Contents
ToggleWhy Celiacs and Those with Non Celiac Gluten Sensitivity Should Get More Sunshine
Sunshine is one of nature’s greatest gifts, but advice from mainstream media and traditional medical resources might have you believing otherwise. If you have heard recommendations to avoid sun exposure to reduce the risk of skin cancer, you’re not alone! Unfortunately, this advice is not only outdated and unfounded, it can actually be dangerous, especially to those with gluten sensitivity and celiac disease.
This article will look at why this is the case. We will discuss:
- The importance of getting regular sunlight exposure
- Vitamin D and sunlight
- The relationship between melatonin, serotonin, cortisol and sunlight
- How sunlight influences endorphins
- How sunlight is needed to regulate inflammation and immune function
- The connection between celiac disease, gluten sensitivity, and sunshine
Why it is Important to Get Regular Sunlight Exposure
It is true that excessive exposure to the sun’s UVA and UVB rays can cause sunburn and other health concerns. However, the 2006 World Health Organization (WHO) report titled “The Global Burden of Disease Due to Ultraviolet Radiation” shows that exposure to the sun’s rays accounts for only 0.1% of the total global burden of disease in disability-adjusted life years (DALYs). DALYs measure how much a person’s expectancy of healthy life is reduced by premature death or disability caused by disease. In other words, the true impact of excessive sun exposure on one’s health is quite limited. When considering the health benefits associated with sun exposure, it becomes clear that the benefits outweigh the risks.
Health benefits of sunshine
There are a number of significant health benefits associated with sunshine exposure as discussed below.
1.Vitamin D production
Vitamin D deficiency affects almost 50% of the population worldwide. In the United States, the overall prevalence rate of vitamin D deficiency is approximately 41%, with the highest rate seen in blacks (82%), followed by Hispanics (69%). For this survey, vitamin D deficiency was defined as a serum 25-hydroxyvitamin D concentration of ≤20 ng/mL (50 nmol/L), but optimal levels of vitamin D status are actually much higher, at 30-100 ng/mL.
Unlike other essential vitamins that must be obtained from diet or supplementation, vitamin D can be synthesized in the skin through a photosynthetic reaction triggered by exposure to the sun’s UVB rays.
These widespread deficiencies can primarily be attributed to limited sunlight exposure (from outdoor time and/or excessive use of sun blocking means like sunscreen and skin cover) as well as environmental factors like air pollution that reduce exposure to sunlight, which is required for vitamin D production in the skin.
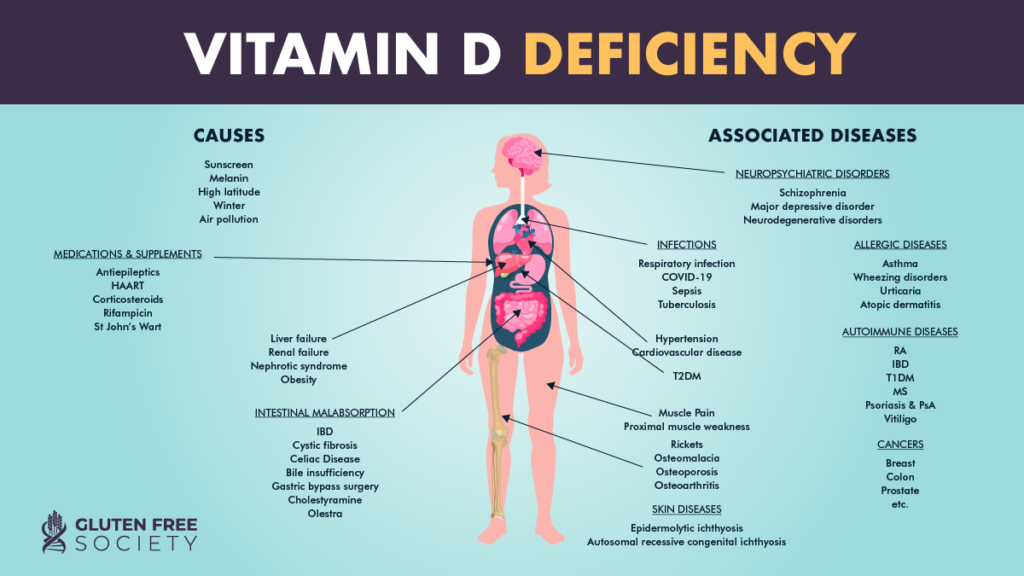
Vitamin D deficiency is a risk factor for a number of diseases. And in fact, emerging research supports the possible role of vitamin D against cancer, heart disease, fractures and falls, autoimmune diseases, influenza, type-2 diabetes, and depression. Current studies suggest that we may need more vitamin D than presently recommended to prevent chronic disease. Research also suggests that increasing serum 25(OH)D levels is the most cost-effective way to reduce global mortality rates, as “the cost of vitamin D is very low and there are few adverse effects from oral intake and/or frequent moderate UVB [exposure] with sufficient body surface area exposed.”
