TL;DR
Yes, the research suggests gluten can be a contributing factor in some people, especially those with celiac disease and possibly other gluten-related disorders. The strongest mechanisms are chronic inflammation, endothelial dysfunction, arterial stiffness, elevated homocysteine, and malabsorption of key nutrients such as folate, vitamin B12, vitamin B6, vitamin D, magnesium, zinc, and iron. Several studies have found higher inflammatory markers, higher homocysteine, and worse vascular function in people with celiac disease, while a recent meta-analysis found that a gluten-free diet was associated with a modest reduction in systolic blood pressure and C-reactive protein.
Contents
ToggleDoes Gluten Cause High Blood Pressure?
High blood pressure is typically presented as a simple salt-and-stress problem, but that is an oversimplification. Blood pressure is heavily influenced by the health of your blood vessels, the degree of inflammation in your body, the integrity of your gut, and whether you are absorbing the nutrients needed to maintain normal vascular tone.
In some people, gluten can be part of that story. The evidence is strongest in celiac disease, where gluten triggers an autoimmune inflammatory response that damages the small intestine and can spill over into the vascular system.
That does not mean gluten is the cause of hypertension in every person. It means gluten-related disease may be an overlooked driver in a meaningful subset of people, especially those with gluten induced malabsorption, nutrient deficiencies, autoimmune problems, or inflammatory symptoms.
What the research actually shows
Human studies have reported increased arterial stiffness, higher C-reactive protein, higher erythrocyte sedimentation rate, higher homocysteine, and vascular impairment in people with celiac disease, even when conventional cardiovascular risk factors are not especially elevated.
A 2024 systematic review and meta-analysis also found that a gluten-free diet was associated with reductions in systolic blood pressure and C-reactive protein, suggesting that in at least some gluten-affected populations, removing gluten may improve vascular risk markers.
A case study published in the Journal of Human Hypertension followed a 49 year old woman with celiac disease whose high blood pressure normalized on the gluten free diet.
A study published in the Journal of Hypertension found that a 90 day gluten free diet led to substantial reductions in systolic and diastolic blood pressure.
Although researchers have made multiple connections between gluten and hypertension, there is not enough evidence to make the blanket statement that gluten raises blood pressure in everyone. A 2022 Cochrane review concluded that, in the general population, evidence is still very limited and it remains unclear whether gluten intake meaningfully changes blood pressure.
The short answer
So, can gluten cause high blood pressure? The most accurate answer is yes – gluten may contribute to high blood pressure indirectly by driving inflammation, endothelial dysfunction, hyperhomocysteinemia, and nutrient malabsorption.
How Gluten May Raise Blood Pressure
Inflammation can damage the blood vessels
Celiac disease is not just a gut issue. It is an immune-mediated inflammatory disease triggered by gluten in genetically susceptible people. Reviews of the literature have linked celiac disease to cardiovascular involvement and have specifically highlighted autoimmunity and inflammation as central mechanisms. That matters because inflammation can reduce nitric oxide availability, impair endothelial function, and increase arterial stiffness, all of which make it harder for blood vessels to relax normally. When vessels lose flexibility and become inflamed, blood pressure can rise.
Why the endothelium matters
The endothelium is the thin inner lining of your blood vessels. It helps regulate dilation, blood flow, clotting, and vascular tone. When the endothelium is injured by inflammation or oxidative stress, blood vessels become less responsive and more rigid. Reviews on homocysteine and hypertension describe endothelial dysfunction as an important mechanism in the development of elevated blood pressure, and celiac-related inflammation has been tied to this same vascular problem.
