The incidence of people suffering with asthma in the U.S. continues to grow. Interestingly enough, so does the incidence of people being diagnosed with gluten intolerance. Because asthma can be an autoimmune reaction, the next question is – Are the two related?
According to a new study in the Journal of Allergy and Clinical Immunology, there is a strong correlation.
Contents
ToggleSource:
Journal of Allergy and Clinical Immunology. 127, Issue 4, April 2011, Pages 1071-1073.

Baker’s Asthma
Baker’s Asthma dates back to an observation from 1700. Bakers exposed to large amounts of flour dust suffered respiratory symptoms that mimicked asthma. This was the first known historical connection between grain inducing asthma. The reaction was later discovered to be an IgE response. IgE is an acute antibody produced by the body’s immune system. The antibody causes the release of immune chemicals called histamines. These histamines are responsible for the shortness of breath, wheezing, coughing, and other allergy symptoms.
For a complete comprehensive breakdown on the relationship between gluten sensitivity, celiac disease, and asthma, read this.
Asthma is Extremely Common and on The Rise
According to EPA statistics, approximately 8% of the U.S. population have asthma. The common thought is that asthma is caused by genetics, airborne allergies, and the over emphasis of hygiene (hygiene hypothesis).
The common medical solution is the use of steroid inhalers, and immune suppressing allergy medications. Many patients are told that the asthma is something they will have to medicate for the rest of their lives. The downside to this – chronic steroid use causes vitamin and mineral deficiency, bone loss, and contributes to diabetes. Allergy medications increase the risk for infection and reduce the immune systems ability to fight pathogenic invaders.
Skin Testing for Allergies is Limited and Incomplete & Misleading
Many doctors perform skin testing for environmental allergies like dust, mold, pollen, etc. Unfortunately, food allergies are rarely looked at as a cause for asthma. If they are investigated, they are usually limited to wheat, soy, peanut, and milk. Measuring wheat allergy is not the same thing as checking for gluten sensitivity. This leads to a lot of confusion among patients. Additionally, skin testing can yield false negative results. Even more unfortunate is the fact that skin testing only measures one type of antibody. There are four more antibodies that contribute to allergy reactions. See the diagram below for more information on this.
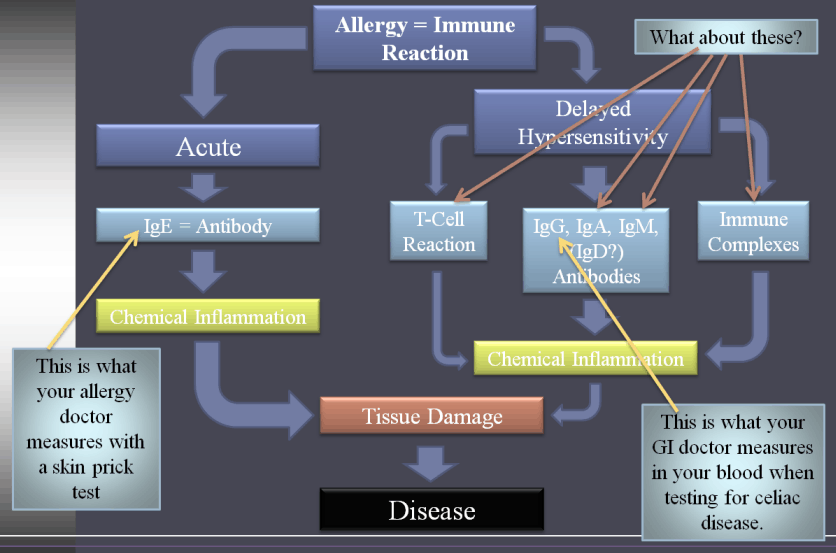
Gluten Free Diet Commonly Improves Asthma
In my practice, I commonly see patients who have been previously diagnosed with asthma. After identifying gluten sensitivity and/or other food allergies with genetic lab testing, these patients always show dramatic improvement. As a matter of fact, for most of them, medication becomes unnecessary.
These patients’ immune systems are so busy fighting their food, that they don’t have left over immune resources to fight the environment. Add to that the fact that gluten can induce inflammation in the lung tissue.