Vitamin D deficiency is also common in those with celiac disease, as it is absorbed through diet and supplementation in the small intestine, which is generally impaired in those with celiac disease. Furthermore, for those with gluten issues, vitamin D deficiency can exacerbate and contribute to the development of autoimmune diseases.
2. Melatonin, serotonin, and cortisol regulation
Research shows that vitamin D helps to regulate melatonin, serotonin, and cortisol in the body.
Melatonin is a hormone produced by the brain in response to darkness. It supports the timing of the body’s circadian rhythms and with sleep. Sunlight helps to regulate melatonin production, which in turn affects sleep quality and a number of other health parameters associated with sleep.
Serotonin is a neurotransmitter or chemical messenger that is believed to help regulate mood. One study found that the rate of production of serotonin by the brain was directly related to the prevailing duration of bright sunlight. Serotonin rose rapidly with increased luminosity. The study suggests that changes in the release of serotonin by the brain, which can be triggered by the sunlight underlie mood seasonality and seasonal affective disorder.
Cortisol is a hormone involved in the body’s stress response. Research shows that sunlight induces gene expression in the adrenals, helping to regulate the body’s response to stress.
3. Endorphin production
Endorphins are considered natural opiates and often referred to as “feel good hormones.” UV rays increase blood levels of endorphins, which in turn leads to enhanced mood and well being. In fact, the June 2003 Journal of Investigative Dermatology, and a study published in November of 2005 in Molecular and Cellular Endocrinology suggest that the cutaneous pigmentary system is an important stress-response element of the skin.
4. Inflammation and Immune Regulation
Research shows that sunlight, through vitamin D and melatonin, also helps to support a healthy inflammatory response and helps to regulate the immune system.
What does all of this have to do with gluten?
People with celiac disease and gluten sensitivity are at greater risk for vitamin D deficiency due to dietary malabsorption. This makes exposure to sunlight a major factor for maintaining adequate vitamin D status and for maintaining optimal health and helping to prevent a number of disease conditions.
Furthermore, the relationship between vitamin D status and celiac disease may work in the opposite direction as well. Research suggests that lack of sunshine and vitamin D deficiency can serve as a risk factor for the development of celiac disease.
As there is a significant overlap in symptoms between gluten sensitivity and vitamin D deficiency symptoms, it is important to test for both conditions in order to help manage and mitigate risk for both. Shared symptoms include depression, sleep disruption, osteoporosis, arthritis, myalgia, cancer, and multiple sclerosis.
What about sunscreen?
So if sunlight is critical to vitamin D sufficiency, should you skip sunscreen altogether? If you will be exposed to direct sun for extended periods of time, sunscreen can be a smart choice to avoid sunburn. However, excessive use for mild daily exposure (for example, in daily face lotion) can inhibit vitamin D absorption. In fact, vitamin D synthesis is inhibited at SPF of 8 or higher.
In addition, as with many skincare products, sunscreen is commonly filled with toxic ingredients that act as endocrine disrupting chemicals. Some commonly used toxic ingredients include oxybenzone, octinoxate, octisalate, octocrylene, homosalate and avobenzone are all systemically absorbed into the body after one use
The Environmental Working Group is a great resource for learning more about safe sunscreen. They also have a searchable database of different brands so that you can make an informed choice about the ingredients in your sunscreen.
Be Aware of Medicines That Cause Sensitivity to the Sun
Many common prescription medications can cause sun sensitivity. If you are taking any of the medicines listed below, talk with your doctor about diet and lifestyle changes that may help you discontinue their use so you can bask in the glory of the health promoting sunshine.
Antibiotics
Antifungals
Antihistamines
Diuretics
Statins
NSAIDS
Oral Contraceptives
The bottom line
Sunshine is critical to the maintenance of proper health, and the benefits outweigh the risks of moderate exposure. Particularly in those with celiac disease or gluten sensitivity, sunshine is necessary to the maintenance of proper vitamin D status which influences a number of key health promoting functions. It is also important to use good judgment. Your skin tone, and time of exposure are important factors to consider. Be safe, but don’t be scared to get regular sunshine within the limitations of your situation.