Contents
ToggleWhat Causes Fibromyalgia? More Studies Point To Gluten
If you’ve been following my research for any length of time, you know that I am passionate about sharing research that shares links between celiac disease or gluten consumption and a wide range of health conditions. Many don’t realize that gluten and celiac disease can be associated with a number of other diseases, so I feel compelled to share these links in an attempt to help you understand and advocate for your own health and to feel empowered with information that can help you make impactful and lasting changes to your diet, lifestyle, and quality of life. Today, we are discussing what causes fibromyalgia. And we are focusing specifically on the link between gluten sensitivity and fibromyalgia. But because fibromyalgia is so often misunderstood, let’s start with a bit of background.
What is fibromyalgia?
Fibromyalgia is a condition generally associated with severe and debilitating muscle, tendon, and soft tissue pain. It is also referred to as:
- Myalgia
- Myofascitis
- Fibromyositis
- Fibrositis
What are common fibromyalgia symptoms?
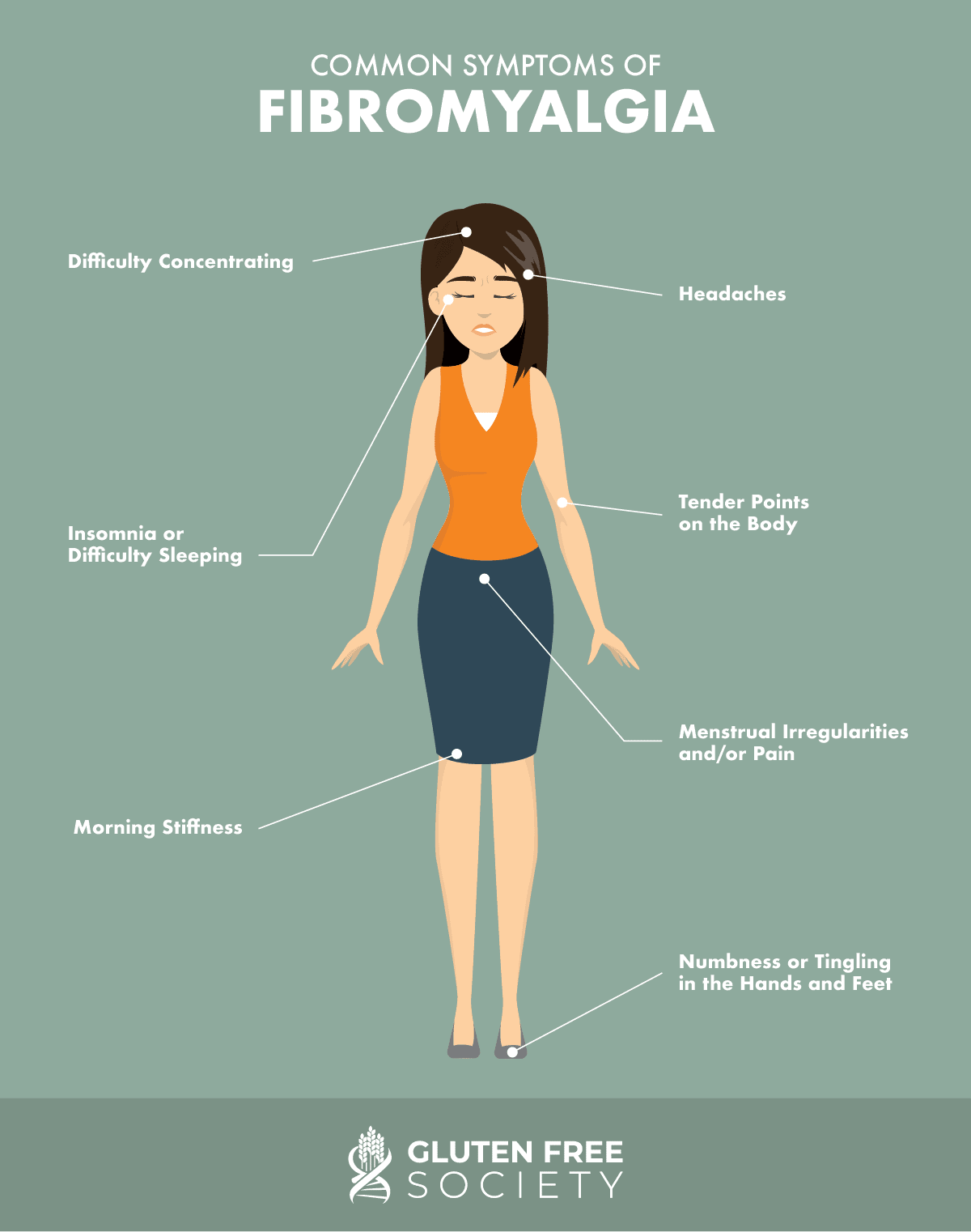
Fibromyalgia causes severe pain in the body. More specifically, some common symptoms experienced by people with fibromyalgia include:
- Tender points pressure points on their body;
- Insomnia or difficulty sleeping;
- Morning stiffness;
- Headaches;
- Numbness or tingling in the hands and feet;
- Menstrual irregularities and/or pain; and
- Difficulty concentrating/brain fog.
How is Fibromyalgia Diagnosed?