With more than 20 million cases of asthma, an estimated 30 million people with gluten sensitivity, and an estimated 1 million with people with celiac disease, wouldn’t it be prudent to investigate the possibility of an overlap? Shouldn’t doctors test for gluten sensitivity as a standard part of practice for every patient with asthma?
Know someone who could benefit from this article? Share it…
In good health,
Dr. Osborne – The Gluten Free Warrior







42 Responses
According to the World Health Organization study done just a few years ago linked the #1 cause of asthma to Fungi. 39% of US homes and close to 70% of schools in the US have mold. Also considering that wheat and anything else thats been stored in a silo tests for mold and aflatoxins. The spores that are breathed in are also carried into the gut and small intestine with the mucus. So the big connection is mold!!!
Oh yeah, there IS a link between gluten and asthma. My daughter and I both used to suffer from asthma. She was on 4 different medications and now she is off 3 medications and we are weaning her off the last one. Her health is SO much better after she became gluten free! Mine too!
I have had uncontrolled asthma for years and have seen Dr.’s at National Jewish Respiratory Hospital and other Dr.’s for second opinions and treatment for 7+ years. After numerous trials of different meds, every type of breathing test imaginable, etc., my condition had worsened to the point that I could not live a normal life. Although NJ is considered one of the “BEST” respiratory hospitals in the US, they disgregarded my questions about leaky gut syndrome and my constant comments about direct relationships to eating foods and asthma symptoms. The problem was that the list was growing longer almost DAILY. I was told that they do not deal with food sensitivities because it would open up a “whole can of worms”. In the past few months, my problems had grown exponentially worse and I was feeling VERY desperate and scared. I had cut wheat gluten from my diet years ago for neruo symptoms with great success, but not ALL gluten. Recently, after reading about all forms of gluten and how it might help to remove them from my diet, I did so. My asthma has improved dramatically in the past week since I cut out rice (once tolerated) corn, amaranth and other forms of gluten besides wheat. The results are amazing! I have not had to use my nebulizer in days which is HUGE for me. I am not using my rescue inhaler numerous times per day, another “miracle” and have not needed prednisone in over a month. I feel as if my asthma is acutally going away or at least improving to the point that I can live with it. What a HUGE relief! Hopefully I will eventually be able to go off of the Symbicort and heal my body even further! Thank you so much for the information! After scouring Dr.’s in the mainstream medical community for years to help with my food sensitivities to no avail, this newsletter/website has literally changed my life!
Corn,rice and amaranth are not wheat
No, but they are carbs, which are proceeded the same way in the gut, therefore acting the same.
It’s the carbohydrates those items are still carbs like the wheat and that is the connection
The contain gluten, which is the point of this article.
Fantastic.
Great to hear of your success. I have come off my inhalers which I have been on for thirty years. I know gluten and lactose make me ill, so I am now more strict in avoiding these foods.
Your post gives me hope.
Great to hear the connection between asthma and gluten is now being recognised. I had asthmatic symptoms for 15 years which gradually became worse leading to numerous stubborn chest infections. Having tried everything to help myself, I eventually had food intolerance testing carried out which showed that I was intolerant to gluten, wheat, dairy and eggs. Much to my chest specialists horror, I cut these foods out of my diet rather than opting for strong steroid medication (the consultant assured me that it would not help and that I would make myself more ill). My symptoms did worsen as my body went through an intensive detoxification process over a period of a few weeks before improvements in my health began to show. That was over four years ago and I have not had any problems with my health or asthmatic symptoms since. I have remained gluten, wheat, dairy and egg free in my diet but there have been a few occassions over the past few years where I have had wheat/gluten in foods without realising and within 5/10 minutes the wheezing, coughing and breathlessness returns so I have no doubt that for me, wheat/gluten was directly responsible for my asthmatic symptoms. I only hope the medical profession begins to waken up to this connection rather than filling people with medications that may alleviate symptoms but do not treat the underlying cause of the illness and which undoubtedly create other problems due to the side effects of the medication.
I am a music teacher and choir director who has had asthma off and on for many years. It has gotten much worse in the last three years. My doctors told me that I have allergies but, after allergy testing, they could not find a true trigger allergen. They then told me that I had acid reflux disease. After months of acid reducers my asthma did not get any better. They now call my disease “Asthma of Undetermined Origin.” I am continually being placed on doses of antibiotics, oral steroids, inhaled steroids (Flovent) and albuterol treatments.