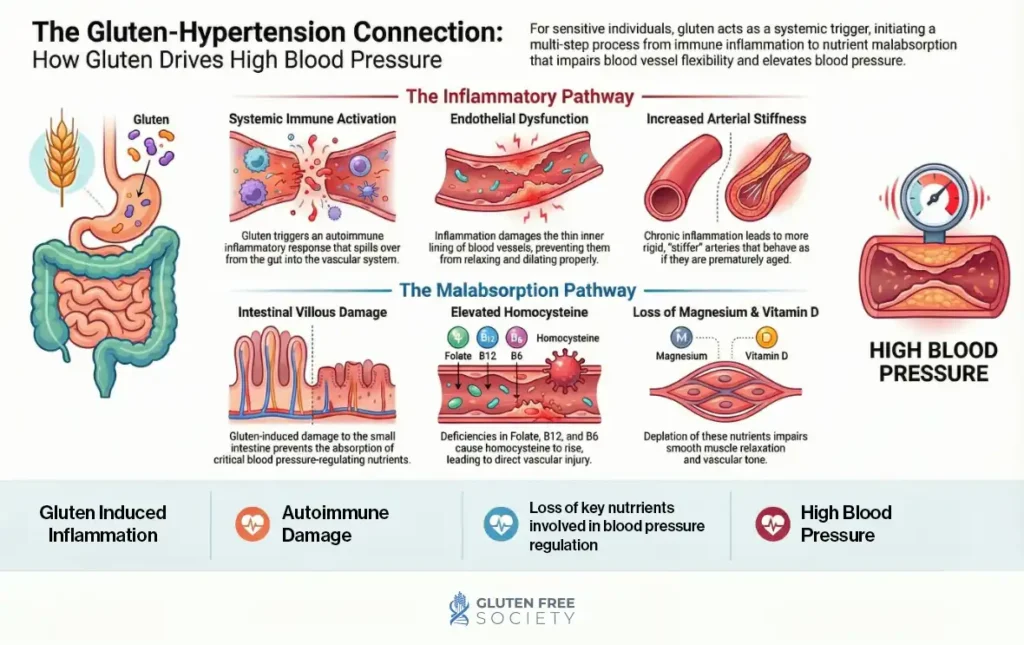
Celiac disease has been linked to arterial stiffness and vascular impairment
In one study, adults with celiac disease had higher pulse wave velocity, higher inflammatory markers, higher homocysteine, and more evidence of arterial stiffness than healthy controls.
Another study found that adults with celiac disease appeared to be at increased risk of early atherosclerosis, likely driven in part by chronic inflammation, and that these vascular abnormalities improved when gluten was removed and the intestinal lining normalized.
In plain English, the vessels in untreated or poorly controlled celiac disease may behave as if they are older, stiffer, and more inflamed than they should be.
Homocysteine may be one of the missing links
Homocysteine is an amino acid byproduct that should be recycled efficiently with the help of folate, vitamin B12, and vitamin B6. When those nutrients are low, homocysteine can rise. That matters because elevated homocysteine has been linked to endothelial dysfunction, vascular injury, and hypertension.
A meta-analysis using Mendelian randomization found evidence supporting a causal link between higher homocysteine levels and hypertension risk, and classic vascular reviews describe hyperhomocysteinemia as a contributor to impaired blood vessel relaxation and increased arterial pressure.
Why this matters in gluten-related disease
In patients with gluten sensitivity and celiac disease, damage to the small intestine can impair absorption of the very nutrients needed to keep homocysteine in check. A well-known case report described a patient with reversible hypertension in the setting of celiac disease, elevated homocysteine, and impaired endothelial function. After a gluten-free diet plus repletion of folate, B6, B12, and iron, the patient’s blood pressure improved and later normalized. A case report is not the same as a randomized trial, but it provides a biologically plausible clinical example of how gluten-related malabsorption could feed into hypertension through homocysteine and vascular dysfunction.
Malabsorption and Nutrient Deficiencies Can Push Blood Pressure in the Wrong Direction
Gluten damage to the gut can reduce absorption of key nutrients
Untreated celiac disease commonly causes deficiency of iron, folate, vitamin B12, vitamin D, zinc, and magnesium, largely because villous damage and brush border injury reduce normal absorption. That is not a fringe observation. It is well described in the medical literature.
Folate, B12, and B6 matter because they regulate homocysteine
When folate, B12, and B6 are low, homocysteine tends to rise. That is relevant to blood pressure because homocysteine is associated with endothelial dysfunction and hypertension. Long-term follow-up data in adults with celiac disease have shown that even people carefully following a gluten-free diet can still have poor vitamin status, which may carry cardiovascular implications through elevated homocysteine.
Magnesium and vitamin D matter because they support vascular function
Magnesium helps regulate vascular tone, smooth muscle relaxation, insulin signaling, and nervous system balance. Vitamin D is also tied to immune regulation and cardiovascular health. Reviews on celiac disease note that magnesium and vitamin D deficiency are common, especially before full intestinal recovery. That means one person may have multiple overlapping hits: immune activation from gluten, damaged intestinal absorption, and lower levels of nutrients needed to maintain normal vessel function.