There is no lab test or definitive way to diagnose fibromyalgia. Rather, a fibromyalgia diagnosis is typically a diagnosis of exclusion – patients are generally diagnosed by testing first for other diseases that have similar symptoms and excluding those. These often include rheumatoid arthritis, major depressive disorder, multiple sclerosis, and other painful autoimmune diseases. If tests for these other conditions come back negative, it is often assumed that what remains must be fibromyalgia.
But while many patients get the diagnosis of fibromyalgia after reporting chronic pain symptoms, it’s sadly often a misdiagnosis. This is because fibromyalgia is often misunderstood. It is often treated with anti-inflammatory medications or supplements but they aren’t effective, because fibromyalgia is actually a disease that starts in the central nervous system. This leaves many fibromyalgia patients with persistent pain despite efforts to mitigate the pain with medicinal anti-inflammatories. It also leaves people who have other inflammatory conditions with a misdiagnosis and more confusion than answers.
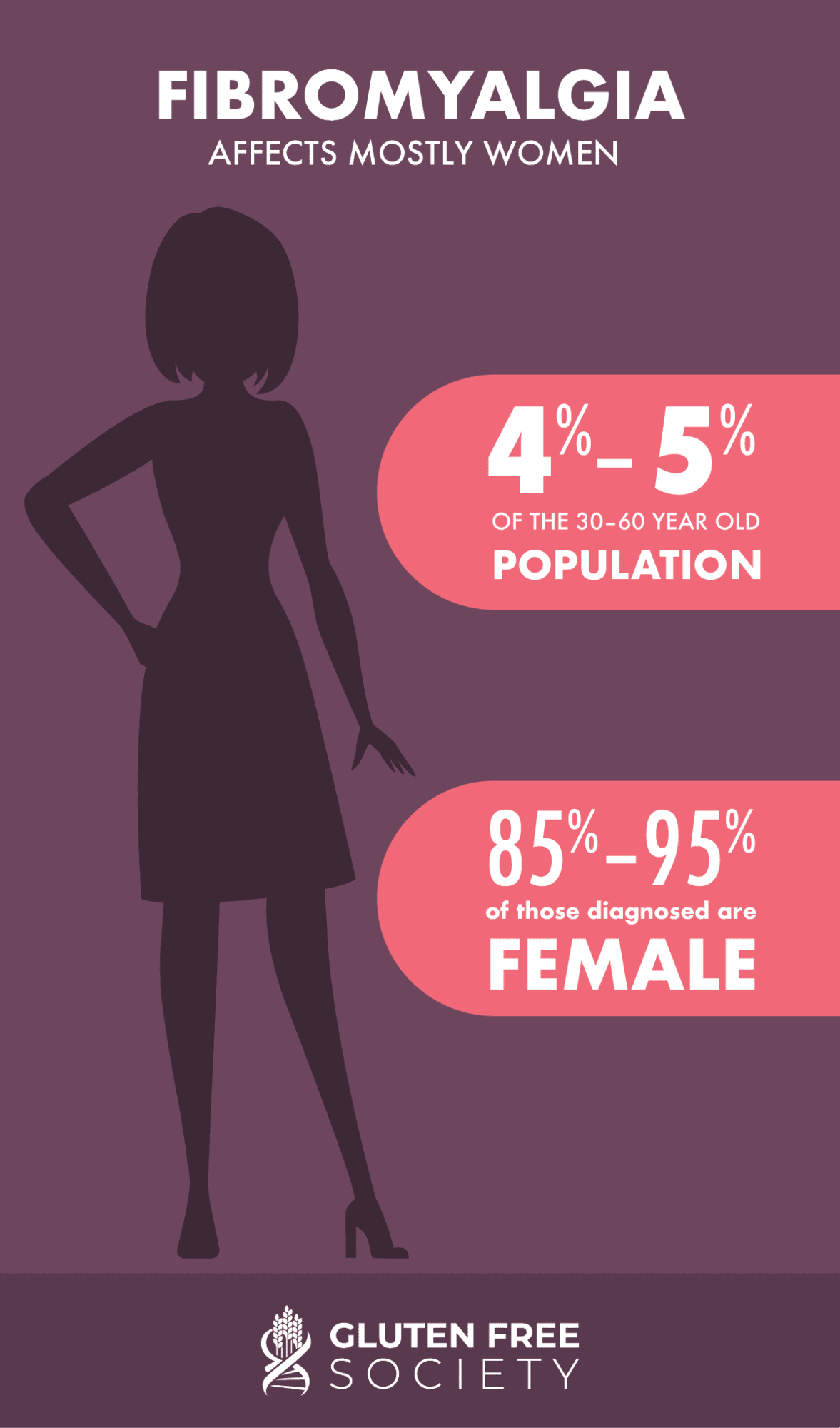
Fibromyalgia affects four to five percent of the 30–60-year-old population. It is largely a disease that affects females, as 85–95 percent of those diagnosed are female.
What causes fibromyalgia?
While the exact causes of fibromyalgia are unknown, there are a number of factors that are thought to contribute to the development of the condition. When answering the question – what causes fibromyalgia, we have to consider the following:
- Abnormal pain messages: The central nervous system is responsible for sending messages throughout the body. It is believed that people with fibromyalgia may process pain messages differently which could result in the feelings of and sensitivity to pain. It is unclear why, but could be the result of changes to chemicals in the nervous system.