Life has become extremely miserable for me. Asthma effects every aspect of my life, from sleeping to the workplace. My wheezing and coughing keep me up at night. Because of that, I have been struggling to stay awake when I drive.
The doctors have told me that I will have to deal with my asthma condition for the rest of my life. There is nothing more that they can do. This is totally unacceptable to me. Recently I have been searching the internet for a possible cause and cure to my condition. I have begun to suspect that gluten is the culprit of my disease. Has anyone gone through the same thing as I have? Does anyone have any suggestions for me? I would surely appreciate some advice.
Richard
I was exactly the same as you up to 6 months ago. Doctors could not do anymore. I cut out dairy, chocolate sugar and bad carbs I.e.bread. my energy increased. I started Pilate’s once a week to stretch and help my body get rid of toxins and increase blood flow. I cut out gluten nearly completely and I just do not know myself as I felt my quality of life had gone. Foods make a huge difference but fresh air is important each day. Good luck Marg Ireland
Hi Margaret I also live in Ireland, and suffer a lot from asthma and bronchitis and chest infections etc I’m looking for answers and how to get better. What do you eat now as a substitute for bread and do you go to like a mountainous area every day for fresh air or do you just breath outside of your house ? 🙂
Yes! Richard, we are pretty much identical in our struggle. I recently (December 2015) went on the Ketogenics diet. My symptoms have improved dramatically. I did have a few days that I ate some food containing Gluten & my symptoms returned. Try going on a very low carb/ gluten free diet. I’ve also lost 34 pounds in the process.
Correction:
I started December 2016 not 2015
I have exactly the same symptoms as you and like you have begun to realize that gluten was most probably the culprit. I removed gluten from my diet and started a water fast for 6 days to detox my body. The detox is incredible as it gets rid of all toxins including gluten! I was in the middle of an asthma crisis at the time and my Doctor said I was mad. By the end of 6 days I felt fantastic, not tired or fatigued on the least, great mental clarity, and completely asthma free. I am only on day 12 now so it is still to early to tell and eating only fresh veg and fruit with some organic meat. My asthma had escalated dramatically over the last year and I was doing prednisone twice a month. I have been asthmatic for 19 years and the symptoms have been escalating. I have seen countless doctors, specialists ,tried everything under the sun, acupuncture, herbs, and noting worked. In fact I was getting worse. During the fast I also stopped using my inhalers and was fine. You should do a gluten sensitivity test ,along with a dairy and egg tests. If you are liked me you will have many allergies. Good luck and cut out the gluten!
Yes. I was completely exhausted from wheezing and coughing nonstop. Found out I had a gluten allergy. Once I went on a gluten free diet, I got off inhalers and prednisone. However, I couldn’t resist eating whip cream today and regretting it! Gluten and lactose intolerance go hand in hand until you’ve been gluten free for a quite a while . At least that’s what I’ve researched it.
Yes when I went gluten free nine years ago after a biopsy of my small intestine confirmed advanced celiac disease I lost my asthma as well as my migraines and vertigo. When I ingest any trace of gluten by mistake my asthma returns. I eat no wheat rye barley or oats. I keep clean of cross-contamination from any utensils plates glasses that have come in contact with any gluten. I have systemic lupus and thyroid issues but the symptoms are much less since going gluten free. It took five years for my body to return to normal (I had had a seizure…was down to 98 pounds, was not sleeping…had rashes etc prior to being gluten free). When I am gluten free I feel good. I have to be very careful but it’s soooo worth it. My allergist did not test me for celiac I found it online due to my symptoms and asked for a test!!!
Awesome Jeanne!
Thanks for sharing your gluten free success story with us.
All the best,
Dr. Osborne – The Gluten Free Warrior
Over the years I’ve been labelled as ‘atopic’ – mild asthma, mild eczema, rhinitis (resulting in loss of sense of smell) and as I got older (now 43) developed lots of gut discomfort, bloating and constipation, brain fog and vertigo, slightly overweight and fatigued. A random blood test revealed borderline hypothyroidism. I went on holiday for first time in years with my sister who noted that my symptoms were very similar to her friend who had been diagnosed celiac. I decided to go gluten free. Within 1 week, the changes were enormous! All these ‘mild’ symptoms have slowly disappeared. After 3 weeks friends were beginning to notice I looked healthier, slimmer, bouncing with energy. Went to see GP to describe transformation and have had to go back on gluten to do celiac blood test- within 5 days back to snotty, itchy, lethargic state! Whatever blood result I will be going back to gluten free as soon as I can!