A gluten-free diet can help, but it is not automatically nutritionally perfect
Here is an important nuance. Going gluten free is necessary for celiac disease, but a gluten-free diet is not automatically nutrient-dense. Reviews have found that gluten-free diets can still be low in B vitamins, iron, calcium, vitamin D, zinc, magnesium, and fiber, particularly when people rely on ultra-processed gluten-free products. So the answer is not just “remove gluten.” The answer is “remove the trigger and rebuild nutritional status.”
Can a Gluten Free Diet Lower Blood Pressure in Non Celiacs?
The strongest human evidence connecting gluten-related disease to blood pressure comes from patients with gluten sensitivity and celiac disease, however; a study of 200 men with uncontrolled high blood pressure found significant reductions in both systolic and diastolic blood pressure when following a gluten free diet.
The following chart summarizes these findings:
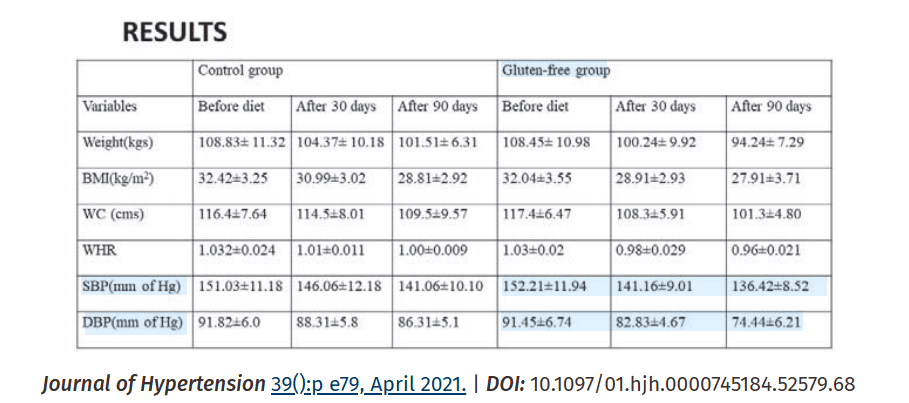
Experimental Research Also Supports a Vascular Effect
A 2024 animal study reported that mice with celiac-like disease induced by gluten exposure showed increased blood pressure and impaired vascular relaxation, along with inflammatory and oxidative stress changes. Animal data do not prove the same effect in humans, but they strengthen the biological plausibility that gluten-triggered immune disease can affect vascular function outside the gut.
Who Should Consider Gluten as a Hidden Blood Pressure Trigger?
You should think about gluten if high blood pressure occurs alongside any of the following
Digestive Symptoms
Chronic bloating, diarrhea, constipation, reflux, abdominal pain, gas, or unexplained weight loss can point to celiac disease or another gut issue affecting absorption. Celiac disease is primarily an intestinal immune-mediated disorder, even though it often has systemic effects.
Nutrient Deficiencies
Iron deficiency, low folate, low B12, low vitamin D, low zinc, or low magnesium should raise suspicion, especially when several show up together or keep recurring. Those deficiencies are commonly described in celiac disease.
Autoimmune Disease or Chronic Inflammation
Celiac disease is autoimmune by nature, and reviews have linked it to broader cardiovascular and inflammatory consequences. If you already have autoimmune disease, unexplained vascular symptoms, or persistent inflammation, gluten should at least be on the differential.
Elevated C-Reactive Protein or Homocysteine
If your homocysteine is high and you also have digestive symptoms, anemia, or other signs of malabsorption, it is worth asking whether gluten-related intestinal damage is part of the reason.
Clinical Perspective From Dr. Osborne
In my clinical experience, numerous patients have achieved significant blood pressure reductions by adhering to the No Grain No Pain diet. This nutritional approach helps decrease chronic inflammation, which in turn facilitates weight loss, enhances mobility, and optimizes nutrient absorption. These collective improvements create a powerful, synergistic effect on overall health.
However, it is important to recognize that a gluten-free lifestyle is not a guaranteed fix for everyone, as hypertension is a multifaceted condition. Because there is no single solution for every scenario, removing gluten may not lower blood pressure in all cases.