- Chemical imbalances: Research has discovered that people with fibromyalgia have unusually low levels of certain hormones in their brain. Low levels of these hormones (serotonin, noradrenaline, and dopamine) can disrupt things like mood, appetite, sleep, and your stress response.
- Sleep issues: Sleep concerns are tricky when it comes to fibromyalgia, because they may be both a symptom and a cause. It may be difficult to distinguish which came first, but some theories suggest that poor sleep may exacerbate pain and other complications of fibromyalgia.
- Genetics: Some research has pointed to genetics as playing a role in the development of fibromyalgia. This means that you may be predisposed to develop the condition and more likely to develop fibromyalgia after a triggering event. This theory follows the adage, “genes load the gun, environment pulls the trigger.”
- Stressful events: Both physical and emotional stress are thought to be possible triggers for fibromyalgia. Events like an injury, a virus, giving birth, having surgery, or experiencing a troubled relationship or death of a loved one trigger a stress response in the body and may contribute to the onset of fibromyalgia.
How are gluten and fibromyalgia related?
While many don’t associate fibromyalgia with gastrointestinal concerns, in fact several studies indicate that patients with fibromyalgia have abdominal symptoms. While the significance of this association is generally not well acknowledged, some report a prevalence of irritable bowel syndrome (IBS) in up to 81% of fibromyalgia patients.
