Contents
ToggleGluten, Grains, and Breast Cancer
October is Breast Cancer Awareness Month, an annual campaign to raise awareness about the impact of breast cancer. Is there a connection between gluten and breast cancer? Incredibly, 1 in 8 women in the United States will develop breast cancer in her lifetime. It is estimated that in 2021, 281,550 new cases of invasive breast cancer will be diagnosed and 43,600 women will die from breast cancer in women in the United States. While it is less common, men get breast cancer too. In the United States in 2021, an estimated 2,650 men will be diagnosed with breast cancer and 530 men will die.
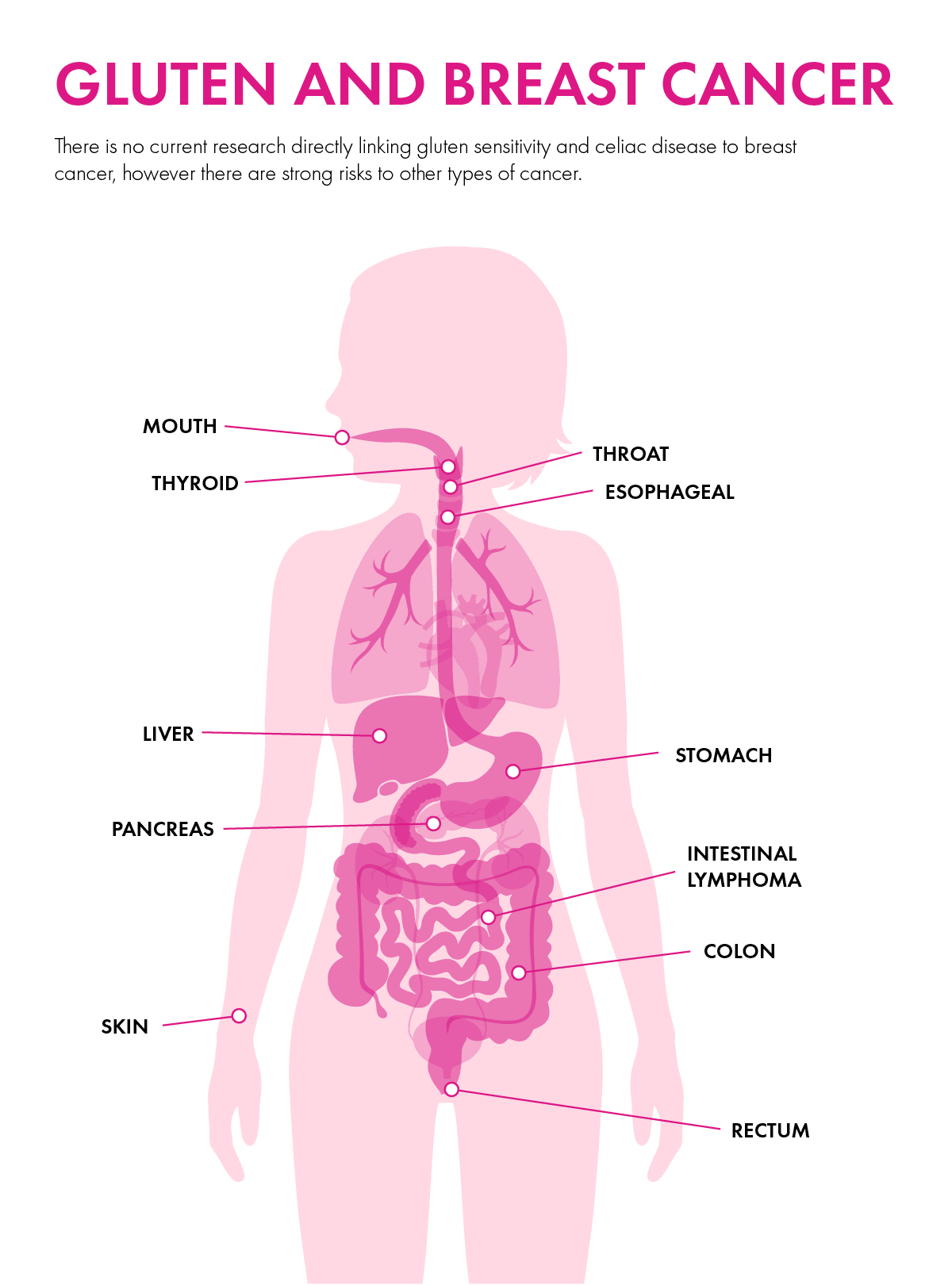
In honor of Breast Cancer Awareness Month, I wanted to take a closer look at how gluten and breast cancer may be related. Now, there is no current research directly linking gluten sensitivity and celiac disease to breast cancer (although there are links to other types of cancer). However, there are a number of conditions that are triggered by gluten consumption that can indirectly influence your risk of breast cancer.
