 A recent research report identified an individual with progressive nerve damage findings mimicking the autoimmune neurological condition known as Lou Gehrig’s disease (AKA – ALS or amyotrophic lateral sclerosis). The condition manifests as progressive muscle weakness and loss, involuntary spasms and twitches, and eventually a degeneration of the muscles responsible for aiding in breathing. Many sufferers of ALS die as a result of suffocation once the muscles of respiration become paralyzed.
A recent research report identified an individual with progressive nerve damage findings mimicking the autoimmune neurological condition known as Lou Gehrig’s disease (AKA – ALS or amyotrophic lateral sclerosis). The condition manifests as progressive muscle weakness and loss, involuntary spasms and twitches, and eventually a degeneration of the muscles responsible for aiding in breathing. Many sufferers of ALS die as a result of suffocation once the muscles of respiration become paralyzed.
There are many theories on the causes of ALS. One prominent suspicion is in a defective antioxidant gene called SOD1(superoxide dismutase). This gene is a powerful antioxidant that is activated by the two essential minerals, copper and zinc. Patients with ALS often have this genetic variant that predisposes areas in the brain and spinal cord to free radical damage.
As ALS is an autoimmune condition, the next question becomes – does gluten play a role in the development or contribute to the disease?
Is There a Gluten – ALS Connection?
The following is the abstract published from the American Journal of Neuroradiology…
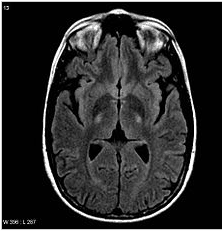
CD is an autoimmune-mediated disorder of the gastrointestinal tract. Initial symptom presentation is variable and can include neurologic manifestations that may comprise ataxia, neuropathy, dizziness, epilepsy, and cortical calcifications rather than gastrointestinal-hindering diagnosis and management. We present a case of a young man with progressive neurologic symptoms and brain MR imaging findings worrisome for ALS. During the diagnostic work-up, endomysium antibodies were discovered, and CD was confirmed by upper gastrointestinal endoscopy with duodenal biopsies. MR imaging findings suggestive of ALS improved after gluten-free diet institution.
Source: AJNR Am J Neuroradiol. 2010 May;31(5):880-1. Epub 2009 Nov 12.
Yes, A Connection Exists
This group of clinicians found a strong correlation in one of their patients, and this is not the only time this connection has been made in medicine (see resources). Why is this an important connection? ALS is a terminal disease with no known cure. The medications being prescribed to treat it are not effective. The quality of life in these patients can deteriorate rapidly and they most often need 24 hour care. This case demonstrates that the hallmark signs of damage in the brain identified by MRI improved after a gluten free diet was implemented.
Gluten Induced Nerve Damage is not a New Discovery
Neurologic diseases linked with gluten sensitivity and celiac disease were initially reported in the medical literature in 1966. The most common manifestations are ataxia, vertigo (dizziness) and neuropathy, followed by epilepsy (seizures), ALS and multiple sclerosis-like symptoms. It is thought that these conditions result from two key components:
- Gluten induced intestinal damage leading to vitamin and mineral deficiencies. Secondarily, these deficiencies cause neurological pathology.
- Gluten acts as a neurotoxin and induces an autoimmune process.
- Cooke WT, Smith WT. Neurological disorders associated with adult celiac disease. Brain 1966;89:683–722
- Hadjivassiliou, M, Gibson A, Davies-Jones CA, et al. Does cryptic gluten sensitivity play a part in neurological illness? Lancet 1996;347:369 –71.
- Hadjivassiliou M, Gru¨newald RA, Lawden M, et al. Headache and CNS white matter abnormalities associated with gluten sensitivity. Neurology 2001; 56:385–88
- Kieslich M, Erra´zuriz G, Posselt HG, et al. Brain white-matter lesions in celiac disease: a prospective study of 75 diet-treated patients. Pediatrics 2001;108:E21
- Lea ME, Harbord M, Sage MR. Bilateral occipital calcification associated with celiac disease, folate deficiency, and epilepsy. AJNR Am J of Neuroradiology 1995;16:1498 –500
- Turner M, Chocan G, Quaghebeur G, et al. A case of celiac disease mimmicking amyotrophic lateral sclerosis. Nat Clin Pract Neurol 2007;3:581–84
All the best,
Dr. O





4 Responses
My mother died two yrs ago in diagnosed ALS. Eventhough she died at the age of 83, she had CD for a long time undiagnosed from her thirties – forties. Then diagnosed CD. I haven’t eaten bread, pasta or any type of gluten containing food since. And I don’t miss it. Its not worth it. Anyone who have had an ALS diagnosed person close by would understand this.
My dad died of ALS complications in 2011. He had all of the symptoms of gluten intolerance. I have been eating G-F for almost 14 years and obviously will continue to eat this way for my whole life.
Hello,
My husband was diagnosed with ALS 2010 ( by the most arrogant female doctor you would never want to meet),
thankfully I felt, after a set of questions and a bit of a physical exam, not even the greatest neurologist in the world could possibly diagnose ALS that quickly. She told us to get things sorted. Fortunately we have been under the care of a fantastic natural (whole of body) doctor. No ALS, just gluten sensitivity plus hyperthyroidism. Please, please do not take the first diagnosis you get as gospel, no doctor in the world is god. My husband is still here and doing well. Our family is GF, it is poison.
I am a CALS. My husband is PALS. It was hard and I cry daily but not in front of him unless we cry together. He couldn’t find anything to give him happiness or hope. We have been focusing on our faith. He was only losing his voice before we made the decision to try different medications, which significantly enhanced his condition. He received treatment for ALS/MND at uinehealth centre . c om from Canada approximately four months ago; since then, he has stopped using a feeding tube, speech is getting better by the day, sleeps well, works out frequently, and has become very active.