new to the gluten free journey?
new to the gluten free journey?

Contents
Toggle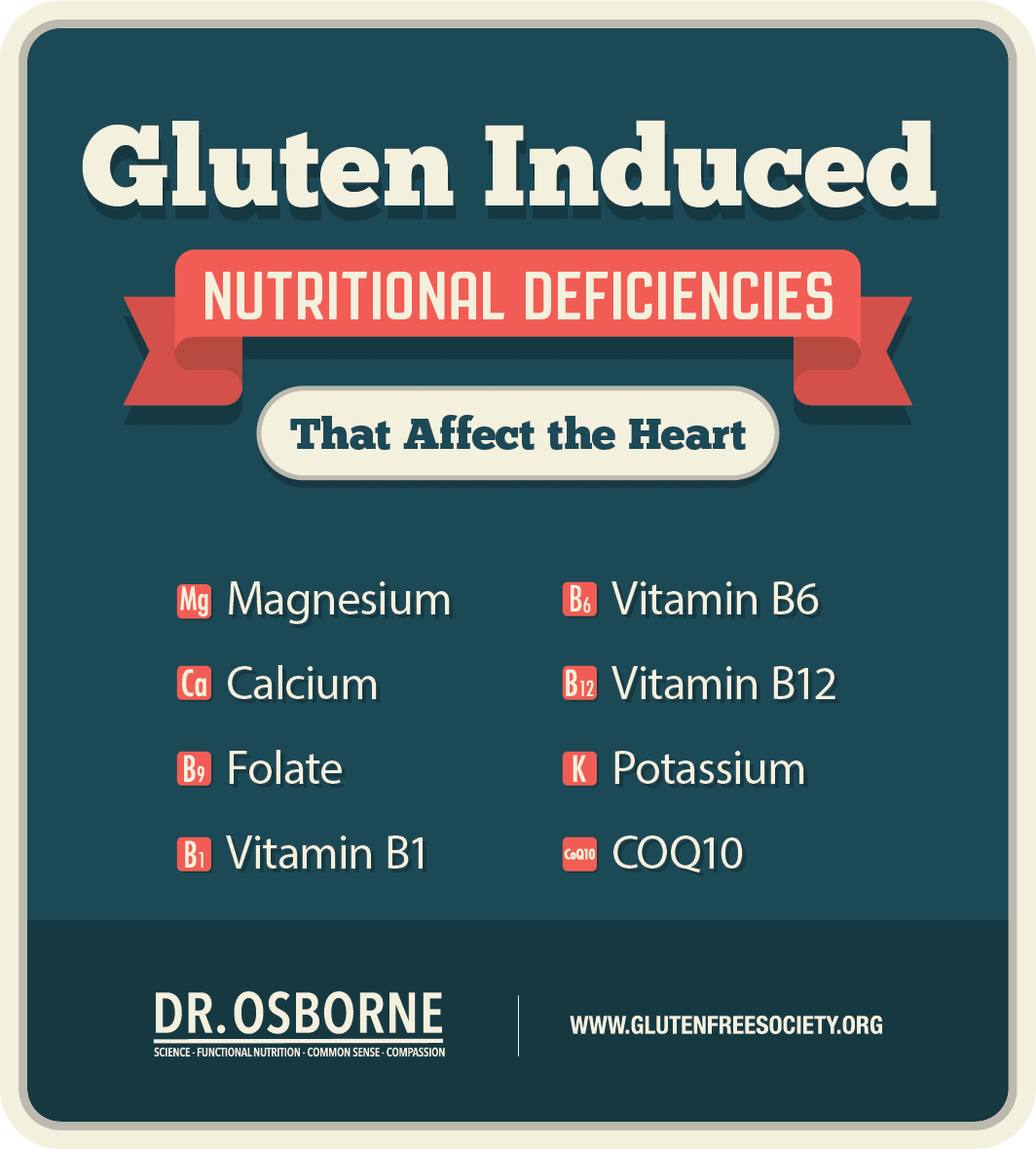 For example, studies have shown that those with celiac disease are often low in vitamin B12, folate, vitamin D, iron, zinc, selenium, magnesium, and calcium.
This is problematic because chronic nutrient deficiencies can cause physical stress and inflammation, which often leads to disease.
For example, zinc and selenium act as powerful antioxidants that prevent the build-up of free radicals. So without an adequate supply of these nutrients, the high concentration of free radicals can lead to cellular damage. And cellular damage causes inflammation.
