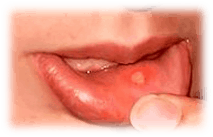
 A canker sore is a small painful ulcer in the lining of the mouth. It can also occur in the GI tract. Canker sores are pretty common and when they are found repeatedly only in the mouth, the condition is called Recurrent Aphthous Stomatitis (RAS). The condition is thought to resolve during the third decade of life.
A canker sore is a small painful ulcer in the lining of the mouth. It can also occur in the GI tract. Canker sores are pretty common and when they are found repeatedly only in the mouth, the condition is called Recurrent Aphthous Stomatitis (RAS). The condition is thought to resolve during the third decade of life.These canker sores can be associated with conditions that affect the GI tract, immune defects and syndromes that are inflammatory. They are not infectious or contagious in any way. However; up to 20% of patients with RAS are deficient in iron, vitamin B and folic acid. Another 3% have malabsorption or GI disorders. The detergent sodium lauryl sulphate found in toothpastes may aggravate them. And NSAIDs and other drugs can cause them.
They found 247 patients with RAS and screened them with the IgA anti-endomysial antibody (EMA) test along with serum IgA and IgA anti tissue transglutaminase. Seven patients with at least one positive test then had duodenal biopsies and all were found to have gluten sensitive enteropathy. This explained why these 7 patients were not successfully treated with the usual anti-canker sore medications (topical corticosteroids, tetracycline, colchicines). Over the next six months, 4 of the patients that went on a strict gluten free diet improved greatly.
Contents
ToggleSource:
BMC Gastroenterol 2009; 9: 44. Gluten sensitivity enteropathy in patients with recurrent aphthous stomatitis.
Gluten Free Society’s Stance:
It’s a little surprising that the researchers found that all 7 patients had a positive biopsy for gluten sensitivity enteropathy. Often this does not happen. A biopsy only selects a small amount of tissue, almost at random, and that tissue sample may not be reflective of what’s occurring in the intestinal tract. Everyone with gluten sensitivity won’t have a positive biopsy, and that could explain why the condition may not be identified.
The medical literature is full of research showing a strong relationship between gluten and many other diseases including osteoporosis, asthma, heart problems, arthritis, cancer, hypothyroidism, psychological disorders and fibromyalgia.
In the best of worlds, everyone with any of the diseases mentioned above is tested by the proper testing method. Identification of a problem is always the first step to solving it!





33 Responses
This is a good post, I stumbled across your post while looking for some random stuff. Thanks for sharing, I’ll be sure to come back.
Very interesting blog post thanks for sharing I just added your blog to my bookmarks and will be back 🙂 By the way this is a little off subject but I really like your web page layout.
This is really interesting, I used to suffer from ulcers very often prior to going on a gluten free diet but haven’t had one since…..hadn’t made the connection though!
Me, too! At it’s worst I had about 15 at once and could barely open my mouth. I’ve been GF for three years and no problems. My son is getting them, though, and I wonder if it’s not related to gluten.
Corn was a trigger for mine as a kid as well as gluten.
I must say that on the whole I am really happy with this site.After reading your post I can tell you are excited about your writing. If only I had your writing ability. I look forward to more updates and will be returning.Thanks!
This is great- I have a 10 year old who suffers with these “Ulcers”- He has high sensitivity to gluten but does not carry the gene.
I am diagnosed celiac and been off it for about 20 months.
I want him to see this article and decide for himself that his diet is making him react!
I have had canker sores all my life. I never knew they could be connected with gluten. That is extremely interesting.
I too have had canker sores most of my life; my daughter has psoriasis, and recently started a gluten-free lifestyle. Maybe there’s a connection; I’m going to try to change my eating habits and se what happens.
Is it cure now ? I m suffering since I born
Yes! Dermatitis herpetiformis is a symptom of gluten sensitivity/celiac!! Gets misdiagnosed as psoriasis or eczema often
all DH’s tests and biopsy were negative, but he has only had obe canker sore in 18 months of GF living.
My 8 yr old daughter was diagnosed Celiac just over a year ago. Since then, I have learned a lot (unfortunately, mostly the hard way)!!! Also, that her canker sores have dissappeared. Wish I’d seen this site a year ago:)
How long did it take for her sores to finally stop?
hi, i was wondering if you guys would know how to ask a doctor to do these special tests i still have cnkers and i know they get worse when my diet has more gluten, also toothpaste deff makes them worse and deff no morning coffee 🙂 some other good advice i know it to drink green food juices ,changes the ph in your body and they go away faster ,this is really really nice you posted this study i am going to pass along thanks 🙂
Jill,
Unfortunately, most doctors would look at you with a blank stare. You can have HLA-DQ genetic testing done via the following link:
https://stg-gfsociety-testing.kinsta.cloud/genetic-testing-for-gluten-sensitivity/
All the best,
Dr. Osborne
Jason coconut toothpaste work
And clove oil diluted helps relief them.