I just want to say, I agree with many whom have posted here, that gluten is related to asthma, wheezing, breathing difficulty symptoms. My 5 year old son started to get asthma symptoms 18 months ago. In the last 6 months it got worse, recurring only after cold/ cough symptoms and suffering every 6 weeks with it. He has had to be on ventolin inhalers, redipred steroids and nebuliser machines. In July (Winter here in New Zealand) we had a frightful visit by ambulance to hospital, with my son nearly losing consciousness due to very inadequate medical care and I became a nervous wreck after that. Determined to find a cure, without drugs. Finding only drugs from Doctors, I searched the net and went to a herbalist who recommended a herbal mixture, fish oil, more coconut oil, massage, breathing exersizes and gluten and dairy free diet. All this on top of the usual vitamin c powder and Echinacea that we had been taking. We also got my son onto colloidal silver. I told her If she told me to stand on my head and sing the alphabet, I would do anything to stop this terrible loss of breath condition. I did as she taught me straight away. I also cut out even more of sugar (even though we already had very little as I am aware of the destruction to health it causes. And I upped our coconut oil consumption, which is antiviral, anti fungal, anti bacterial and amazing for many health ailments, helping people in tropical locations stay the healthiest of humanity. But when my son got a skin ailment ( I suspect from the asthma drugs) a doctor told me to watch for allergies to coconut oil, lavender, tea tree oil and all herbs and it was better to have all drugs under the sun. When I asked her if the skin condition would benefit from gluten and dairy free diet, she told me skin conditions have nothing to do with our diet (yeah Righto) Lucky for years of experience and mis treatment in the medical society I now listen to natural doctors and my own intuition from my own experiences. I have read intensively of many ailments and I know that any symptom: cough, runny nose, runny stools, fever, skin rash, pain is your body asking for help and it is upset from the inside out, trying to get the upsetting foreign substances out. It is pretty simple. Anyway I really want to confirm that my son has not had any sign of asthma, not even a wheeze for 8 weeks now. Now we are in spring time and he has had many a cough and sniffle again (which in the last 18 months was always followed with wheezing and asthma symptoms) with no Asthma symptoms!!! I am so excited and really wanted to share this with others. Do not wait for a test!! Try an elimination diet, first no wheat and dairy for a month, then back on dairy and find out what makes you feel most alive and great. Our whole family of 6 feels better gluten and dairy free. Do not be put off by expensive gluten or dairy free products. We have a large family and another babe on the way, so we can not afford all the packaged convenience items. I make my own gluten free bread and almond/ nut milk, sugar free coconut cream ice cream, dairy free smoothies with coconut oil and we (as always have done) eat a good variety of vege, a lot home grown organic and our own grass raised organic beef. I urge you to investigate and listen to yourself, take your health into your own hands, and heal yourself. You are the only one with the wisdom to heal yourself.
To good health and happiness that we all deserve!!
I have respiratory arrested and been ventilated due to asthma. Was told by NJ I was allergic to animals (I am a vet). They never tested me for food. I was told to get rid of my pets and find a new profession. They gave me a prn rx for steroids and inhalers and an in invitation to their most invasive studies (thanks but I’ll skip having my airways scraped). 10 years of living on the meds later I accidentally discovered food as a trigger when I went off grains and dairy during a 3 week cleanse. This began my journey. So happy to find GFS. #glutenwarrior
I have recently been to my doctor to mention I may be intolerant to gluten and he is giving me a blood test and asked me to try gluten free for 30 days.
over the years I have had or been treated for the following:asthma, rhinitis, vertigo, constipation, Burping, wind, anaemia, shortness of breath, epilepsy, headaches, tiredness,thrush , water infections, daily periods, fast heartbeat, excess mucus. No one had ever put the symptoms together they had all been treated separately and none have every gone away. I have seen a dietician and she says I look gluten and lactose intolerant, she also sguested i may have a sugar imbalance and to drink 2 1/2 ltires of water a day. I am in to day 4. Already my excess wind and Bloating have gone and my stomach is flat. I can tell very quickly what isn’t agreeing with me such as my instant hot chocolate, sweet beetroot and cheese. Someone at work who’d been on holiday for a week even asked if I’d lost weight. I also showed her my daughters, sisters and mothers symptoms and she said there is often a genetic link which passes from mother to daughter. My sister suffers really bad Fibroneualgia. Hope this helps others who have been wondering which illness in the alphabet they were going to get next. I will keep you posted.
