Contents
ToggleShould We Generically Recommend Calcium For Bone Loss?
High doses of calcium are commonly prescribed for patients with osteoporosis. This recommendation is fundamentally flawed for many reasons. Keep reading to learn why…
A research report in the New England Journal of Medicine identifies antibodies against osteoprotegerin (a protein that prevents bone breakdown) in several patients with celiac disease. This protein is responsible for helping maintain bone density. When it is attacked by the body’s immune system, bone loss becomes accelerated leading to osteoporosis.
Source:
N Engl J Med 2009;361:1459-65.
Bone Loss is a Complex Process
It is a common thought that osteoporosis associated with celiac disease is a result of malabsorption of vitamins and minerals (mainly vitamin D and calcium). The above report links an autoimmune process of bone loss to gluten sensitivity separate and distinct from gluten induced malabsorption. This finding begs us to ask the questions – Is Osteoporosis an autoimmune process? Should all patients with bone loss be assessed for gluten sensitivity?
Why is this an important link?
If osteoporosis has an autoimmune component, then we have to go back and look at gluten as a potential cause as it is the only known cause for any of the autoimmune diseases. That means that everyone with osteoporosis should potentially be screened for gluten sensitivity. Additionally, we have to consider the possibility that osteoporosis is another manifestation of the “gluten syndrome” AKA – non-celiac gluten sensitivity.
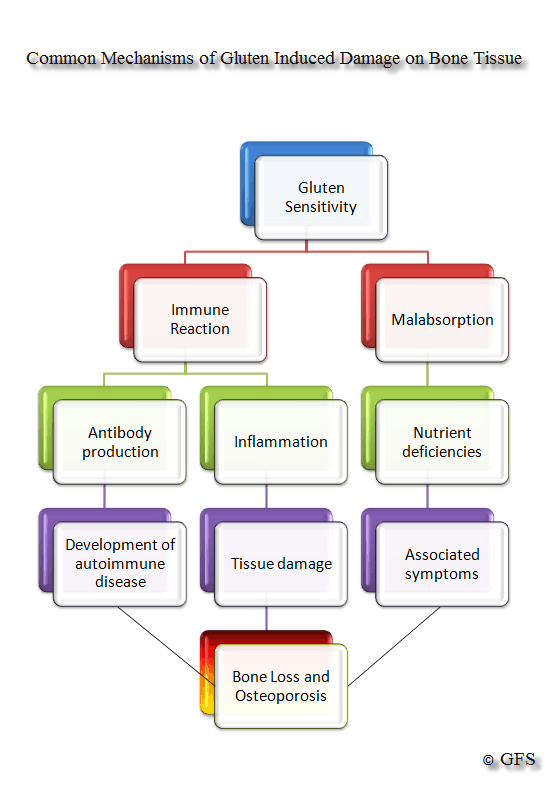
Very few are aware of the field of research called Osteoimmunology. This relatively new field of research explores the connection between a healthy immune system and bone tissue. It has been well established that many immune system derived chemicals help regulate inflammation, bone cell growth, bone resorption, and more. That being said, we know that gluten can cause a dysfunctional immune system leading to a host of different immune chemical reactions that have negative impacts on human health (especially bone health).
The diagram below displays some common effects gluten can have on bone:
Supplementing with High Doses of Vitamin D and Calcium Not the Answer…
Most doctors generically recommend high doses of calcium mixed with vitamin D as part of the treatment component to patients with osteopenia or osteoporosis. This recommendation is fundamentally flawed because bone is a dynamic structure that is made up of multiple minerals under the direction of hormones and co-enzymes (vitamins). Vitamin D and calcium are only 2 pieces of a very dynamic puzzle.
Those diagnosed with bone loss should have their vitamin and mineral levels tested specifically. This allows targeted supplementation as opposed to guess work on the part of the doctor or patient. This unique individual targeting allows for a specific food/supplemental protocol to help maximize and optimize bone growth potential.
Getting Calcium and Vitamin D From Dairy
Another common bad recommendation for those with gluten induced bone disease is to increase the intake of fortified dairy products. There are a number of problems with milk, cheese, yogurt, butter, and other dairy products produced in the U.S. One of the biggest – the cows are fed genetically modified grains high in gluten in order to keep up with milking demands. Additionally, the use of hormones to enhance milk production can be very problematic to human health. Some research has also identified similarities in the protein casein. This milk based protein has been shown to resemble gluten and contribute to a number of medical conditions. If you have ever come across the term – gluten free/casein free diet, you are probably aware of this connection. There is a large body of evidence suggesting that children with developmental disorders like autism show marked improvement when removing dairy and gluten from the diet. The take away here is simply this – don’t assume that dairy is as healthy as TV has led you to believe.
Don’t Forget Weight Bearing Exercise
Often times one of the biggest missing components to rebuilding bone tissue is resistance exercise. Keep in mind that we define walking as movement, not as a form of resistance exercise. Walking is not enough to restore bone health. The following exercise are considered very effective to build muscle and bone tissue without the need for expensive gym equipment:
- Push ups
- Pullups
- Situps
- Squats
- Lunges





3 Responses
Hello and thanks for this.
Well I never had the test for gluten sensitivity but here’s my story,
I’ve had IBS as long as i can remember and during that time i used to smoke. I ate white bread and all products containing gluten with no difference in symptoms of any other foods.
I stopped smoking 4 months ago and I’ve noticed that my diet had to change, and the first thing that i noticed was that white bread/pastries made me really irritable, of course through the first month i was expecting to feel so as i stopped smoking. After the second month (through this period I was eating whole grain bread and cheerios :D) I couldn’t really tell if i had sensitivity really as i referred every symptom i go through to quitting smoking. but it’s been 4 months now! and I’m not sure but i’ve noticed that when i eat pastries even small amounts i would be okay the first day, but afterwards i would be sick for more than 4 days! this includes anxiety, depression and very bad mood in addition to GERD to which of course doctors would do all tests and say “nothing is wrong with you, you’re perfectly healthy” and give me stuff like Zantac and Nexium and those two drugs really made me more anxious and irritated not to mention depression and feeling that i’m going crazy. I stopped Zantac the 4th day and on the other occasion i stopped Nexium after 2 days!
Could it be Gloten sensitivity that is causing GERD for a period of time after i eat gluten?
I am looking for the girl, the fotographer, who started repigmenting after going gluten free.
Excellent video that addresses Ramzi’s question, and great, indepth info on gluten issues. We are learning soooo much!
I just found this in the last several weeks… the best I’ve found.
http://www.glutenology.net/glutenology-health-matrix-free-video/