Im a 52 year old man who has been geting canker sores for the last year now sometimes 3 or more at a time all the time is there some way to find out what is causing them this is becomeing a nightmere I need help
Phillip,
Are you gluten free? If not, you might consider being tested and if necessary implementing the diet.
https://stg-gfsociety-testing.kinsta.cloud/genetic-testing-for-gluten-sensitivity/
My youngest daughter had a geographical tongue, which we were told was viral so nothing could be done. But she had pain and didn’t want to eat as foods ‘burned’. We went gluten free after the gene discovery. Her tongue has cleared up! She eats now! Now we’ve learned about corn and rice though through your site. Must explain about her occasional flare ups. Thanks for this info!! Your saving lives!
I am only 19 but I have suffered from chronic fatigue, joint pain, and dizzyness for as long as I remember so someone suggested that I try gluten-free. After just three weeks I was still skeptical that I was gluten-intolerant so when I went out of town I didn’t bother avoiding gluten. The very next day I woke up with several painful sores inside my mouth but I didn’t connect the two things until now!
I am the same. I have just got tested for crohns and ceoilaic. My doctor who did the procedure said it is ceoilaic but we will see. As when I have ulcers it is several not just one. I feel that I have one of these and when I do have the ulcers is when I am having a flare up not sure what it is yet.
I was diagnosed with Hashimoto two years ago, hypothyroid over ten years ago, but was only told to go Gluten Free about six months ago. Only after going Gluten free did I discover the acute and almost immediate joy of irritated lips and gums after ingesting gluten. Now, I’m not even sure what I have eaten that is causing them…because I’m pretty sure everything I have ingested in the last two days has been gluten free.
My question is: How could I not be getting mouth sores for all the years I was haphazardly ingesting gluten, but now that I have cut it out of my diet, I’m having such a strong and distinct reaction when I do ingest it, no matter how small? Is that normal?
Is there anything to the toothpaste or maybe lip balm I am using? Could those be causing me havoc?
Thank you!
Kameron,
Yes it is common to recognize more acute reactions to gluten after removing it. Very common.
and yes, check your toothpaste and lip balm as they can often contain gluten and grain based ingredients that are tricky to find. Here is a list of different names for gluten you can use to cross reference:
https://stg-gfsociety-testing.kinsta.cloud/guidelines-for-avoiding-gluten-unsafe-ingredients-for-gluten-sensitivity/
All the best,
Dr. Osborne
I am currently going through an ordeal of blisters and cankers on my inner lips upper and lower as well as inflammation of my tongue. I have been Celiac for 15 years but have had mouth issues for 3 months bouncing back between Dr. And dentist. Now referred to oral surgeon, didn’t make the connection to gluten until now , thanks.
A stomach specialist will be more than happy to do the he tests on you for gluten not a plain MD ,unless for insurance you need referrals I have full blown Celia disease for about6 yrs diagnosed, and continue getting not mouth sores but outside in the ends, cracks, of my lips , I’ll try the green juice idea. Ty! Nice web sight!
That is called angular chelitis. It is b vitamin deficiency and/or fungal. All related to gluten.
Also check for leaky gut to make sure your food intolerance isn’t beyond gluten. Gluten can be a huge gut destroyer or aid in its destruction. Once leaky gut comes even other foods can cause mouth sores, acne, body pain, etc. Get an igg test done. Very helpful. And l-glutamine also helps in healing the gut from the years of inflammation from gluten/foods,medicines,stress…
I have celiac disease and was wondering if I should be concerned if a product says it is Gluten-free, but then it states it is processed in a facility that uses or process wheat?
I have carefully pinpointed that I get canker sores from Gluten. Bread or Beer – I’m certain of it.
Like others commenting on here I suffered with painful mouth ulcers periodically throughout my life. Since commencing on a mostly gluten free diet 6 years ago, I have been free of this scourge.
I had canker sores in my mouth for years, actually as long I remember… it got to become extremely painful for las 3 years. Doctors did all types of tests trying to figured out and everything came negative. I had painful legs and extrem fatigue. I decide to go to a Naturalist Doctor. They order a blood test and then we had an appointment to follow up. The test came posive allergy for gluten and casein. So I eliminated it from my diet….
The wonderful suprising positive side effects… No more cankers sores in my mouth, no more migraines, no more big belly bloating, no more painful legs. I had no idea all this “problems-sicknes” that the Doctor had put several names, was just a reaction from my allergies.
Interesting that gluten causing canker sores. Being highly sensitive to corn even a strict gf diet I am now looking at my toothpaste containing hidden corn. Any suggestions would be appreciated. Even brands that have no corn?