Mounting evidence suggests that vitamin D deficiency is associated with an increased risk of heart disease and its risk factors, including type 2 diabetes and high blood pressure. For example, in a study of 230 heart attack patients admitted to a hospital, 96% of them had abnormally low vitamin D levels.
Studies have also associated higher magnesium intake with reducing cardiovascular disease risk factors, including lowering blood pressure, fighting inflammation, improving lipids (i.e., cholesterol and triglycerides), and balancing blood sugar and insulin.
For example, high blood pressure plays a big role in the initial damage to the lining of blood vessels that I mentioned earlier. And a collection of studies found that supplemental magnesium significantly lowered both systolic and diastolic blood pressure when compared to a control group. The systolic blood pressure dropped an average of 4.18 mm Hg and the diastolic blood pressure dropped an average of 2.27 mm Hg.
The above is relevant because a study evaluating the effectiveness of blood pressure-lowering medications concluded that a 0.8 – 2 mm Hg change in systolic blood pressure significantly reduced the risk of heart disease. And a 2 – 3 mm Hg change in diastolic blood pressure reduced the risk of stroke by 6 – 12%.
Further, vitamin B12 and folate deficiencies have been linked with an increased risk of stroke. And folate deficiency has also been associated with abnormal blood clotting and complications.
For example, studies have shown that those with celiac disease are often low in vitamin B12, folate, vitamin D, iron, zinc, selenium, magnesium, and calcium.
This is problematic because chronic nutrient deficiencies can cause physical stress and inflammation, which often leads to disease.
For example, zinc and selenium act as powerful antioxidants that prevent the build-up of free radicals. So without an adequate supply of these nutrients, the high concentration of free radicals can lead to cellular damage. And cellular damage causes inflammation.
Mounting evidence suggests that vitamin D deficiency is associated with an increased risk of heart disease and its risk factors, including type 2 diabetes and high blood pressure. For example, in a study of 230 heart attack patients admitted to a hospital, 96% of them had abnormally low vitamin D levels.
Studies have also associated higher magnesium intake with reducing cardiovascular disease risk factors, including lowering blood pressure, fighting inflammation, improving lipids (i.e., cholesterol and triglycerides), and balancing blood sugar and insulin.
For example, high blood pressure plays a big role in the initial damage to the lining of blood vessels that I mentioned earlier. And a collection of studies found that supplemental magnesium significantly lowered both systolic and diastolic blood pressure when compared to a control group. The systolic blood pressure dropped an average of 4.18 mm Hg and the diastolic blood pressure dropped an average of 2.27 mm Hg.
The above is relevant because a study evaluating the effectiveness of blood pressure-lowering medications concluded that a 0.8 – 2 mm Hg change in systolic blood pressure significantly reduced the risk of heart disease. And a 2 – 3 mm Hg change in diastolic blood pressure reduced the risk of stroke by 6 – 12%.
Further, vitamin B12 and folate deficiencies have been linked with an increased risk of stroke. And folate deficiency has also been associated with abnormal blood clotting and complications.
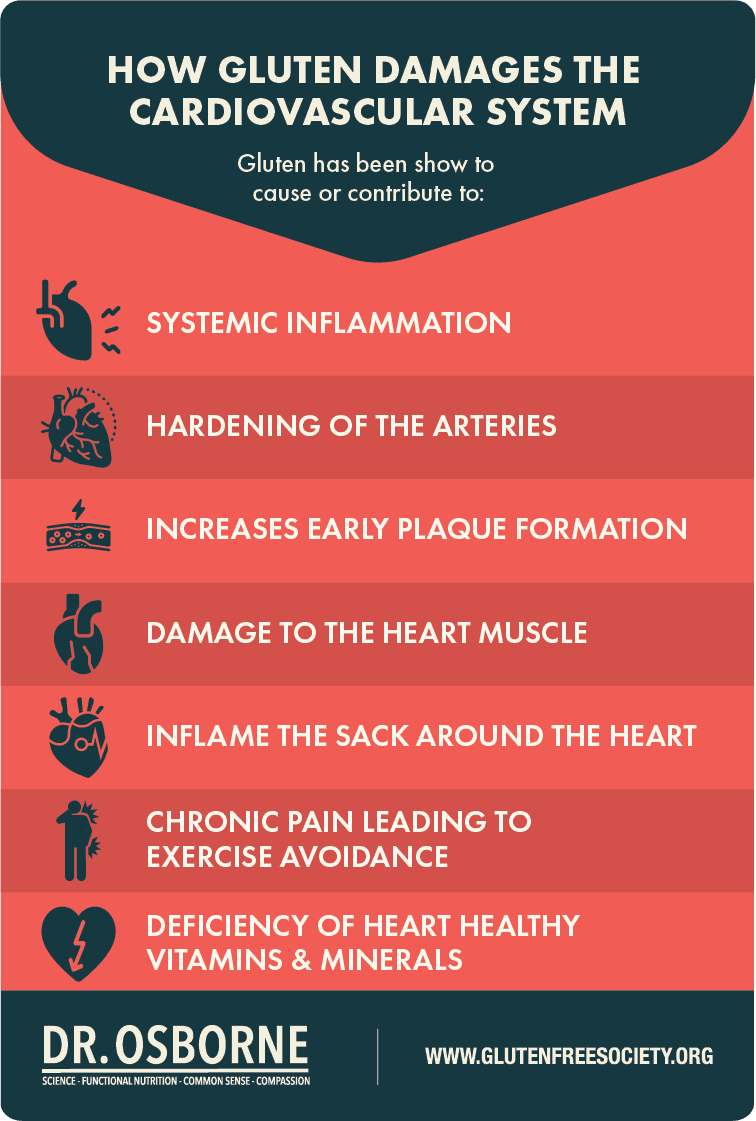
 Processed foods also contain food additives, such as emulsifiers, preservatives, and thickeners. And science is beginning to find that these food additives alone may promote inflammation, insulin resistance, and obesity.
