If you want accurate celiac testing, you need to be eating gluten during the diagnostic process. When you stop eating gluten, antibodies can fall and intestinal damage can start to heal within 4 months, which can make blood tests and biopsies look “normal” even when celiac disease is the real issue.
The takeaway: If you have been gluten free for 4 months or longer, and your doctor wants to send you for celiac disease testing, he will most likely recommend a gluten challenge to ensure your results are accurate.
TL;DR
For standard celiac blood tests and an endoscopy/biopsy to be accurate, you generally need to be actively eating gluten. If you’ve already reduced/removed gluten, antibody levels can fall and the intestine can start healing, increasing the risk of a false negative test result.
Contents
ToggleHow Much Gluten Should I Eat Before a Celiac Test?
How much gluten to eat + how long? There isn’t one universally-agreed “perfect” gluten challenge, but major celiac organizations commonly cite ranges like:
- ~2 slices of wheat bread daily for 6–8 weeks (NASPGHAN guidance)
- At least ~1 slice daily for ~2–3 weeks before biopsy (University of Chicago Celiac Center)
- Some clinical literature suggests 3–6 grams of gluten/day for ~12+ weeks may optimize diagnostic accuracy in certain scenarios (especially if prior gluten avoidance was long).
- If you’re already eating gluten: Don’t stop until all testing is complete.
- If eating gluten makes you very sick, make sure you let your doctor know. He/she may offer different guidance to help you get tested accurately and safely.
Scenario | What many authorities commonly advise | Why it matters |
|---|---|---|
Preparing for celiac bloodwork after being gluten-free | ~2 servings/day ≈ 2 slices wheat bread daily for 6–8 weeks (NASPGHAN guidance) | Gives antibodies time to rise reducing risk of false negatives. |
Preparing for biopsy (endoscopy) | University of Chicago center guidance often cited: ≥ 1 slice/day for ~2–3 weeks before biopsy | Helps increase odds of seeing villous injury if present. |
UK/NICE-style “normal diet” guidance | Gluten in >1 meal/day for at least 6 weeks before testing (amount not precisely specified) (NICE) | Emphasizes consistency; supports test validity. |
Higher-dose classical challenge (some adult protocols) | ~8–10 g gluten/day (~4–6 slices bread/day) for 6–8 weeks (Canadian Celiac Association description) (Celiac Canada) | Can improve signal but may be poorly tolerated. |
We know that if you have avoided gluten from your diet for a long time, you may be nervous to reintroduce it for fear of dealing with the many symptoms that can come with gluten consumption. This hesitation is understandable and valid, so always consider your own personal circumstances and work with your doctor to navigate an accurate diagnosis.
Smaller or more infrequent servings may work better for your own personal circumstances. In addition, you can consider the quality of the gluten that you choose to consume. Something like organic sourdough may cause less discomfort and have fewer other side effects than a refined and processed form of gluten.
You may also consider talking with your doctor about genetic testing combined with your history of symptoms as the primary basis for making a diagnosis of non celiac gluten sensitivity instead of celiac disease.
A gluten challenge is not recommended before the age of 5, during puberty, or during pregnancy, as the consumption of gluten can affect nutrient absorption and lead to deficiencies that may contribute to pregnancy or growth complications.
Consider This Before a Gluten Challenge
Celiac testing depends on your immune system producing measurable antibodies (and on you eating enough gluten). Anything that suppresses antibody production can increase the odds of a false negative test result. This is one reason many people suffer for years before getting a diagnosis. If any of the below apply to you, talk with your doctor before performing celiac testing.
- Taking immune suppressing medicines – NSAIDS, steroids, certain biologics, antihistamines, anti-seizure, antibiotics, and chemotherapy
- Have been diagnosed with SIBO or gut dysbiosis
- Have been diagnosed with a chronic yeast or viral infection – i.e. Candida, EBV, or CMV.
- Suspect chronic mold exposure
- Follow a low protein or vegan diet – antibody production requires adequate protein.
Safety note: Don’t stop or change any medication to “prove” a diagnosis. Always coordinate testing decisions with your prescribing clinician.
How Celiac Testing Works
There are several different options to test for celiac disease.