Gluten Induced Nutritional Deficiencies Are Linked to BC
In addition, there are a number of gluten induced nutritional deficiencies that can be linked to an increased risk for the development of breast cancer. The following are the most common nutrient deficiencies that also may influence breast cancer development, mortality, and recurrence:
- Vitamin D: A wide body of research has been directed toward identifying vitamin D status as a breast cancer risk factor. Some research has found that circulating vitamin D levels (greater than or equal to 45 ng/mL) may protect against breast cancer. Another analysis found that women with the highest quintile of circulating 25(OH)D were associated with a 45% decrease in breast cancer risk when compared with those women with the lowest quantile of blood 25(OH)D.
- Vitamin C: Epidemiological studies have shown an inverse association between dietary vitamin C intake and the recurrence and mortality of breast cancer. For example, one study reported that frequent use of vitamin C supplements is associated with a decreased risk of breast cancer recurrence. Another study found that vitamin C use shortly after breast cancer diagnosis is associated with reduced mortality and recurrence risk. Vitamin C may also provide support alongside drug therapy. One study found that combining high-dose vitamin C with conventional anticancer drugs can have therapeutic advantages against breast cancer cells.
- Vitamin A: Vitamin A and carotenoids play an important role as powerful antioxidants that modulate oxidative stress and cancer development. Epidemiological evidence shows reduced breast cancer risk from retinol (animal-sourced vitamin A) and/or carotenoids (plant-sourced vitamin A) through inhibition of cell proliferation, survival, and invasion. It also suggests protective effects of vitamin A and carotenoids in breast cancer development and progression. Vitamin A may also mitigate the harmful effects of radiation in breast cancer patients.
- B Vitamins: Several B vitamins have been associated with breast cancer risk. For example, a prospective epidemiologic study found a threshold level for serum vitamin B12, below which an increased risk of breast cancer among postmeno-pausal women was observed. Another prospective study found that high folate intake was associated with decreased breast cancer risk, and that vitamin B12 intake may modify this association. The prospective cohort Shanghai Women’s Health Study found a similar association.
- Zinc: Research suggests that zinc may play a role in chemoprevention and its level may be associated with cancer risk. One study observed that serum zinc level is associated with breast cancer risk in BRCA1 carriers and noncarriers. In addition, analysis of serum zinc concentration revealed a tendency toward an increased risk of breast cancer for unselected breast cancers and BRCA1 carriers with higher zinc levels. Furthermore, exciting new research by Cardiff University and King’s College London has identified the switch which releases zinc into cells which may have implications for breast cancer prevention. This switch, known as CK2 is a protein which opens one transporter, called ZIP7, and allows the zinc to flow. Earlier research by the team already linked zinc delivery to types of breast cancer, so the discovery that CK2 opens ZIP7 suggests that drugs which block this release of zinc could also block cancer development. Early results from clinical trials of CK2 inhibitors suggest they are performing well.
- Magnesium: Magnesium is responsible for over 300 enzymatic reactions in the body, and has been linked to breast cancer risk. One study found both a direct negative association and an indirect association between dietary magnesium intake and breast cancer risk. The indirect association is driven by magnesium’s ability to influence the level of C-reactive Protein, an inflammatory marker.
- Selenium: Research has found an association between a low serum selenium levels and survival rates among breast cancer patients. In fact, one study followed up its previous five-year study and found that the 10-year actuarial cumulative survival was 65.1% for women in the lowest quartile of serum selenium, compared to 86.7% for women in the highest quartile.
Gluten Induced Fatty Liver Disease Can Increase the Risk for the Development of BC
In addition to gluten-induced nutrient deficiencies, gluten-induced fatty liver disease (non-alcoholic fatty liver disease or NAFLD) can increase the risk for breast cancer. Gluten and liver health may seem like an unlikely connection, but there is a strong link which I’ve dug into in a prior article.
Research shows that the prevalence of NAFLD in patients with breast cancer is significantly higher than in healthy controls. Moreover, breast cancer patients with NAFLD showed poorer prognosis in terms of recurrence. One study links the high levels of endogenous estrogens present in cirrhosis to an increased risk of breast cancer.
Certain Environmental Factors Are Linked to BC
While not gluten related, it is important to note that certain environmental factors can also increase one’s risk for breast cancer.
A report from the National Institute of Environmental Health Sciences shares that the chance of developing breast cancer increases with exposure to endocrine disrupting chemicals during the periods of prenatal development, puberty, pregnancy, and menopausal transition. About 300 chemicals used in personal care products, flame retardants, food processing, pesticides, and other purposes were tested and found to affect hormones known to increase breast cancer risk. Some chemicals tested may be in air and water pollution.
A case control study looked at how certain factors affect breast cancer risk. It found that environmental factors were the third most common link, behind familial or inherited factors and lifestyle factors such as poor diet and smoking.
Reduce Your Risk
While no research exists that directly links gluten and breast cancer, there are a number of ways that gluten consumption can influence your risk of developing breast cancer. Knowledge is power, so I hope this information helps to empower you to make healthy lifestyle choices that reduce your risk of developing this awful disease.