It’s also worth noting that many food additives are derived from gluten-containing grains. For example, malt extract is made from barley. Corn is used to make maltodextrin, high fructose corn syrup, and monosodium glutamate (MSG) among many others. Even xanthan gum, a common ingredient in “gluten-free” foods, may be derived from corn and wheat.
Finally, processed foods are packed with refined table salt, stripped of health-promoting trace minerals. So a diet rich in ultra-processed foods may elevate one’s blood pressure.
As you can see, processed foods are associated with many heart disease risk factors. Thus, it’s not surprising that science has also found a link between eating them and an increased prevalence of heart disease.
Here is another article that outlines ingredients to avoid on a TRUE gluten free diet – https://www.glutenfreesociety.org/guidelines-for-avoiding-gluten-unsafe-ingredients-for-gluten-sensitivity/
Processed foods also contain food additives, such as emulsifiers, preservatives, and thickeners. And science is beginning to find that these food additives alone may promote inflammation, insulin resistance, and obesity.
It’s also worth noting that many food additives are derived from gluten-containing grains. For example, malt extract is made from barley. Corn is used to make maltodextrin, high fructose corn syrup, and monosodium glutamate (MSG) among many others. Even xanthan gum, a common ingredient in “gluten-free” foods, may be derived from corn and wheat.
Finally, processed foods are packed with refined table salt, stripped of health-promoting trace minerals. So a diet rich in ultra-processed foods may elevate one’s blood pressure.
As you can see, processed foods are associated with many heart disease risk factors. Thus, it’s not surprising that science has also found a link between eating them and an increased prevalence of heart disease.
Here is another article that outlines ingredients to avoid on a TRUE gluten free diet – https://www.glutenfreesociety.org/guidelines-for-avoiding-gluten-unsafe-ingredients-for-gluten-sensitivity/
Stay up-to-date with the latest articles, tips, recipes and more.

*These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure or prevent any disease.
If you are pregnant, nursing, taking medication, or have a medical condition, consult your physician before using this product.
The entire contents of this website are based upon the opinions of Peter Osborne, unless otherwise noted. Individual articles are based upon the opinions of the respective author, who retains copyright as marked. The information on this website is not intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice. It is intended as a sharing of knowledge and information from the research and experience of Peter Osborne and his community. Peter Osborne encourages you to make your own health care decisions based upon your research and in partnership with a qualified health care professional.
5 Responses
I get overwhelmed at all of the possible nutritional deficiencies that I might have. I know I don’t get everything in my diet all the time.
Try the app called: Cronometer.
I started using it last year in July. I’ve lost 21 lbs, and lowering my Chloresterol and Blood sugar. I found I was not getting all my vitamins and minerals, just from using the app. It’s amazing! I feel so much better now!
Does hernia affect size of heatt
Italy is known for having much better and healthier wheat. They don’t have the many problems with it that we have in the US. Would these missing nutritional deficiencies still be considered there?
Why does my blood pressure go up when I am lying down and how do I cure it, thank you !