The following chart illustrates who may be the best candidate to consider diet change in relationship to high blood pressure:
| Scenario | How gluten may affect BP | Strength of evidence | Typical clues |
| Celiac disease | Inflammation, malabsorption, autoimmune stress | Moderate | GI issues, anemia, nutrient deficiency |
| Non-celiac gluten sensitivity | Immune/inflammatory reaction | Emerging | Symptoms after gluten without classic celiac labs |
| Processed gluten-heavy diet | Weight gain, insulin issues, sodium load | Stronger for diet pattern than gluten itself | BP rises with ultra-processed meals |
What To Do If You Suspect Gluten Is Affecting Your Blood Pressure
Step 1: Do not stop your blood pressure care
Do not use this article as a reason to stop medications or ignore hypertension. High blood pressure can damage the brain, kidneys, heart, and eyes over time. Gluten may be part of the problem for some people, but it is rarely the only variable.
Step 2: Get evaluated for celiac disease before removing gluten
If celiac disease is on the table, testing is usually more accurate before you eliminate gluten. Once gluten is removed, antibodies and biopsy findings may normalize and make diagnosis harder. The evidence linking gluten-related disease to blood pressure is strongest in diagnosed celiac disease, so proper testing matters.
Step 3: Check the terrain
A more complete workup may include nutrient testing, iron studies, folate, B12, vitamin D, magnesium assessment, inflammatory markers, and homocysteine. That is especially reasonable if blood pressure issues are accompanied by fatigue, anemia, neuropathy, brain fog, digestive symptoms, or autoimmune problems. The literature supports a strong overlap between celiac disease, nutrient depletion, and homocysteine-related vascular risk.
Step 4: If gluten is a trigger, remove it completely and rebuild nutrition
For people with celiac disease, the treatment is lifelong strict gluten elimination. Studies suggest that gluten abstinence with mucosal healing can improve vascular abnormalities, and meta-analytic data suggest a modest improvement in systolic blood pressure and C-reactive protein on a gluten-free diet. But the diet must be done well, not just replaced with processed gluten-free junk food.
The Bottom Line
Gluten does not appear to be a universal cause of hypertension in the general population. But in people with celiac disease, and possibly in a broader subgroup with gluten-related inflammatory disease, gluten can contribute to high blood pressure through a multi-step process: immune activation, inflammation, endothelial dysfunction, arterial stiffness, hyperhomocysteinemia, and malabsorption of key nutrients.
If you have high blood pressure plus digestive symptoms, nutrient deficiencies, autoimmunity, or elevated homocysteine, gluten deserves a closer look. The real question is not whether gluten raises blood pressure in everyone. The real question is whether your body is reacting to gluten in a way that is damaging your gut and your blood vessels at the same time.
FAQ
Can gluten cause high blood pressure?
Yes, possibly. The best evidence suggests gluten may contribute to high blood pressure indirectly in susceptible people, especially those with celiac disease, through inflammation, endothelial dysfunction, homocysteine elevation, and nutrient malabsorption. Evidence in the general population is still limited and inconsistent.
Can celiac disease raise blood pressure?
Yes, it may in some patients. Human studies have linked celiac disease to increased arterial stiffness, inflammatory markers, vascular impairment, and elevated homocysteine, all of which can push blood pressure in the wrong direction.
Can a gluten-free diet lower blood pressure?
Possibly. Human studies have shown that gluten free diets can lower blood pressure.
What is the connection between gluten and homocysteine?
The connection is usually indirect. In celiac disease, gluten damages the small intestine, which can reduce absorption of folate, vitamin B12, and vitamin B6. Those nutrients are needed to recycle homocysteine. When they are low, homocysteine may rise, and elevated homocysteine has been linked to endothelial dysfunction and hypertension.
What nutrient deficiencies from gluten damage may affect blood pressure?
The major ones discussed in the celiac literature include folate, vitamin B12, vitamin B6, vitamin D, and magnesium. These nutrients influence homocysteine metabolism, immune balance, vascular tone, and overall cardiovascular function.
Is the problem gluten itself or processed gluten foods?
For celiac disease, the immune-triggering problem is gluten itself. In the wider population, blood pressure may also be worsened by ultra-processed dietary patterns, excess sodium, poor nutrient density, and refined carbohydrate load. So in some people, both factors may be in play: gluten as an immune trigger and processed food as a metabolic trigger. Evidence tying blood pressure directly to gluten in the general population remains limited.
Should everyone with high blood pressure go gluten free?
Not necessarily. Beyond gluten, there are many factors that contribute to hypertension. But people with high blood pressure plus digestive symptoms, nutrient deficiencies, autoimmune disease, elevated homocysteine, or a family history of celiac disease may warrant screening for gluten-related disease.





