No Grain No Pain – Bringing an End to Autoimmunity
>>Pick up your copy of No Grain No Pain Here<<
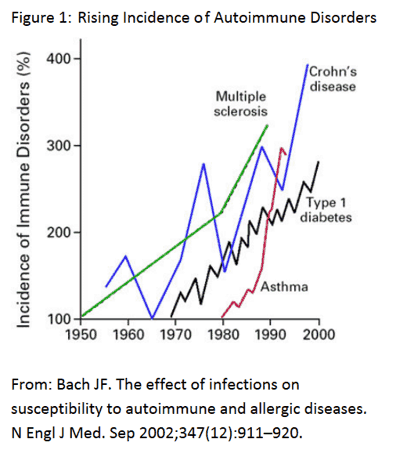
The Rise of Autoimmune Disease – Is an increase of dietary gluten the cause?
Autoimmune disease occurs when a persons immune system mounts an attack against their own tissues. An estimated 50 million Americans are suffering with autoimmune disease (AID), and the numbers are climbing. To give you perspective on this health crisis – 1 out of every 7 people you meet have an AID. Autoimmune disease trumps both cancer (9 million) and heart disease (22 million). Autoimmune disease is the #1 cause of death in women under the age of 65. Science has recognized more than 100 forms of autoimmune disease. In Western countries, autoimmune disease has been increasing at an alarming rate(1).
This modern day plague can affect any organ in the body. You might recognize some of these more common forms of autoimmunity by name:
 Rheumatoid Arthritis – causes inflammation of the joints leading to swelling, pain, stiffness, weakness, and ultimately crippling pain and dysfunction.
Rheumatoid Arthritis – causes inflammation of the joints leading to swelling, pain, stiffness, weakness, and ultimately crippling pain and dysfunction.- Type I Diabetes – The immune system attacks the cells in your pancreas responsible for producing insulin causing a rise in blood sugar.
- Multiple Sclerosis – The immune system attacks the insulation around your nerves (myelin) leading to nerve pain, brain fog, loss of memory, muscle pain, muscle weakness, and can eventually cripple a person’s ability to walk.
- Psoriasis/Psoriatic Arthritis – Causes a chronic inflammation in the joints and on the skin.
- Asthma – Though rarely called an autoimmune process, asthma definitely has its roots in AI. It causes an inflammation in the airway that inhibits the flow of oxygen leading to trouble breathing, wheezing, exercise intolerance, and more.
- Hashimoto’s (hypothyroidism) – Damages the thyroid leading to reduced metabolic function, fatigue muscle pain, slow healing, and a host of other hormone based symptoms.
- Celiac Disease – Causes damage to the small intestines, and leads to malabsorption of vitamins and minerals. Can be fatal if left unrecognized.
- Crohn’s Disease – This disease causes inflammation on the right side of the large intestine. Typical symptoms include chronic diarrhea, blood in the stool, and physical wasting due to malnutrition.
- Ulcerative Colitis – An autoimmune disease that manifests as inflammation and ulceration of the left colon.
- Lupus (SLE) – An autoimmune condition that causes inflammation and rashes on the skin, a butterfly shaped rash on the face, as well as damage to the kidneys, heart, and brain.
There are many more types of autoimmune disease, and collectively these diseases all share the same origins. Doctors in today’s conventional medical system are focused on using medicine to suppress the symptoms of AID. These drugs include NSAIDS, steroids, and immune suppressing medications. Unfortunately these medicines do not address the underlying causes of autoimmunity. These medications can have serious complications and side effects to include an increase risk for gastric bleeding, ulcers, increased risk of infection, diabetes, and even cancer.
The good news is that we actually know that most of the triggers of autoimmune disease are diet and lifestyle related. Consider the following quote from researchers:
Indeed, over the last few decades significant changes in western dietary habits, environmental surroundings, and pollution exposure, infectious habitat and stress load, have led to a parallel rise in autoimmune diseases(1).
There are four well known, and scientifically established triggers for autoimmunity. Simply put, they are:
- Food
- Chemicals
- Microbial imbalances (bacteria, parasitic, fungal, viral)
- Nutritional deficiency
Excessive stress could also be considered a factor in the development of AID. Though stress by itself is rarely solely responsible for autoimmune illness. I have discussed all of these triggers in depth. You can learn more about them here.