- Blood Testing: A blood test is available that checks for certain antibodies. People with celiac disease who eat gluten produce antibodies in their blood because their immune systems view gluten as a threat. It is important to note that you must be on a gluten-containing diet for antibody blood testing. It is also important to note that these types of tests can also be misleading, as they come back falsely negative 10-15% of the time.
- Endoscopy: An endoscopy is when a tube is inserted down your throat so that a practitioner can look at your small intestine for signs of inflammation or damage. They will also take a small biopsy of your intestines to look for the hallmark damage of celiac disease, villous atrophy**. Like blood testing, you must be eating a diet that contains gluten for this test to be accurate.
- Genetic Testing: DNA testing is a highly accurate look at your genes to understand whether you have a genetic predisposition to reacting to gluten. Many doctors use DNA testing along with a patient’s medical history to determine a diagnosis. Make sure to get a test that measures for all genes linked to both NCGS – non celiac gluten sensitivity (HLA-DQ1/HLA-DQ3) and celiac disease (HLA-DQ2/HLA-DQ8).
**Note: A biopsy finding villous atrophy can sometimes be misleading. Villous atrophy has different causes beyond gluten. Parasites, B-vitamin deficiencies, glyphosate, non steroidal anti inflammatories (NSAIDS), proton pump inhibitors (PPI’s to treat GERD), and selective serotonin reuptake inhibitors (SSRIs) used for depression and mood disorders, are all known causes of villous atrophy.
Should You Get Tested?
You might be wondering if you should get tested for celiac disease at all. Here are some instances in which you should test for celiac disease:
- If you are experiencing symptoms of celiac disease, it is best to get tested to confirm a diagnosis and rule out other potentially complicating factors
- If you know that you have a family history of celiac disease – first-degree relatives of people with celiac disease (parents, siblings and children) have a much greater risk compared to 1 in 100 in the general population
- If you have an associated autoimmune disorder or other condition, especially type 1 diabetes mellitus, autoimmune thyroid disease, autoimmune liver disease, Down syndrome, Turner syndrome, Williams syndrome, or a selective immunoglobulin A (IgA) deficiency. Research continues to link the autoimmune spectrum of diseases to gluten sensitivity.
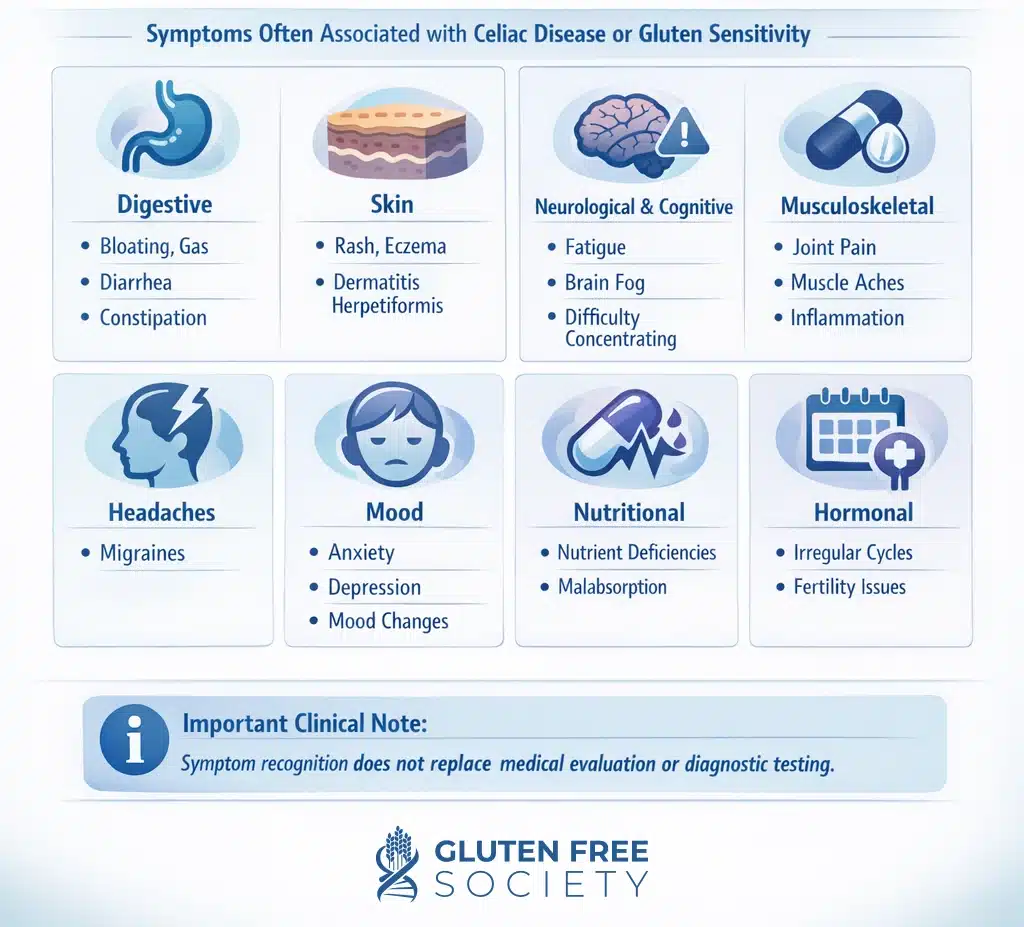
Some people prefer to use symptom recognition as an alternative to formal testing. The benefits to this are that it does not require gluten consumption prior to testing, and it is also less expensive and less invasive than some of the other methods. However, the symptoms of celiac disease and gluten sensitivity can overlap with other conditions and can vary greatly from person to person. This can make a diagnosis challenging. Common symptoms include the following:
- Digestive symptoms such as bloating, gas, diarrhea, or constipation
- Skin issues like rash, eczema, or dermatitis herpetiformis
- Fatigue, brain fog, or difficulty concentrating
- Joint pain, muscle aches, or inflammation
- Headaches or migraines
- Mood changes, depression, or anxiety
- Nutrient deficiencies due to malabsorption
- Irregular menstrual cycles or fertility issues
Despite testing flaws and potential false negatives, the best way to diagnose celiac disease is to test. If your test shows up negative, you may want to try the No Grain No Pain gluten elimination diet for a few weeks to see if that helps your symptoms. We also suggest working with an experienced functional practitioner who can help dig deeper to determine if there are other factors at play.
Conclusion
Gluten consumption is required if you are performing blood or biopsy testing to diagnose celiac disease. As an alternative to doing a gluten challenge, your doctor can give a diagnosis of non celiac gluten sensitivity based on your history combined with genetic testing.
FAQ
Should I eat gluten before a celiac blood test?
How much gluten should I eat before a celiac blood test?
Commonly cited guidance is roughly 2 servings/day (about 2 slices of wheat bread) for 6–8 weeks before testing, but protocols vary by clinician and patient situation.
How long do I need to eat gluten before testing?
Many guidelines and patient organizations cite ~6 weeks or longer (especially if you’ve been gluten-free). Some centers cite shorter minimums for certain steps (e.g., a couple weeks before biopsy), but longer challenges can improve detection in some cases.
What if I already stopped gluten – can I still get tested?
You can, but you may need a gluten challenge (reintroducing gluten for a period) to reduce false negatives. Another option is HLA genetic testing (DQ2/DQ8), which doesn’t require eating gluten, but it can’t confirm celiac by itself; it mainly helps rule it out if negative.
Can I “just eat a little gluten” for a few days?
A few days is often not enough for reliable antibody rise in many people. Many recommendations are measured in weeks, not days.
What if eating gluten makes me very sick?
Work with a clinician. Some people use a modified approach (lower dose/longer duration) or discuss alternatives to traditional testing. Don’t push through severe symptoms without medical guidance.
What tests are typically used for celiac screening?
Most workflows start with blood tests, and many proceed to endoscopy/biopsy if positive. Patient organizations summarize this “blood test → biopsy confirmation” flow.
Why can tests be falsely negative?
False negatives can occur from reduced gluten exposure, IgA deficiency, early/mild disease, patchy intestinal damage, or timing/test selection.







One Response
Hopefully this will give me some insight.