Glad to hear you are doing better!
Thanks for sharing your TRUE gluten free success story!
All the best,
Dr. Osborne
I know this was posted 2 months ago but if you still feel sick maybe you should try grain free, and not just gluten free.
I am just reading about this now. I am a severe asthmatic. I use 4 different pumps everyday. Also been on and off steriods for a long time for my Asthma. After reading G this article I will follow it and hope it will help. The life I lead now with my asthma is not a quality of life.
I’m 28. I’m a martial artist, and train up to 7 times a week.although I’ve had asthma since a young age, it hit hard the last couple years. There have been days where I feared going up the stairs. My quality of life has been greatly reduced, it has even effected my mental health at times.
I have been to specialists in Montreal and Quebec City. I’ve tried various drugs,( symbicor, singulair, Spiriva, alvesco, ect. With some success. For over a year i was on 8 puffs of symbicor a day! it seems however thay my condition depends on the weather. It gets the worst in the winter or when it’s humid after rainfall. I have allergies to dust and animals.
recently I went to see a chiropractor who did something called nrt, in order to test which foods may be effecting my lungs. He said wheat, gluten, corn, barley, malt…are the culprit and that I need to cut them out 100%..not even a crumb.
I am currently on week 2 of this diet. It is incredibly difficult as almost all gluten free products utalIe corn as a replacement for the wheat. Health foods charge a fortune for groceries. With thay said, I am learning with every day that passes. I have felt some improvement in my breathing and lost 8 pounda thus far, my face doesn’t look bloated, my energy has gone slightt up.
any advice for corn, wheat, gluten free food.
I was told that all red meat has barley in it unless the animal is grass fed. Is this true? Must I cut out meat as well to truly commit to this diet.
I would encourage you to follow you doctors advice and avoid all meat that is not grass fed. In my experience this is a major problem for many going gluten free. Avoid gluten free products. They are not healthy. They will not going to help you recover from extensive workouts. Remember, that to follow martial arts is to value your diet and food as a critical element in your training.
Stick with grass fed meats, wild fish, free range birds, vegetables, nuts, and fruit.
Let me know how you feel in a month afterward. You might also consider reading No Grain No Pain – it dives into much more detail than this post and might be very helpful on your journey.
Best,
Dr. Osborne
Read, “No Grain No Pain” and all your questions will be answered. The author creates a great roadmap to help transition to a gluten free diet and also points out hidden sources of triggers.
I had medication for asthma for over 30 years,inhalers and steroids the lot. After a period of increasing stomach and digestion problems and excessive wheezing I read an article on the web like this and decided to give a gluten free diet a go.
Within 3 months my asthma was effectively cured and other ailments have largely gone away. In my experience various tests are largely ineffective and the medics are uninterested in the connection which I find quite odd given it is a cost free way of curing this debilitating illness.
Your story is quite common Stephen. I wish more doctors would pay attention. Thanks so much for sharing. Your experience may give someone else the strength to go gluten free!
All the best,
Dr. O
I’ve had chronic asthma for many years….gradually getting worse. I Dr Googled and did research online and decided to give myself a Gluten Free 28 day trial. Well…..I’ve not had ‘itchy’ lungs. I’ve not been using my inhalers for the past week (or Montelukast tablets). I no longer have that annoying cough throughout the day and at night before I go to sleep (I used to take my Fostair inhaler just before bed, opening up my lungs and therefore initiating an annoying cough sequence before sleep). I’m eating more meat now (I prefer veggie, but something’s gotta give). But I’m just eating more paleo type stuff. I haven’t tried sipping an occasional single malt whisky yet… I so like not coughing, I’m frightened to try!!