Does gluten cause fibromyalgia?
Some research has suggested that gluten ingestion can contribute to fibromyalgia. Studies have shown that gluten ingestion can exacerbate symptoms of fibromyalgia. Additional studies have shown that the avoidance of gluten can significantly improve fibromyalgia symptoms.
A gluten free diet CAN help fibromyalgia symptoms
In fact, one small study assessed the effectiveness of a gluten-free diet in seven adult female screening-detected celiac disease subjects, categorized as severe IBS and fibromyalgia patients. At the start of the study, all patients had poor Quality of Life and VAS (pain scale) scores, a high number of tender points and drug prescriptions, and increased Tissue Transglutaminase (tTG) levels (a blood marker for celiac disease). After one year on a gluten-free diet, all of these measures significantly improved in all patients. The number of prescriptions relied upon significantly decreased and tTG returned to normal levels in all subjects.
Results of this study show that the adherence to a gluten-free diet by fibromyalgia patients can simultaneously improve celiac disease and fibromyalgia symptoms. It’s important to note that the study was small, but it is promising that when a gluten free diet was implemented, symptoms of celiac disease, IBS, and fibromyalgia were all decreased substantially. It suggests that fibromyalgia sufferers may actually have underlying or undiagnosed gluten sensitivity, and both conditions may be addressed by following a gluten-free diet.
Another small study followed 20 patients, this time confirmed without celiac disease but with a fibromyalgia diagnosis. All patients were put on a gluten free diet for an average of 16 months. The level of widespread chronic pain improved dramatically for all patients. For 15 patients, chronic widespread pain was no longer present at all, indicating remission of fibromyalgia. These 15 patients returned to work or normal life. In three patients who had been previously treated in pain units with opioids, their drugs were discontinued. Fatigue, gastrointestinal symptoms, migraine, and depression reported by several patients also improved together with pain. Again, this is a small study with wildly promising results that even in patients without celiac disease, a gluten-free diet can help to resolve fibromyalgia symptoms.
How nutrient deficiencies can play a role
Several observational studies have evaluated the nutritional status of patients with chronic musculoskeletal pain like that in fibromyalgia by comparing their dietary patterns with the dietary patterns of healthy, pain-free people or with nutritional reference values. A systematic review of 12 research papers found that those experiencing chronic pain were consistently low in many of the same nutritional deficiencies that are commonly found in celiac disease patients:
- Magnesium – Magnesium inhibits certain nerve receptors, such as N-methyl-D-aspartate, which may be a cause of fibromyalgia pain. Low levels of magnesium are associated with low-grade chronic systemic inflammation and chronic sleep deprivation, a common complaint in fibromyalgia patients.
- B Vitamins – B-complex vitamins act as coenzymes in energy metabolism and low levels have been identified in fibromyalgia patients. It’s not surprising, as low energy and fatigue are common symptoms of the disease.
- CoQ10 – CoQ10 increases cellular ATP (energy) production. Therefore, research has suggested their supplementation could help improve fatigue and other symptoms that are common in fibromyalgia.
- Vitamin D – A meta-analysis revealed credible evidence that vitamin D can be a determinant factor for fibromyalgia. Almost all of the studies reviewed found lower levels of vitamin D among fibromyalgia patients than the control groups.
- Zinc – Zinc deficiency may contribute to the dysfunction of natural killer cells and cell-mediated immune function which can play a role in the symptoms of fibromyalgia.
- Selenium – Selenium deficiency has been related to skeletal muscle disorders, due to an amplified prostaglandin synthesis and many times has been found to be lower in patients with fibromyalgia than control groups.
An undeniable relationship
The relationship between gluten and fibromyalgia is still being explored, but the available research is clear that a gluten-free diet holds promise for relief of the wide range of fibromyalgia symptoms.
Want to know more about this? Watch Dr. Osborne’s replay link in the video below!








One Response
Those who suffer from Fibromyalgia as I do should benefit from benefits assistance even though that is mild… hence whatever the circumstances is both married and single should benefit.