to develop zinc deficiency as their body is growing because the body requires more zinc during this time.
- Pregnancy: Pregnancy is among the most nutritionally demanding phases of life, as the nutrients a pregnant woman consumes must cover the needs of herself as well as her growing baby.
- Breastfeeding: Like pregnancy, breastfeeding involves a woman feeding and nourishing both herself and her baby.
- Increased or intense exercise: Exercise has wonderful benefits for the body but is also a muscular trauma that requires nutrients for healing and repair, and regrowth of the tissue. This results in a higher demand for nutrients in order to heal and repair the damage induced by the exercise.
- Trauma: Similar to exercise, trauma in the form of a sprain, tissue damage, a broken bone, injury, or other traumatic event requires additional nutrients for healing and repair.
- Chronic inflammatory disease: Chronic diseases like diabetes, autoimmune disease, and celiac disease cause increased inflammation in the body, which results in heightened nutrient needs to help manage the inflammation.
Increased loss of nutrients
Certain conditions and situations cause the body to lose nutrients at a faster rate, making a deficiency more likely. Such conditions include the following:
- Kidney disease: malnutrition in those with chronic kidney disease results from a combination of a number of issues, including decreased appetite and nutrient intake, hormonal derangements, metabolic imbalances, inflammation, increased catabolism, and dialysis related abnormalities.
- Burns: nutrients can be lost through a burn
Aggressive skin inflammation: psoriasis or eczema lose proteins and nutrients more aggressively) - Surgical procedures: Certain surgical procedures performed on various components of the digestive system can influence nutrient absorption. For example, gastric bypass affects the stomach, cholecystectomy (removal of the gallbladder) impacts bile secretion and fat absorption, and intestinal resection results in less area for nutrients to be absorbed.
How to Reduce Your Risk of Developing Nutritional Deficiencies
Diet and lifestyle choices can have a profound impact on your nutritional status. Consider the following to preserve and optimize your body’s nutritional bank account.
Make Good Choices
- Eat whole, nutrient dense, organic foods with minimal to no processing
- Use safe, non toxic cookware
- Filter your water
- Filter your air
- Use natural hygiene and self care products
- Use natural house hold cleaning products
- Get regular sunshine exposure
- Go outside and get exposure to nature. Flowers, trees, animals, etc
- Limit your screen time. Excessive blue light exposure and EMF can also drive nutritional deficits
- Get enough sleep
- Exercise and move your body
- Manage your relationships and set clear boundaries to reduce stress
- Have fun – Don’t forget that the pursuit of improving your health to extreme degrees can create stress. Make sure you are living a life of purpose and fulfillment.
Test, Don’t Guess
If you are making great choices, but still struggling in your health, consider having your nutritional status checked. Have an intracellular nutrient analysis (INA) performed. Customize your food choices to your deficits. Consider supplementation. If this feels overwhelming, work with an experienced nutritional expert.
FAQ: What Causes Vitamin & Mineral Deficiencies?
What is the most common cause of vitamin and mineral deficiencies?
In real life, it is usually a combination of poor absorption, medication-related depletion, and ultra-processed diets. For many people, chronic gut inflammation is the root that drives the rest.
Which companies offer home test kits for detecting vitamin deficiencies?
There are many companies offering serum lab testing, but they do not always reflect nutritional status accurately.
The Intracellular Nutrient Analysis (INA) test is the most accurate and reliable test to help determine functional deficiencies at a cellular level. INA testing is available through Dr. Osborne and through Gluten Free Society.
Can you be overweight and still be nutrient deficient?
Yes. You can be high-calorie and low-nutrient at the same time. That is one of the signatures of ultra-processed diets.
Which medications are most associated with nutrient depletion?
Common categories include:
PPIs (B12, iron, calcium, magnesium)
Metformin (B12, also discussed with folate and others)
Statins (lower circulating CoQ10)
Diuretics (B vitamins, magnesium and other mineral losses)
Steroids (reduced calcium absorption and bone effects)
NSAIDs (GI injury and occult blood loss leading to iron deficiency)
Why do my labs look normal if I feel deficient?
Serum labs do not always reflect true nutritional status. Nutrients work in the cell. Measuring levels in the blood or serum can be misleading. That is one reason people consider Intracellular Nutrient Analysis (INA) home test kit from Dr. Osborne’s website to evaluate functional cellular status.
Where can I find a specialist to assess my nutrient levels?
Doctors do not typically train in nutrition. That’s why most will run a basic panel, tell you your labs are “normal,” and send you home with no answers. That is exactly why people stay sick and stay deficient. If you want a root-cause approach, you need a clinician who looks at:
Symptoms plus labs, not labs alone
Digestion, absorption, gut inflammation, and medication depletion
Gluten and other food sensitivity risk factors
A plan that includes food, lifestyle, and targeted support
Work with Dr. Osborne’s team through Origins Wellness Center. The focus is not just identifying deficiencies. The focus is why your body is running low and how to correct it.
What are the best supplement brands for addressing common deficiencies?
If you want to address deficiencies effectively, you want two key things:
1. Quality and clean sourcing
2. Bio-available forms and doses
Dr. Osborne’s supplement line offers both. You can view his full catalogue of high quality nutritional supplements here.