Suffice it to say, I’m sticking with this lifestyle now. I feel better than I’ve done in some time (despite just having nasal surgery!!) I’d recommend a trial to anyone. Do it properly though, give it the four weeks and see what happens!!
I’m 37, and had allergies most of my adult life – sneezing, runny nose, watery/itchy eyes etc. The symptoms have changed over the last 2 years – wheezing and chest tightness and asthma attacks that gets you coughing.
I’ve been dairy free for 7 days and wheat free for about 4 days. My lungs are quite inflamed at the moment. How long do you think I need to stick with this regimen before noticing any difference ? I’m all for it, but want to know so I change my strategy if this doesn’t work.
Also do you think, while my gut repairs itself (i.e. still leaking), I could be allergic to other foods (that would not cause me problem if the gut was healthy) during this period?
I could run 10k in 50 minutes and now I get out of breath walking – in just 1 year. Any comments appreciated.
The HLA-DQB1 gene is associated with atypical celiac disease and asthma. Add an allele or two and you can get things like narcolepsy, peanut allergy.
At 65 I have been gluten free for six years. I actually love eating this way now. My lifelong asthma is totally gone. My vitamin D levels are normal. My CRP (inflammation) levels are low. My once inflamed thyroid is normal. As long as I am religiously gluten free, my skin rashes are gone. (My skin is my first indication of gluten exposure now.)
Eating gluten free is much easier than it was in the past. If you have health issues, not just stomach issues, just give it a try. You have nothing to lose and good health to gain.
I have recently developed asthma and I’m 63. Have not smoked or drank alcohol since I was 28 but have had 2 bouts with pneumonia. I would like to go gluten and dairy free. But I am unsure of which foods contain gluten. Also I use yogurt with live bacterial culture which helps my digestion as well as a substitute for oily salad dressings which upset my stomach. I also rarely eat red meat but eat store bought chicken and fish. I would appreciate any helpful advice. I also have irritable bowel syndrome and fibromyalgia.
I sure appreciate the info provided on this site. Blessings, Rae
Hi Rae,
two things:
1. Check out this page. It contains a list of gluten and the hidden terms commonly used for gluten on food labels.
2. Follow the 30 diet protocol in No Grain No Pain.
Let me know how you do.
All the best,
Dr. Osborne
This article has made it all so clear to me. I ‘ve had asthma for 4 years now and recently had the worst flare up due to being exposed to smoke from a fire pit during a family gathering. I was having a really hard time for over 5 weeks with heavy chest and even anxiety because I couldn’t breath. I was and still am on steroids (nasal spray, inhaler) and allergy medicine. Some days I was feeling I was doing better and others I was feeling miserable. An additional inhaler was prescribed which made me feel better but still some nights I had to use the nebulizer. I’ve been vegan for a few months now so I decided to cut out gluten from my diet less than a week ago. I thought it was the last inflammatory food I haven’t cut out so it was worth giving it a try. It’s been almost a week since I did that and the heavy chest has gone away. It’s amazing how after 36 hrs of taking gluten out of my diet I’ve felt so much better. The difference feels like night and day. I’m still using the inhalers and nasal spray but my doctor has now reduced the dosage of one of them because my numbers have improved (breathing test). I’m so glad I found this article which corroborates the idea I had about inflammatory foods. Thank you for posting it and thanks to all the people who have shared their experiences. Hope you can find your own answers to heal your body.
The comments on this subject make me feel better. I have been on asthma medicines for many years with reasonable but not always good success. Recently I have been diagnosed with celiac and now cannot eat a crumb of gluten without a reaction. One good thing, getting gluten out of my diet definitely helps my asthma!
I have severe asma for 35 years (I am 41 y o) I take Symbicort every single day for the last 10 years. Since I am on a gluten free diet no more asma, and corticoides…. I am happy than ever.
I miss the bread but there is no more asma atacks
How do you know you don’t have anymore asthma?
I have severe persistent asthma and allergies I am on breo and I’m not sure if it is working. I feel a burning like inside my chest and lungs. I also have gerd so I am not sure what could be causing the burning sensation inside my lungs after I take the inhaler. I have been told I need to go gluten free and dairy free and avoid yeast due to my blood type as o+. Does going gluten free really help that?
Yes! Yes! A thousand times yes it works!