The Connection Between Gluten & Autoimmune Disease
Gluten is a very well known and researched cause of celiac disease. Additionally, research has shown that a gluten free diet can actually help improve other forms of autoimmune disease. Studies have shown that a gluten free diet can improve outcomes for the following forms of AID(2,3,4,5,6,7):
Kidney disease: membrane proliferative glomerulonephritis, IgA nephropathy
Liver conditions: Autoimmune hepatitis (fatty liver disease)
Nerve & Brain (neurological) Disease: Peripheral neuropathy, Guillain-Barre syndrome, myasthenia gravis, myopathy (muscle pain), schizophrenia, cerebellar ataxia, vertigo, meniere’s disease, depression, ADD/ADHD, and autism.
Heart Disease: autoimmune myocarditis, dilated cardiomyopathy
Skin Disease: vitiligo, psoriasis, eczema, dermatitis herpetiformis, epidermolysis bullosa, pemphigus vulgaris, alopecia areata, linear IgA disease, cutaneous vasculitis, erythema nodosum and erythema elevatum diutinum dermatomyositis, and chronic urticaria (hives).
Hormonal Disease (endocrine): Addison’s, Hashimoto’s, Grave’s, Type I Diabetes
Blood Disorders: Hemolytic/aplastic anemia, leukopenia, thrombocytosis, anemia, pure red cell aplasia, thrombocytopenic purpura(TPP), IgM deficiency, IgA deficiency
Gastrointestinal Diseases: GERD, eosinophilic esophagitis, gastritis, IBS, Ulcerative Colitis, and Crohn’s disease.
Eye Disease: Uveitis
Rheumatological Diseases: Rheumatoid arthritis, Lupus, reactive arthritis, ankylosing spondylitis, psoriatic arthritis, polymyositis, polymyalgia rheumatica, undifferentiated connective tissue disease, fibromyalgia, and restless legs syndrome.
If you struggle with an AID, and have not tried going gluten free, you might be missing one of the most important pieces of the puzzle to solving your underlying inflammation and immune problem. As a matter of fact, I have personally seen thousands of cases of autoimmunity go into remission with diet change in my clinic, and this has been the genesis of a complex body of resources that I house on my website, Gluten Free Society.
It is my hope, that all medical professionals who commonly see and treat AID, will become educated on the potential possibility that gluten is a major trigger for all forms of autoimmunity, not just celiac disease…and in this recognition, make a gluten free diet a standard recommendation of care.
Medical References:
- Aaron Lerner, Patricia Jeremias, and Torsten Matthias, “The World Incidence andPrevalence of Autoimmune Diseases is Increasing.” International Journal of Celiac Disease, vol. 3, no. 4 (2015):151–155.
- Aaron Lerner, Ajay Ramesh & Torsten Matthias (2018) Going gluten free in non-celiac autoimmune diseases: the missing ingredient, Expert Review of Clinical Immunology, 14:11, 873-875.
- Lerner, Aaron & Ramesh, Ajay & Matthias, Torsten. (2017). Are Non-Celiac Autoimmune Diseases Responsive to Gluten-Free Diet?. International Journal of Celiac Disease. 5. 164-167. 10.12691/ijcd-5-4-6.
- Oliveira, F. Gluten and Neuroimmunology. Rare association with Myasthenia Gravis and Literature Review
Rev Assoc Med Bras (1992). 2018 Apr;64(4):311-314. - Badsha, H. Role of Diet in Influencing Rheumatoid Arthritis Disease Activity. Open Rheumatol J. 2018 Feb 8;12:19-28.
- Rodrigo, L, et al. Cutaneous and Mucosal Manifestations Associated with Celiac Disease. Nutrients. 2018 Jun 21;10(7).
- Limketkai, BN, et al. Prevalence and factors associated with gluten sensitivity in inflammatory bowel disease. Scand J Gastroenterol. 2018 Feb;53(2):147-151






3 Responses
(injected toxins are more dangerous than ingested toxins)
I have never understood, while our immune system is located in the gut, they are administrating all vaccines into the bloodstream directly and bypassing the immune system !!
I have stopped getting vaccines about 6 years ago. They made my blood sugars spike then drop, having type one diabetes. I also would have a seizure following them. Since I stopped I have not gotten any flu or major illness. I only once got a decent cold following a move during a winter storm.
So much of this makes sense to me. I was diagnosed with type one diabetes at the age of 14, celiac disease at 15(a blessed accident with diabetes blood work put in wrong testing…was actually suppose to be for A1c), then chronic Urticaria at 16, and finaly complex seizures at 17. Later the hives were seen to come from polyester. And I just had my second brain surgery and now reacting to lactose like I have an intolerance.